30 Assessment and management of the airway
Airway Obstruction: A mechanical impediment to the delivery of air to the lungs or to the absorption of oxygen in the lungs.
Auscultate: To listen, most commonly with a stethoscope, for sounds within the body to aid in assessment of the frequency, intensity, duration, and quality of sounds.
Blind Nasotracheal Intubation: Nasotracheal intubation performed without the use of a laryngoscope.
Cricothyrotomy: A puncture through the cricothyroid membrane with a large-bore cricothyrotomy catheter or large-bore intravenous catheter for immediate access to the airway.
Extubate: The removal of an endotracheal or nasotracheal tube from the trachea.
Laryngoscopy: Use of a laryngoscope to view the anatomy of the larynx.
Laryngospasm: An involuntary, spasmodic closure of the vocal cords of the larynx.
Nasopharyngeal Airway: A device, usually a flexible tube, placed through the nares to create an air passage between the nose and the nasopharynx.
Nasotracheal Intubation: Insertion of a breathing tube through the nose into the trachea for facilitation of a patent airway.
Oropharyngeal Airway: A device placed in the oropharynx to conduct air or gases into the trachea; commonly referred to as an oral airway.
Oropharynx: One of three anatomic components of the pharynx; it extends behind the mouth from the soft palate to directly above the hyoid bone. The oropharynx contains the palatine and lingual tonsils and lies between the nasopharynx and the laryngopharynx.
Orotracheal Intubation: The insertion of a breathing tube through the mouth into the trachea for facilitation of a patent airway.
Sellick Maneuver: Also referred to as cricoid pressure, it is the application of external pressure to the cricoid bone before and during laryngoscopy in an effort to compress the esophagus, preventing regurgitation through the esophagus during intubation of the trachea.
Tracheostomy: An opening through the neck into the trachea that provides a conduit for the placement of an indwelling tube to establish a patent airway.
Airway management is a fundamental skill essential to all personnel in perianesthesia nursing. Airway assessment and airway management are crucial for providing safe and effective care to patients after surgery. As these vulnerable patients enter the postanesthesia care unit (PACU), they are extremely susceptible to many events that can compromise ventilation and adequate oxygenation of vital body tissues. Of particular concern are the residual effects of many potent and potentially life-threatening medications given by anesthesia personnel during the intraoperative period. These medications include, but are not limited to, opioids, sedatives, hypnotics, inhalational gases, neuromuscular blockers, insulin, intravenous fluids, and blood products. In addition, predisposing factors have the potential to affect the patency of the postsurgical airway. These factors include histories of obstructive sleep apnea, obesity, snoring, smoking, asthma, and ear, nose, and throat surgery and neck surgery.1 Anticipation and early recognition of respiratory distress coupled with adequate airway assessment and management skills are paramount in assuring the best possible patient outcome.
Airway management
Patients arrive in the PACU still experiencing the depressant effects of anesthesia. They may be obtunded, which renders them unable to maintain their own airway. Loss of important airway reflexes soon leads to airway obstruction. In some instances, the obtunded patient’s tongue and epiglottis fall back on the posterior pharyngeal wall, further occluding the airway. Indications of airway obstruction include increased respiratory effort, retraction of the muscles of respiration, a rocking chest motion, abnormal or absent breath sounds, cyanosis, and signs associated with hypoxemia and hypercarbia.2 Upon recognizing an airway obstruction, the nurse should place the patient supine, position a pillow beneath the head, tilt the head backward, and extend the neck, unless contraindicated. The nurse should then lift the lower jaw upward using moderate pressure (Fig. 30-1). Often this maneuver is all that is necessary for spontaneous respiratory effort to be effective. If the airway obstruction does not clear, the oral cavity should be inspected for foreign material and the oral pharynx should be suctioned if necessary. If large particles are present, the nurse should turn the patient’s head to the side and remove the particles manually.3
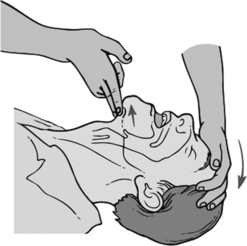
FIG. 30-1 Opening of airway with head-chin-lift maneuver.
(From Lewis S, et al: Medical-surgical nursing: assessment and management of clinical problems, ed 8, St. Louis, 2011, Mosby.)
If spontaneous respiratory effort is absent, positive pressure breathing must be initiated. A bag-mask unit that is connected to an oxygen source should be used. The requirements for a bag-mask unit are addressed in Box 30-1.3 For optimal airway management, the perianesthesia nurse should be positioned behind the patient’s head. The mask should be securely placed over the patient’s mouth and nose with the neck extended. The lower jaw should be lifted at its angle with the other fingers of the hand holding the mask. The thumb of that hand should be placed at the top of the mask. Moderate downward pressure provides compression over the bridge of the nose and reduces air leaks (Fig. 30-2).
BOX 30-1 Requirements for Bag-Mask Unit
• Self-refilling but without sponge rubber inside
• Nonjam valve system at 15 L/min oxygen inlet flow
• Transparent plastic face mask with an air-filled or contoured resilient cuff
• Standard 15-mm inside/22-mm outside diameter fittings
• No pop-off valve, except in pediatric models
• System for delivery of high concentrations of oxygen through an ancillary oxygen outlet at the back of the bag or via an oxygen reservoir
• Availability of adult and pediatric sizes
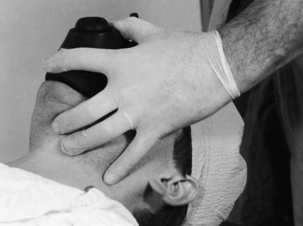
FIG. 30-2 Holding of mask with one hand.
(From Miller R, et al: Miller’s anesthesia, ed 7, Philadelphia, 2010, Churchill Livingstone.)
After the mask is properly placed, ventilation of the patient’s lungs should be attempted. While the perianesthesia nurse is ventilating the lungs, an assistant should auscultate the chest and assess the quality of breath sounds. If an assistant is unavailable, the perianesthesia nurse should check to determine whether the chest rises with inspiration and falls with expiration. This observation is merely a crude estimate of ventilation.4 If breath sounds are not audible during auscultation, or if the crude estimate of ventilation is inconclusive, an appropriately sized oropharyngeal airway should be inserted and bag-valve-mask ventilation should be resumed (Fig. 30-3). The oral airway is noxious to conscious or lightly sedated patients and should be used with extreme caution in this population.5 The untoward consequences associated with inappropriate use of the oral airway include bradycardia, retching, vomiting, and laryngospasm.6
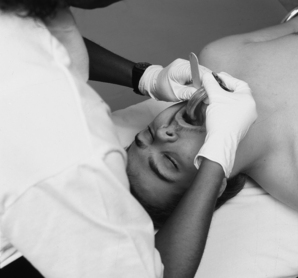
FIG. 30-3 Insertion of oral airway. Airway is inserted with use of tongue blade to displace tongue forward.
(From Sanders MJ: Mosby’s paramedic textbook, ed 3, St. Louis, 2007, Mosby.)
The oropharyngeal airway relieves an airway obstruction by providing a mechanical conduit for air to pass between the base of the tongue and the posterior oropharynx.3 For placement of an oropharyngeal airway, the perianesthesia nurse should first open the patient’s mouth with the right hand and place a tongue blade toward the posterior aspect of the tongue with the left hand. Slight pressure should then be applied to draw the tongue forward. With the oropharyngeal airway held in the right hand, the nurse should slip the airway in over the tongue blade into the oropharynx. The airway should not be twisted or forced into place, and placement should be accomplished quickly with careful avoidance of trauma to the soft tissue and teeth.
In comparison with the oropharyngeal airway, the nasopharyngeal airway is less stimulating to the irritant receptors in the upper airway, especially in awake or lightly sedated patients.7 The nasopharyngeal airway should be lubricated with a local anesthetic water-soluble lubricant, such as 1% lidocaine gel or ointment, and gently passed with the right hand through the nostril along the curvature of the nasopharynx into the oropharynx. The nasopharyngeal airway should never be forced. If resistance is encountered on placement, the other nostril should be considered unless otherwise indicated. When positioned properly, the nasopharyngeal airway should rest between the base of the tongue and the posterior pharyngeal wall.7 This airway should not be used in a patient with a nasal-septal deformity, a leakage of cerebrospinal fluid from the nose, or a coagulation disorder.6
After the oropharyngeal or the nasopharyngeal airways has been placed properly, ventilation should be attempted. Assessment of ventilatory effort should be continuous. With insertion of the oropharyngeal airway, the airway obstruction often clears. In this instance, the patient should be given a breath via the bag-valve-mask unit to assist with the spontaneous ventilatory effort and to help with removal of accumulated carbon dioxide. If apnea persists, positive-pressure breathing should be initiated via bag-mask with adequate tidal volumes. For a normal healthy adult, the perianesthesia nurse should consider tidal volumes of 8 to 12 mL/kg at a rate of 12 to 14 breaths/min as initial settings. For prevention of oxygen delivery into the stomach, pressure on the bag-mask device should not exceed 25 cm H2O.6
Intubation of the trachea
Intubation of the trachea is a proficiency reserved for only those nursing personnel with advanced airway management training and who are properly credentialed to intubate. Nurses should be familiar with their states’ Nurse Practice Acts as well as their hospitals’ policies regarding intubation privileges. The perianesthesia nurse should be familiar with the technique of intubation and capable of performing it quickly and efficiently should it be necessary and if it is in his or her scope of practice to do so. Airway management skills, such as endotracheal intubation, can be developed in the operating room setting under the mentorship of a certified registered nurse anesthetist or a physician anesthesiologist. With the same mentor, the perianesthesia nurse should continue to practice intubation skills on a monthly basis in the operating room. In an airway emergency, the properly trained perianesthesia nurse should intubate the trachea if ventilation of the patient’s lungs is unsuccessful. Endotracheal intubation indicates the placement of an endotracheal tube directly into the trachea. When the endotracheal tube is placed through the mouth, the method is called orotracheal intubation. When the endotracheal tube is placed through the nose, the method is called nasotracheal intubation. Other indications for endotracheal intubation in the PACU include the inability of the patient to protect the airway, prolonged mechanical ventilation, and cardiac and respiratory arrest.8
Equipment for endotracheal intubation
Adult and pediatric intubation equipment should be kept in the PACU at all times. This equipment should be inspected daily and after each use for proper functioning. For a list of the suggested airway management items to be kept in the PACU, see Box 30-2. Table 30-1 shows the recommended sizes for endotracheal tubes given the patient demographic. The formula age / 4 + 4 may be used as a guide when preparing endotracheal tubes for pediatric patients.9 For example, a size 5.0 mm endotracheal tube may be prepared for a 4-year-old child. Because of their importance, the laryngoscope and endotracheal tubes are discussed in detail.
BOX 30-2 Suggested Equipment for PACU Pediatric and Adult Airway Management Carts
Pediatric endotracheal equipment
• No. 2 Macintosh curved blade
• No. 1 and No. 2 Miller straight blades
• Assorted pediatric oral airways
• Pediatric masks of various sizes
• Empty 5-mL syringe for inflation of an endotracheal tube cuff
• Reverse-angle endotracheal tubes
• Endotracheal and oral suction catheters
• Tape for securing endotracheal tube
Adult endotracheal equipment
• Sterile gauze with topical water-soluble lubricant
• Sizes 6-mm through 9-mm cuffed tracheal tubes
• Endotracheal and oral suction catheters
• Tape for securing endotracheal tube
• 10-mL syringe for inflation of the endotracheal tube cuff
• Tongue blades for airway insertion
• Assorted-sized oropharyngeal airways
Table 30-1 Recommended Sizes for Endotracheal Tubes
| GROUP | INTERNAL DIAMETER (mm) |
|---|---|
| Pediatric | |
| Premature | 2.0 |
| Newborn | 2.5 |
| 6 months | 3.5 |
| 1 year | 4.0 |
| 2 years | 4.5 |
| 4 years | 5.0 |
| 6 years | 5.5 |
| 8 years | 6.0 |
| 10 years | 6.0-6.5 |
| 12 years | 6.5-7.0 |
| 14 years | 7.0-7.5 |
| Adult | |
| Female | 7.0-7.5 |
| Male | 7.5-8.0 |
Laryngoscope
The laryngoscope is used for visualization of the larynx and the anatomic structures in close proximity to the larynx (Fig. 30-4). The laryngoscope has two main parts: the handle and the blade. The handle holds the blade and houses batteries that provide electricity for the light on the side of the blade. The blade consists of three sections: the spatula, the flange, and the tip. The spatula can be straight or curved; it is the long main shaft of the blade. It compresses and moves the soft tissue of the lower jaw for facilitation of direct vision of the larynx.10 The flange, which is on the side of the spatula, deflects tissue that may obstruct the direct vision of the larynx. The tip, at the distal end of the spatula, is either curved or straight and serves to elevate the epiglottis, either directly or indirectly. The blade is attached to the handle at a connection called the hook-on fitting. The perianesthesia nurse is strongly encouraged to practice connecting the blade to the handle before using the laryngoscope in an emergency.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



