44 Care of the plastic and reconstructive surgical patient
Abdominoplasty: Surgical removal of abdominal fat and skin.
Augmentation Mammoplasty: Surgical procedure performed to enhance the size and shape of a breast.
Blepharoplasty: Procedure done to correct deformities of the upper or lower eyelid with excision of redundant skin or protruding fat.
Dermabrasion: Surgical planing of the skin with removal of the epidermis and portions of the superficial dermis for elimination of high spots or other irregularities in an uneven skin surface.
Deep Inferior Epigastric Artery Perforator (DIEP) Flap: Autologous breast reconstruction performed using an abdominal wall flap. Less abdominal wall damage is incurred using this technique.
Gynecomastia: Benign hypertrophy of breast tissue in males.
Inosculation: Vessel anastomosis from host to graft that allows for graft revascularization.
Latissimus Dorsi Flap: Reconstructive procedure involving donor site muscle, adipose tissue, and skin blood supply that is left connected and then tunneled to the mastectomy site.
Lipectomy: Surgical removal of fatty tissue.
Otoplasty: Surgical procedure done to reduce prominence of the ears.
Pedicle Flap: A preferred flap for wound tissue that is somewhat avascular, such as cartilage, bone, and tendon, or in the presence of avascular scar tissue and radiation-affected tissue. This type of flap is used to provide soft tissue closure while allowing blood vessels to remain intact.
Reduction Mammoplasty: Surgical removal of glandular tissue, fat, and skin from the breasts to achieve lighter, smaller, and firmer breast proportions.
Rhinoplasty: Reshaping or reconstruction of the nose when its shape has been altered as a result of trauma or when the patient is unhappy with its form.
Rhytidectomy: Surgical tightening of facial and neck muscles with removal of excess skin; commonly called a face lift procedure.
Tissue Expansion: Insertion and positioning of a temporary inflatable balloon or implant device under the skin, which is periodically increased in size through instillation of normal saline solution to promote expansion of the skin for reconstructive purposes.
Transverse Rectus Abdominis Myocutaneous (TRAM) Flap: This procedure is performed after a mastectomy and involves the reconstruction of a breast with autografting of lower abdominal muscle, skin, and adipose tissue. A pedicle TRAM flap uses the entire rectus abdominal muscle, whereas the free flap technique only partially involves this muscle.
Tumescent Liposuction: A dilute solution of lidocaine, used in combination with epinephrine, is injected into the adipose tissue layer to facilitate the vacuum removal of fat cells via a small cannula.
The field of plastic surgery encompasses cosmetic and reconstructive surgery, and related procedures and techniques have continuously evolved over time. This discipline is growing as consumer demand for cosmetic surgical procedures increases1 and the ability to achieve aesthetic reconstructive surgical outcomes improves.
Plastic surgery derives its name from the Greek word plastikos, which means to mold or give shape. The first successful tissue transfers are said to have originated in India more than 2500 years ago. Modern grafting techniques were explored in nineteenth-century Germany. Today, reconstructive procedures involve much more than the correction of acquired and congenital deformities. They are also performed to correct defects related to tumors, trauma, infection, burns and postburn contractures, pressure ulcers, or disease.2,3 Ideally, these procedures represent interconnected therapy4 that strives to restore normal function and enhance appearance to maintain or improve body image and self-esteem.5
Skin grafts
Skin grafting is the most common method for covering open areas that result from incomplete wound healing, trauma, burns, or large surgical incisions. Grafting involves the removal of a skin layer of varying thickness that is then transplanted to a host site. Transplanted skin layers can originate from the individual, be synthetic in origin, or be an expanded portion of the host’s own skin. The lower abdomen supplies a good source for the full-thickness skin graft.6
The major types of skin grafts are outlined in Box 44-1. Revascularization generally takes 3 to 5 days and requires growth of vessels from the host or the recipient tissue via a process called inosculation. For cosmetically pleasing results, the color, texture, thickness, and hair-bearing nature of the skin used for grafting should be chosen to match the recipient site. As a rule, the closer the donor skin is located to the recipient area, the better the match.
Box 44-1 Major Types of Skin Grafts
• A full-thickness graft includes all underlying dermis and epidermis and a small amount of subcutaneous tissue. These grafts, used to cover areas such as the nasal tip, dorsum, ala, and sidewall of the lower eyelid and ear, are more prone to necrosis.
• A split-thickness graft includes a portion of the underlying dermis and the entire epidermis. This graft is the least durable. It can be thin, medium, or thick, depending on the amount of dermis included.
• A composite graft comprises two or more tissue components and often includes skin and subcutaneous tissue, cartilage, or mucosa that can be used to reconstruct a patient’s ear, nose, or eyelid.
• A free cartilage graft involves a portion of cartilage that is harvested and reimplanted to provide structure and support to the site. One example is the use of rib cartilage to create an ear structure in a patient with microtia.
• An autograft indicates that the donor and the recipient are the same person.
• An isograft signifies that the donor and the recipient are genetically identical.
• Allograft or homograft means that the donor and the recipient are of the same species; this procedure may entail the use of cadaver tissue.
• A xenograft indicates that the donor and the recipient are of different species (e.g., porcine or bovine sources).
• Bioengineered skin and skin substitutes contain cells that may be animal, human, or host hybrids which acclimatize to the wound and accelerate healing. The mechanism of action is unknown.
Factors that influence graft survival include: adherence to the recipient tissue; adequate vascularity signs, which include color and capillary refill of site; close monitoring of graft tissue for early identification of complications; and strict management of oxygenation, hemodynamic stability, thermoregulation, pain control, and positioning. Postoperative monitoring and assessment for serum or blood in the graft site is important during the first 24 hours. Excess fluid can cause the graft to lift from its bed and must be removed. The donor site should be kept clean, and heals by forming a new layer of skin.7 Many variations exist in the type of wound dressing used, use of pressure dressings, required positioning of the patient, use of ice or antibiotic ointments, and handling of donor sites.
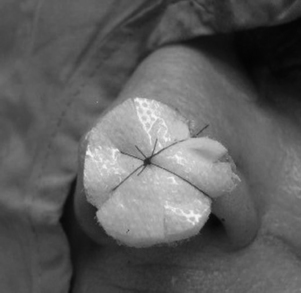
Every effort should be made to keep the patient calm and still and to prevent touching, removing or shifting of dressings. Some dressings, such as the bolster dressing shown in Fig. 44-1, may actually be sutured in place. Generally, the grafted area should be elevated and protected from both pressure and motion. The patient should be positioned to prevent any pressure on or other trauma to the graft or the donor site. The surgeon may order cold packs to reduce metabolic requirements of the graft and enhance its chances of survival. Dressings over grafts should be observed closely for drainage. The presence of excess drainage should be reported to the physician.
Flaps
Microvascular tissue transfer and free flaps
The most serious complication in a microvascular tissue transfer procedure is tissue necrosis. Tissue death occurs when the artery or the vein that supplies the flap develops a thrombus. Arterial thrombosis can result in complete flap failure within 4 hours of onset. Arterial occlusion is characterized by a pale cool flap that does not bleed when stuck with a needle. Hematomas can form at the recipient site and occur more commonly in the patient who preoperatively smokes or uses nonsteroidal antiinflammatory drugs or corticosteroids.8
Venous thrombosis is more commonly encountered, but it is not an immediate threat. Thrombosis is characterized by a congested warm mottled flap that continuously oozes dark blood. Objective assessment of the flap is possible with fluorometry, transcutaneous oxygen tension, thermometry, laser Doppler scan, temperature monitoring, buried Doppler probe, or photoplethysmograph disk for monitoring of blood flow. Any change in skin color from the normal baseline or monitoring findings that indicates imminent occlusion should be reported to the surgeon immediately. A donor site typically generates more painful stimuli than the transplanted skin graft or flap site.9 Pain management should be individualized and based on the patient’s self-reported pain levels. Nursing care should include administration of analgesics and selected nonopioid adjuvants with attention to comfort measures as needed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree