17 The integumentary system
Desquamation: The process by which dead cells are shed at a fairly constant rate.
Dermis: Corium, or the second layer of the skin.
Epidermis: Multilayered outer covering of the skin.
Frostbite: Trauma caused by the crystallization of tissue fluids in the skin or subcutaneous tissue.
Integumentary system anatomy
The skin, or integument, provides a boundary between the internal and external environments of the body. With aging, the skin becomes thinnerwith less elasticity and diminished collagen. There is less inflammatory response and integumentary immunity protection with aging. Skin generally accounts for about 15% of the total body weight. The skin is divided into two major layers: the epidermis and the dermis, which includes the hypodermis (Fig. 17-1). Depending on location, skin varies in number of layers and thickness. The soles of the feet and palms of the hands have the thickest skin (approximately 1.5 mm) and have five layers. Eyelids have the thinnest skin (approximately 0.10 mm) and have four layers.
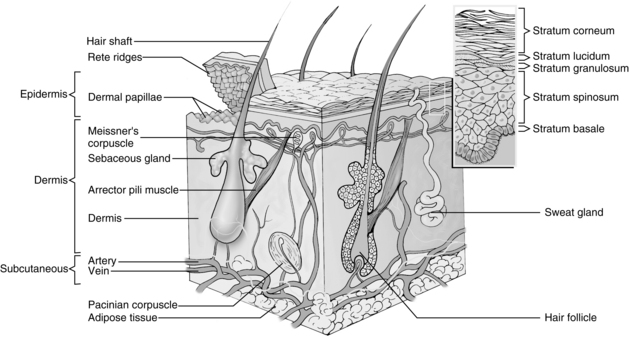
FIG. 17-1 Layers of epidermis.
(From Monahan FD, et al: Medical-surgical nursing health and illness perspectives, ed 8, St. Louis, 2007, Mosby.)
Hypodermis
The hypodermis functions as a shock absorber and heat insulator. Located under the dermis, it comprises fat, smooth muscle, and adipocytes. These cells store and accumulate necessary fats. The hypodermis acts as a site of energy production, and insulation. This area of the body stores fat in characteristic locations: hips on women, abdomen in men.2
Integumentary functions
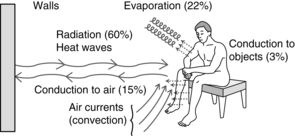
Thermoregulation
Skin, subcutaneous tissue, and fat in the subcutaneous tissue provide heat insulation for the body. Heat is lost from the body to the surroundings by radiation, conduction, convection, and evaporation (Fig. 17-2). Radiation of heat from the body accounts for approximately 60% of the total heat loss. In this mechanism, heat is lost in the form of infrared heat waves. Conduction of heat to objects represents approximately 3% of the total heat loss, whereas conduction of heat to the air represents approximately 15% of the total heat loss. When water is carried away from the skin by air currents, convection of heat occurs. Evaporation constitutes approximately 22% of the heat loss. Even without sweating, water still evaporates from the skin and the lungs; this is called insensible loss and totals approximately 600 mL/day.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree