Taking Action
Setting Health Care in Its Social Context
, Interview with Ruth Watson Lubic byDiana J. Mason
“There is no doubt that it is around the family and the home that all the greatest virtues, the most dominating virtues of human society, are created, strengthened and maintained.”
—Winston Churchill
Ruth Watson Lubic, EdD, CNM, has been a pioneer in advancing new models of maternal and child health services in the United States. She founded and directed three childbearing centers: the nation’s first out-of-hospital birth center at the Maternity Center Association (now Childbirth Connections) on East 92nd Street in Manhattan, the Morris Heights Childbearing Center in the southwest Bronx, and the Family Health and Birth Center (FHBC) in northeast Washington, D.C. The first nurse recipient of the prestigious MacArthur Foundation Fellowship (so-called “Genius” Award), Dr. Lubic has dedicated her life to promoting the health of families, particularly ethnic minorities living in poor communities, through a model of empowerment.
She co-founded the American College of Nurse Midwives Foundation, the American Association of Birth Centers, and the Community Based Nurse-Midwifery Education Program Consortium for the distance education of new nurse-midwives. In 2001, she received the Gustav O. Lienhard Award from the Institute of Medicine for “pioneering work in the development of humane and innovative services for childbearing and childrearing families.”
In 2009, Diana Mason interviewed Dr. Lubic in her apartment in Washington, D.C., where she stays when she’s working—at the age of 83—as the interim general director of the FHBC. Her primary home is in New York City, where she lives with husband, Bill, a lawyer who plans to retire when she does.
DM: Ruth, you’ve dedicated your life to developing new models of childbirthing services. Why have we needed new models of care?
RL: Originally it was to try to provide young families who were disenchanted with in-hospital childbirthing experiences with what they were seeking to meet their needs. So we set up the first birth center demonstration project in New York in 1975. We tried to find out from them what it was that they didn’t like: They didn’t like being separated; they didn’t like the threat of the Caesarean section; they didn’t like having the baby taken away. Some hospitals had “rooming in,” but it was always somebody else’s house—it wasn’t their house. And so we thought we would see if home birth might meet their needs. But home birth is really expensive if you institutionalize it. If we had tried to set up a home birth service that was providing birth at home with New York City being as large as it is, we would have needed a number of midwives on call at one time. But Maternity Center had done that when it opened the first school of nurse midwifery in 1931. They had run it that way because they couldn’t run it any other way. They wanted to meet the needs of immigrant families, or poor families from the South who knew midwives and still believed that hospitals were places you go to die. A hospital had that “taint” on it. They had run that home birth service from 1931 until about 1958 or 1959. And it had gotten to the point where there weren’t enough people coming for home births anymore. I mean the idea of hospital birth had pretty much taken hold, especially after World War II; it became more institutionalized. The people that the midwives did see were largely affluent and could afford anything; they didn’t want to leave their homes, go to the hospital, and they wanted to be more in control.
I think that the control idea with childbearing is very important, because if a woman feels she’s in control of her birth—not meaning that she’s alone with her birth or that she’s dictating to professionals, but that her wishes are taken into consideration—that’s a preparation for motherhood that can’t really be imitated anywhere else. Let me just tell you an anecdote about when I had become a midwife and I went to work at Flower Fifth Avenue Hospital [in Manhattan]. There was no midwifery service there. So I was just teaching expectant parents part-time and working there. And I remember one time a woman coming up to me and saying—on the postpartum floor this is— “Can you tell me the name of the nurse who was with me during my labor?” And I said, “Well, I can find out. But why do you want to know?” She said, “Well, I think I bit her. I think that I was cursing her, but I’m not sure.” But she wanted to apologize to the nurse. The reason that that happened was because in those days, women were given usually Demerol and Scopolamine (Scopolamine being an amnesiac), so they would forget what happened in labor. Then they would be put in a bed with padded side rails raised because they were often not under control of themselves or their emotions, having been given those medications. So that to me was a real sadness that a woman would be thinking that she had behaved badly in labor, when labor is really a time for empowerment to take place. It’s not pain-free, but when you teach a woman how to manage the discomfort that she’s feeling and you assist her in doing that, and you encourage her, it’s a totally different experience.
Earlier in the day, Dr. Lubic had introduced Dr. Mason to Joan Brickhouse at the Family Health and Birth Center. Ms. Brickhouse gave birth at the Center and became a breastfeeding “peer counselor,” encouraging women to breastfeed and helping with problems and questions that may arise. The breastfeeding rate for women who deliver at the Center is 100%.
RL: Joan Brickhouse is a breastfeeding peer counselor. I took her with me when I went to testify in the capitol building. Representative Steve Cohen [D-TN] had brought people in from Memphis, from the large city hospital there, and they were talking about all their problems—you know, the numbers of deliveries and how many deliveries they had and how many babies went to the NICU and so forth. We listened to all of that. Then I got up and gave the statistics from the birth center, which were very different. Of course people looked at them, sort of with disbelief, because they were so different [from those of the Memphis hospital] and we had been able to reduce the disparities associated with birth so remarkably. So then I said, “But I would like you to meet one of our mothers, Joan Brickhouse.” Joan got up to the microphone and she said, “I wasn’t delivered. I gave birth.” The audience was blown away. That’s the way we want women to feel about the birth experience because that sets the tone for mothering. And if you enter mothering with that feeling of ‘I did something wrong’, ‘I wasn’t a nice girl,’ you know, and all that guilt that the use of drugs, and so forth, sets up in the hospital setting, then you’re going to be very uncertain of yourself where mothering is concerned. And of course, in the days where all those drugs were being used, fathers were excluded; so you didn’t have the support of your mate to advocate and assist you.
There is a difference between the midwifery approach and the obstetrical approach. Midwives feel that bearing a child is not just a medical situation, or a biological situation. It’s a situation that has important implications—social, emotional, and medical, true, but even religious and political implications. When I talk about that, I usually cite an example from the birth center that we started in the South Bronx. One woman who came from a Muslim country gave birth at the center, and people from her mosque came in afterward and formed a big circle in the reception area. It happened at night, although if it had happened in the daytime, we would have encouraged the same thing. The cultural dictate was for the baby to be passed around among mosque members. And each person spoke the words of Allah into the baby’s ear. So that’s an example of a religious dimension of child birth.
But, childbirth is also political. Moses was saved from Pharaoh’s wrath by the midwives who took him into the bulrushes and hid him because Pharaoh had dictated that all Hebrew males be killed.
And the empowerment—when we were on 92nd Street in New York, even though the families were empowered at the center, they were mostly middle-class, well-educated people. We had some racially mixed couples who felt themselves upwardly mobile. In other words, they weren’t low-income families who suffer from lack of self-esteem and depression because of where they live and their hopelessness that they can never get out of that. We went to the South Bronx to serve a low-income population because we felt that we could do a lot for their outcomes. At that time, the Bronx had the second highest infant mortality in the country, with only Washington, D.C., having worse outcomes. It was when we were in the Bronx that I really became aware of the empowerment factor, and how effective it was to do simple little things like have every women test her own urine, weigh herself, and write it on her chart—which she saw and she got the test results, and so forth. We really believed that it was her health, not our health. And we felt that every woman should have access to her chart. So, every woman did. When she came into the unit, she would pick her chart out of the chart drawer, and then she would begin doing her own self-care. Now, she did that with some oversight if she had any trouble. But when you treat women that way, you’re saying, “We think that you’re intelligent enough to do this; we think you have the ability, the interest to do this. And, we think you can do it.”
In coming down to Washington, I wanted to replicate this empowerment idea. And then coming here expanded into what it is now a collaborative effort. I looked for partners because we were not into being the “Golden Arches” of birth centers, in other words. There had been at least one obstetrician who came to us in New York wanting to franchise birth centers. We just wanted to set something up and have someone in the community keep it going as we had done in the Bronx where we formed a partnership between the Morris Heights Health Center and the Maternity Center Association. And we made it a good deal for them, in the sense that we said that if it’s successful, programmatically and fiscally, we will give it to you. And then we raised the money to renovate the space, and so forth. It was another demonstration project, and that center is operating today.
I came to Washington to replicate the birth center in the South Bronx. But when I got down here, I met with the woman who was running Healthy Babies Project at the time—Dolores Farr—which is a case management, home visiting, educational sort of organization. They were really surviving on donations and foundation grants. We partnered with Healthy Babies because they weren’t doing any clinical care and we needed to find a place to put these services. I had my stipend from the MacArthur Award, but we didn’t have any money other than that and we needed a building. But Dolores said, “Well, I know where there’s a building.” And she then took me to show me the building that we’re in today, which at the time was a derelict former Safeway supermarket. And when she showed it to me, it was sitting in the neighborhood, sort of at the top of a rise, and everyone coming out of the housing project behind it must have walked past it every day. I took a look at the size of it and exclaimed, “Oh, Dolores, we could have child care in there as well.” And we do.
Under the umbrella of the Developing Family Center, we have the Family Health and Birth Center, which does clinical care, maternity care, pediatrics, family planning, and well-women gynecology, and then we have the Healthy Babies project, which does the home visiting. They do a lot of education. For example, they have a program that is called Effective Black Parenting, which is a curriculum that came out of California. Right now they lost their funding for a fathers’ group called Developing Dads. And there’s Early Childhood Development in the building. Babies 6 weeks to 3 years can be cared for there. So it’s “one-stop shop,” as the saying goes. But more than that, it’s what we like to say: “It’s setting health care in its social context.”
We’re eager to get older women to come. Typically, older, low-income women don’t come in for care. And we did some focus groups on that. I spoke to women in the housing project behind us and said, “Look, we’re all women, I know what it’s like to be flat on my back with my legs in the air and it’s not fun. We’re gentle. We know what it feels like, and so forth. So, come and see us because there’s a high rate of cervical cancer and that sort of thing.” It turns out that because so often they are matriarchs in their families, the reason they don’t go for care, as they expressed it, is “if there’s something wrong with me, I don’t want to know about it.” It’s not typical of only low-income women. We meet women over all economic levels who have the sense that, “If I have cancer, I don’t want to find it. I don’t want to look for it.” So, we’re not doing as much “GYN-ing” as we like, although it’s improved a lot over the period of time that we’ve been there.
The pediatric nurse practitioners in the District can take care of young people up to age 21. But we don’t see many adolescents coming in for preconceptions. We see them mainly when they’re already known to be pregnant. And one of the reasons for that is that the pediatric rooms of which we have two are decorated for small children. So you can just see a strapping 16-year-old boy sitting in there amongst all the little animals, and so forth. One year as a community service, we did physicals on young men in nearby Spingarn High School, who were coming out for football. The coach said they were having trouble getting physical exams for the young men who didn’t have any coverage. So we said we would do physicals on them and we did. That year it was just a few, maybe four or five young men, and already one of them had hypertension. The life expectancy of black males in this ward of D.C., where we are—Ward 5—the last I heard it was 56 years, which is worse than Kenya. So, one of my favorite sayings is, “Come home, Bill Gates—there’s a little in your backyard that needs to be taken care of too!”
DM: So now you have this Family Health and Birth Center in Ward 5 of Washington, D.C. What are the clinical outcomes and financial outcomes?
RL: Well, we have been able to reduce the disparities among African Americans. In 2005, we were able to save over a million dollars because of lower preterm birth; lower low birth rate and lower Caesarean section. This was at a time when our operating expenses were $1,007,400. So we saved more money for the system than it cost us to operate, but we were unable to realize those savings because the savings all went to Medicaid and to managed care companies and their stockholders because they’re for-profit entities. This is a major weakness in the system.
We don’t know what our infant mortality rate is because we haven’t had the funds to follow the families to find out how many babies might die between 6 weeks and 1 year of age. So what we’re doing is estimating our infant mortality rate, although we never say what we think it is because we’re not sure. But the infant mortality rate would be dependent on these precursors to infant mortality, and preterm birth is the largest precursor. Preterm babies are born before 37 weeks of pregnancy. Low birth rate babies are born below 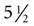 pounds, even though they may be 40 weeks of gestation. So there are two different approaches there. But when you do something that runs against the common thread, you’re always suspect. So the folks who have been doing it and getting poor results don’t have to explain what they’re doing, but those of us who are doing it and getting good results have to prove that we’re getting good results.
pounds, even though they may be 40 weeks of gestation. So there are two different approaches there. But when you do something that runs against the common thread, you’re always suspect. So the folks who have been doing it and getting poor results don’t have to explain what they’re doing, but those of us who are doing it and getting good results have to prove that we’re getting good results.
DM: There are about 200 birth centers across the country that provide a beginning infrastructure for making childbearing centers the frontline of maternity care. With the clinical and financial outcomes that you have, it’s stunning that you continue to have to do battle just to sustain childbearing centers financially, let alone promote them. What are the major barriers to being able to ramp this up and have it be the model for the country?
RL: From my point of view, the major barriers are that we are flying in the face of generally accepted patterns of care, for example, with organized medicine and hospitals.
DM: So over the years, you fought against organized medicine, which tried to claim that the outcomes for free-standing childbirthing centers and outcomes nurse-midwives in general were not comparable to outcomes from hospital-based deliveries and obstetricians. Now, recently, you’ve had the American College of Obstetrics and Gynecologists [ACOG] come out as supporting accredited childbirthing centers. Do you still have resistance from organized medicine?
RL: I think so, though we try to be friends. We try to reach out. But in terms of organized medicine, I have invited representatives of ACOG to come out and see us, and they’re always too busy. It’s very difficult not to have the impression that organized medicine would wish that we would go away, never bother them again. But my position is that the health care professions exist to improve the care of families. And if you’re not doing that, then you need to put your tail between your legs and go away.
DM: Now at the Family Health and Birth Center there is Linda Randolph, who plays a key role and she’s a physician.
RL: She’s actually the president of the umbrella organization, which is called the Developing Families Center. We wanted to be very sure that people understood that we were not physician-haters and that we welcome any kind of physician input into what we were doing, but that the opinions of the families mattered to us more than the opinions of organized medicine.
DM: You also, over the years, have fought the issue of reimbursement of services, payment of services. Maybe you can talk a minute about how that battle has gone. I remember back when you were at Maternity Center Association how you fought and fought to get Medicaid and Blue Cross Blue Shield reimbursement for deliveries. You were successful then. Do you still have issues with getting paid for services?
RL: At the Maternity Center Association in the early days, about 5% of our clients were eligible for Medicaid. So, it wasn’t a big deal, except it was an important policy issue. So we fought to get Medicaid reimbursement and we got it. In going to the Bronx, it’s a different deal because almost everybody was coved by Medicaid. And that’s true in Washington as well. But the Medicaid reimbursement is not always dependable, in the sense that Medicaid programs, after covering birth centers for their facilities fees [for overhead] for something like 22 years, withdrew that fee at the end of the Bush administration. It has since been restored under the Affordable Care Act, but it’s an example of hardball tactics that are not in the best interest of the nation; the facility fee that a birth center needs is perhaps a quarter of the facility fee that a hospital needs. And now, there is a bill in Congress to ensure that birth centers are paid a facility fee. It’s so poignant that the facility fee that a birth center gets is like a quarter of the facility fee that a hospital gets. So, suppose you don’t pay the birth center their facility fee. Suppose you make them close down, which I think some groups would like to see happen. You drive the women into hospital births, and the Medicare program has to pay 3 to 4 times what it would have paid if the women had been cared for in a birth center—to say nothing of her personal empowerment and her ability to mother. Then in 2008, it was withdrawn in South Carolina, Florida, Alaska, and the state of Washington.
DM: And the argument was that Medicaid bureaucrats realized that it wasn’t required by law to pay the fee to childbearing centers but it was for hospitals. So, that in itself is a lesson about the importance of having a policy that’s clear in statute and not relying on the kindness of strangers, if you will, who write or interpret regulations. Let me provide another frame for this and that is that it’s also about empowerment of women and families and providing really high-quality childbearing services and getting families off to a healthy start for the whole country.
RL: To me, you make the decision based on which system is most supportive to families. Because, I have to ask the question: How are we going to compete in a global economy if about 16% of our population is not able to realize its potential? And that’s what’s happening with the African-American community. Whatever health care is given should ensure the fact that African-American families feel capable of making health care decisions and implementing those health care decisions. And that’s what we’re all about. One of the things that my husband exhorts me about is you should not focus solely on low-income African-American families. What is happening is good for any American family, whether they’re low-income black, low-income Hispanic, or low-income anything; or whether they’re middle income; or whether they’re upper income even, because we know that people who have a high level of income don’t necessarily have important opportunities to strengthen their families.
DM: So if you were going to ensure that their childbirthing centers are a framework and part of the infrastructure of our health care system, we need to require a sustainable facility fee, but what else needs to happen from a policy perspective?
RL: I would like to see the United States of America take a position similar to that of France, which is “the protection of mothers and babies.” Not aid to, not assistance for, but protection of. It’s a whole different mindset. And so I work to try to affect that mindset, because to me it’s very important to the health and strength of the country. I think that it’s very important that physicians and midwives work together as a team and they provide what the families need at any given point in time. And that means that not every family needs physician care. Many families need more than midwifery care. But we need to work together as a team. And that’s not always easy to effect, but I would work for as long as I can for that to happen.
DM: And what are the policy approaches to support that?
RL: I think that Congress has to be able to say “We want our families strengthened,” and this is one route that has been proven to some extent and we need to support it, for the future. We need funding that will support this model of care. And supporting it will save money in the long run. Because of what I mentioned in the past that if all Medicaid supported births were managed on the model that we have presented, it would save billions a year. I think that nowhere in the whole health care reform effort will there be the payoff that you would get from personalized, supportive, empowering, maternity services. Because it’s not just that birth, it’s what goes on through the whole life of the family. If you’re going to make change in this country, you have to start with childbearing families.
For a list of related websites, please refer to your Evolve Resources at http://evolve.elsevier.com/Mason/policypolitics/
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


