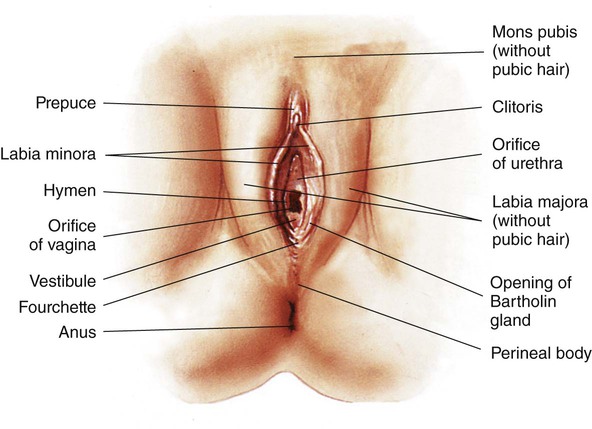
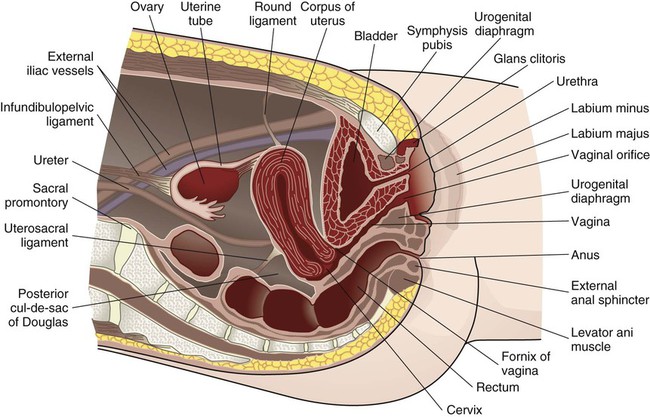
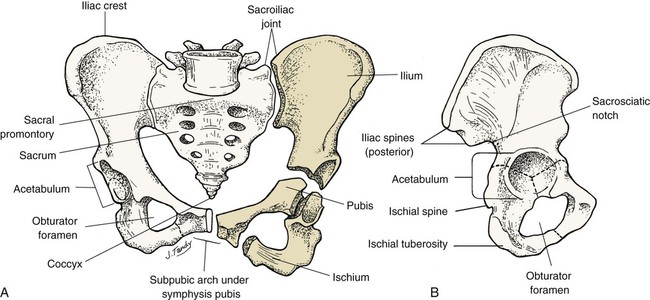
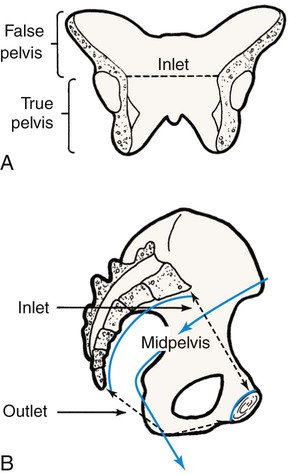
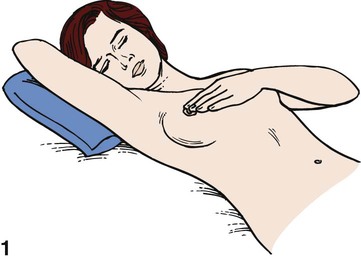
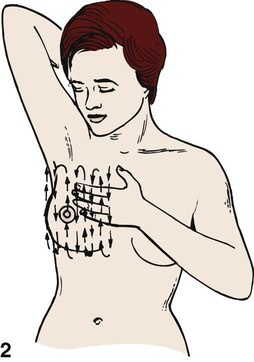
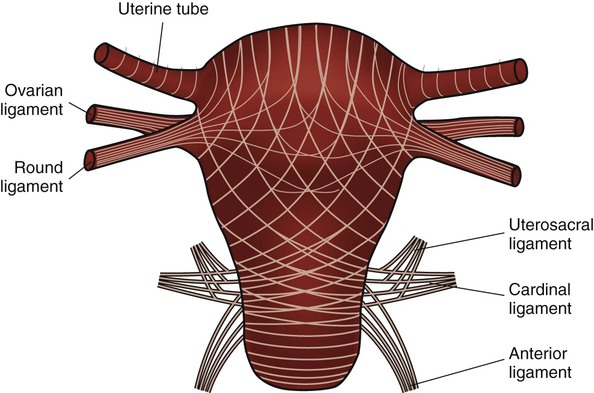
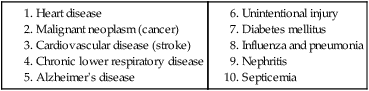Chapter 3 On completion of this chapter, the reader will be able to: • Identify the structures and functions of the female reproductive system. • Describe the menstrual cycle in relation to hormonal, ovarian, and endometrial responses. • Identify the phases of the sexual response cycle. • Identify facilitators and barriers for women to access care in the health care system. • Analyze financial, cultural, gender, and communication barriers that may affect a woman’s decision to seek and follow through with health-promoting activities. • Describe the need for health promotion across the woman’s life span. • Analyze conditions and factors that increase health risks for women across the life span, including life stage, substance abuse, eating disorders, medical/health conditions, pregnancy, and intimate partner violence. • Describe components of taking a woman’s history and performing a physical examination. • Review patient teaching of breast self-examination. • Describe how the history and physical examination can be adapted for women with special needs. • Outline the health-screening schedules for women across the life span. • Identify the correct procedure for assisting with and collecting Papanicolaou test specimens. The external genital organs, or vulva, include all structures visible externally from the pubis to the perineum. These include the mons pubis, labia majora, labia minora, clitoris, vestibular glands, vaginal vestibule, vaginal orifice, and urethral opening. The external genital organs are illustrated in Fig. 3-1. The uterus is divided into two major parts: an upper triangular portion called the corpus and a lower cylindric portion called the cervix (Fig. 3-2). The fundus is the dome-shaped top of the uterus and is the site at which the uterine tubes (fallopian tubes) enter the uterus. The isthmus, or lower uterine segment, is a short, constricted portion that separates the corpus from the cervix. The uterine wall is made up of three layers: the endometrium, the myometrium, and part of the peritoneum. The endometrium is a highly vascular lining made up of three layers, the outer two of which are shed during menstruation. The myometrium is made up of layers of smooth muscles that extend in three different directions (longitudinal, transverse, and oblique) (Fig. 3-3). Longitudinal fibers of the outer myometrial layer are found mostly in the fundus, and this arrangement assists in expelling the fetus during the birth process. The middle layer contains fibers from all three directions, which form a figure-eight pattern encircling large blood vessels. These fibers assist in ligating blood vessels after childbirth and control blood loss. Most of the circular fibers of the inner myometrial layer are around the site where the uterine tubes enter the uterus and around the internal cervical os (opening). These fibers help keep the cervix closed during pregnancy and prevent menstrual blood from flowing back into the uterine tubes during menstruation. The bony pelvis serves three primary purposes: protection of the pelvic structures, accommodation of the growing fetus during pregnancy, and anchorage of the pelvic support structures. The two innominate (hip) bones (consisting of ilium, ischium, and pubis), the sacrum, and the coccyx make up the four bones of the pelvis (Fig. 3-4). Cartilage and ligaments form the symphysis pubis, sacrococcygeal joint, and two sacroiliac joints that separate the pelvic bones. The pelvis is divided into two parts: the false pelvis and the true pelvis (Fig. 3-5). The false pelvis is the upper portion above the pelvic brim or inlet. The true pelvis is the lower, curved, bony canal, which includes the inlet, the cavity, and the outlet through which the fetus passes during vaginal birth. The upper portion of the outlet is at the level of the ischial spines, and the lower portion is at the level of the ischial tuberosities and the pubic arch. Variations that occur in the size and shape of the pelvis are usually related to age, race, and sex. Pelvic ossification is complete at about 20 years of age. The breasts are paired mammary glands located between the second and sixth ribs (Fig. 3-6). About two thirds of the breast overlies the pectoralis muscle, between the sternum and midaxillary line, with an extension to the tail of Spence. The lower one third of the breast overlies the serratus anterior muscle. The breasts are attached to the muscles by connective tissue or fascia. Findings from several studies using ultrasound imaging to investigate the anatomy of the breast reported differences from previous descriptions (Geddes, 2007; Love and Barsky, 2004; Ramsay, Kent, Hartmann, et al., 2005). The following description incorporates these findings. Each mammary gland is made of a number of lobes that are divided into lobules. Lobules are clusters of acini. An acinus is a saclike terminal part of a compound gland emptying through a narrow lumen or duct. The acini are lined with epithelial cells that secrete colostrum and milk. Just below the epithelium is the myoepithelium (myo, or muscle), which contracts to expel milk from the acini. The ducts from the clusters of acini that form the lobules merge to form larger ducts draining the lobes. Ducts from the lobes converge in a single nipple (mammary papilla) surrounded by an areola. The anatomy of the ducts is similar for each breast but varies among women. Protective fatty tissue surrounds the glandular structures and ducts. Cooper’s ligaments, or fibrous suspensory, separate and support the glandular structures and ducts. Cooper’s ligaments provide support to the mammary glands while permitting their mobility on the chest wall (see Fig. 3-6). The round nipple is usually slightly elevated above the breast. On each breast the nipple projects slightly upward and laterally. It contains 4 to 20 openings from the milk ducts. The nipple is surrounded by fibromuscular tissue and covered by wrinkled skin (the areola). Except during pregnancy and lactation, there is usually no discharge from the nipple. The breasts change in size and nodularity in response to cyclic ovarian changes throughout reproductive life. Increasing levels of both estrogen and progesterone in the 3 to 4 days before menstruation increase the vascularity of the breasts, induce growth of the ducts and acini, and promote water retention. The epithelial cells lining the ducts proliferate in number, the ducts dilate, and the lobules distend. The acini become enlarged and secretory, and lipid (fat) is deposited within their epithelial cell lining. As a result, breast swelling, tenderness, and discomfort are common symptoms just before the onset of menstruation. After menstruation, cellular proliferation begins to regress, acini begin to decrease in size, and retained water is lost. After breasts have undergone changes numerous times in response to the ovarian cycle, the proliferation and involution (regression) are not uniform throughout the breast. In time, after repeated hormonal stimulation, small, persistent areas of nodulations may develop. This normal physiologic change must be remembered when breast tissue is examined. Nodules may develop just before and during menstruation, when the breast is most active. The physiologic alternations in breast size and activity reach their minimum level about 5 to 7 days after menstruation stops. Therefore breast self-examination (BSE) (systematic palpation of breasts to detect signs of breast cancer or other changes) is best carried out during this phase of the menstrual cycle (see Guidelines box). Although monthly BSE used to be recommended to all women, the current guidelines recommend BSE as an option (American Cancer Society, 2012b), mostly because they believe that many unnecessary biopsies and other procedures result. However, breastcancer.org (2012) continues to recommend that all women perform BSE monthly (see the Critical Thinking Case Study). Menstruation is the periodic uterine bleeding that begins approximately 14 days after ovulation. It is controlled by a feedback system of three cycles: endometrial, hypothalamic-pituitary, and ovarian. The average length of a menstrual cycle is 28 days, but variations are normal. The first day of bleeding is designated as day 1 of the menstrual cycle, or menses (Fig. 3-7). The average duration of menstrual flow is 5 days (with a range of 3 to 6 days) and the average blood loss is 50 mL (with a range of 20 to 80 mL), but these vary greatly. The four phases of the endometrial cycle are (1) the menstrual phase, (2) the proliferative phase, (3) the secretory phase, and (4) the ischemic phase (see Fig. 3-7). During the menstrual phase, shedding of the functional two thirds of the endometrium (the compact and spongy layers) is initiated by periodic vasoconstriction in the upper layers of the endometrium. The basal layer is always retained, and regeneration begins near the end of the cycle from cells derived from the remaining glandular remnants or stromal cells in this layer. Implantation of the fertilized ovum generally occurs about 7 to 10 days after ovulation. If fertilization and implantation do not occur, the corpus luteum, which secretes estrogen and progesterone, regresses. With the rapid decrease in progesterone and estrogen levels, the spiral arteries go into spasm. During the ischemic phase, the blood supply to the functional endometrium is blocked and necrosis develops. The functional layer separates from the basal layer, and menstrual bleeding begins, marking day 1 of the next cycle (see Fig. 3-7). Toward the end of the normal menstrual cycle, blood levels of estrogen and progesterone decrease. Low blood levels of these ovarian hormones stimulate the hypothalamus to secrete gonadotropin-releasing hormone (GnRH). In turn, GnRH stimulates anterior pituitary secretion of follicle-stimulating hormone (FSH). FSH stimulates development of ovarian graafian follicles and their production of estrogen. Estrogen levels begin to decrease, and hypothalamic GnRH triggers the anterior pituitary to release luteinizing hormone (LH). A marked surge of LH and a smaller peak of estrogen (day 12) (see Fig. 3-7) precede the expulsion of the ovum from the graafian follicle by about 24 to 36 hours. LH peaks at about day 13 or 14 of a 28-day cycle. If fertilization and implantation of the ovum have not occurred by this time, regression of the corpus luteum follows. Levels of progesterone and estrogen decline, menstruation occurs, and the hypothalamus is once again stimulated to secrete GnRH. This process is called the hypothalamic-pituitary cycle. The primitive graafian follicles contain immature oocytes (primordial ova). Before ovulation, from 1 to 30 follicles begin to mature in each ovary under the influence of FSH and estrogen. The pre-ovulatory surge of LH affects a selected follicle. The oocyte matures, ovulation occurs, and the empty follicle begins its transformation into the corpus luteum. This follicular phase (pre-ovulatory phase) (see Fig. 3-7) of the ovarian cycle varies in length from woman to woman. Almost all variations in ovarian cycle length are the result of variations in the length of the follicular phase. On rare occasions (i.e., 1 in 100 menstrual cycles), more than one follicle is selected and more than one oocyte matures and undergoes ovulation. PGs produced by the woman cause regression of the corpus luteum and regression and sloughing of the endometrium, resulting in menstruation. PGs increase myometrial response to oxytocic stimulation, enhance uterine contractions, and cause cervical dilation. They may be a factor in the initiation of labor, the maintenance of labor, or both. They may also be involved in dysmenorrhea (see Chapter 4) and preeclampsia/eclampsia (see Chapter 12). The sexual response cycle is classically divided into four phases: excitement, plateau, orgasmic, and resolution, according to the seminal work of Masters and Johnson (1966). The four phases occur progressively, with no sharp dividing line between any two phases. The time, intensity, and duration for cyclic completion also vary for individuals and situations. Other researchers have suggested different models to explain sexual response. Leeman and Rogers (2012) emphasize the need to address sexuality and possible sexual difficulties with women in the postpartum period. Specific issues related to this period (and prior procedures such as episiotomy) must be considered in counseling to promote healthy sexuality during the postpartum period. Despite these alternate models of sexual response, it is still common to describe the classic four stages in which specific body changes take place in sequence, and this description is useful in educating and talking with women who may have concerns about possible sexual dysfunction. Table 3-1 compares male and female body changes during each of the four phases of the sexual response cycle. TABLE 3-1 FOUR PHASES OF SEXUAL RESPONSE In the United States, disparity among races and socioeconomic classes affects many facets of life including health. Limited finances is associated with lack of access to care, delay in seeking care, few prevention activities, and little accurate information about health and the health care system. Women use health care services more often than men but are more likely than men to have difficulty in financing the services. Many poor women have traditionally been underinsured or uninsured, but rules about health insurance and who and what are covered are undergoing a transition with the Affordable Care Act (healthcare.gov, 2012). People will not be denied insurance because of pre-existing conditions, and various preventive health services will be covered under health insurance. However this legislation is far from decided and its impact on the American people will not be known for years. With a greater focus on preventive health care services and with 32 million formerly uninsured patients having access to health care, nurses, advanced practice nurses, including nurse practitioners, midwives, and clinical nurse specialists, are critical to the provision of high quality, safe, effective, and accessible health care (see the Community Focus box). We live in a multicultural society with constantly changing demographics, and for nursing care of women to be optimal, cultural differences must be addressed with great sensitivity and competency. Nurses are in excellent positions to be responsible for providing culturally sensitive and competent health care (Escallier, Fullterton, and Messina, 2011). A variety of reasons are given to explain some of the differences in accessing care when financial barriers are adjusted. Some women experience racial discrimination or disrespectful, disillusioning, or discouraging encounters with community service providers such as social services and health care providers. Many women do not seek care from the health care system because of lack of trust (Yang, Matthews, and Hillemeier, 2011). A lack of cross-cultural communication also presents problems. Desired health outcomes are best achieved when the health care provider has knowledge of and understanding about the culture, language, values, priorities, and health beliefs of those in various ethnic groups. Conversely, members of these various groups should understand the health goals to be achieved and the methods proposed to do so. Language differences can produce profound barriers between patients and providers. Even with an interpreter, misinformation can occur on both sides of the communication. Providers must consider culturally based differences that could affect the treatment of diverse groups of women, and the women themselves must share practices and beliefs that could influence their responses to treatment or willingness to adhere to treatment. For example, women in some cultures value privacy to such an extent that they are reluctant to disrobe and, as a result, avoid physical examination unless absolutely necessary. Other women rely on their husbands to make major decisions, including those affecting the woman’s health. Religious beliefs may dictate a plan of care, as with birth control measures or blood transfusions. Some cultural groups prefer folk medicine, homeopathy, or prayer to traditional Western medicine; and others attempt combinations of some or all practices. Nurses can integrate into their own practice various holistic approaches to care, in accordance with Dossey’s (2010) Theory of Integral Nursing. It is critically important to be sensitive to cultural differences and at the same time not stereotype and assume that a woman has certain beliefs because of her ethnic background. Although the amount of health information on the Internet is increasing, information in languages other than English is limited and not all information on the Internet is accurate, making health literacy an important issue in culturally competent care. Gender influences provider-patient communication and may influence access to health care in general. Researchers have reported significant male-female differences in receipt of major diagnostic and therapeutic interventions, especially with cardiac and kidney problems. Women tend to use primary care services more often than do men and, some believe, more effectively. The gender of the provider plays a role. The concept of “gender concordance,” in which the patient’s gender matches the health care provider’s gender, was found to be important for women seeking Pap tests (McAlearney, Oliveri, Post, et al., 2011). McAlearney et al. found that women were more comfortable having a Pap test performed by a female physician and having a female nurse present. Sexual orientation may produce another barrier. Nurses need to understand the specific health care needs and issues related to sexual orientation (Brennan, Barnsteiner, de Leon Siantz, et al., 2012). Some lesbians may not disclose their sexual orientation to health care providers because they feel they may be at risk for hostility, inadequate health care, or breach of confidentiality. In many health care settings, heterosexuality is assumed, and the setting may be one in which the woman does not feel welcome (magazines, brochures, and environment reflect heterosexual couples, or the health care provider shows discomfort interacting with the woman). Lesbians themselves may hold beliefs that are incorrect (e.g., that they have immunity to human immunodeficiency virus [HIV], sexually transmitted infections [STIs], and certain cancers [e.g., cervical]). The perceived lack of risk can result in lesbians avoiding health care, as well as in health care providers giving incorrect advice or not providing appropriate screening for these women. Not all gynecologic cancers are related to sexual activity; lesbians who have never had children may be more at risk for breast, ovarian, and endometrial cancer. Their risk for heart disease, cancer of the lung, and colon cancer is not different from that of the heterosexual woman. To offset stereotypes, it is necessary for providers to develop an approach that does not assume that all patients are heterosexual. More content related to this issue needs to be included in nursing curricula. Maintaining optimal health is a goal for all women. Essential components of health maintenance are the identification of unrecognized problems and potential risks and the education and health promotion needed to reduce them. Current trends in the health care of women have expanded beyond a reproductive focus. A holistic approach to women’s health care goes beyond simple reproductive needs and includes a woman’s health needs throughout her lifetime, with attention to physical, mental/emotional, social, and spiritual health. Women’s health is considered to be part of the primary health care delivery system with assessment and screening focusing on a multisystem evaluation that emphasizes the maintenance and enhancement of wellness. Prevention of cardiovascular disease, promotion of mental health, and prevention of cancers beyond just reproductive-related cancers are all components of well-woman care. It is important to consider all aspects of women’s health, particularly in light of the fact that the leading causes of death in women in the United States include more than just reproductive health conditions (Box 3-1). All teens undergo progressive development of sex characteristics. They experience the developmental tasks of adolescence such as establishing identity and sexual orientation, emancipating from family, and establishing career goals. Some of these processes can produce great stress for the adolescent, and the health care provider should treat her very carefully. Female teenagers who enter the health care system usually do so for screening or because of a problem such as episodic illness or accidents. Previous guidelines recommended that young women should be screened with Pap tests at age 18 or when they become sexually active. Guidelines suggest that Pap tests begin at age 21, but controversy exists about the evidence to support these new guidelines, with some health care providers providing evidence for earlier testing (Zhao, Kalpos-Novak, and Austin, 2011). Gynecologic problems are often associated with menses (either bleeding irregularities or dysmenorrhea), vaginitis or leukorrhea, STIs, contraception, or pregnancy. The adolescent is also at risk for use of street drugs, for eating disorders, and for stress, depression, and anxiety. Many women first enter the health care delivery system for a Pap test or for contraception. Visits to the nurse may be their only contact with the system unless they become ill. Some women postpone examination until a specific need arises such as pregnancy, infertility, pain, abnormal bleeding, or vaginal discharge. Recently the availability of the human papillomavirus (HPV) vaccine has created another reason for young women to enter the health care system (Saraiya, Rosser, and Cooper, 2012). Most young women begin having sex in the mid- to late teens. At age 15, 13% of teens have had sex, but by age 19, 70% of teens have had sexual intercourse (Guttmacher Institute, 2012). A sexually active teen who does not use contraception has a 90% chance of pregnancy within 1 year. The United States has the highest teen pregnancy rate in the industrialized world. By age 20, one third of all American girls get pregnant; most of these pregnancies are unintended (CDC, 2012). Effective educational programs about sex and family life are imperative to control the rate of teen pregnancy and STIs (Box 3-2). The nurse can provide information regarding the need for child spacing, methods of family planning that are consistent with religious and personal preferences, non-contraceptive benefits of certain methods, the appropriate use of methods selected, and the protection of future fertility when so desired. The woman older than 35 years does not have a different physical response to a pregnancy per se but, rather, has had health status changes as a result of time and the aging process. These changes may be responsible for age-related pregnancy conditions. For example, a woman with type 2 diabetes may not have had expression of her diabetes at age 22 years but may have full-blown disease at age 38 years. Other chronic or debilitating diseases or conditions increase in severity with time, and these in turn may predispose to increased risks during pregnancy. Of significance to women in this age-group is the risk for certain genetic anomalies (e.g., Down syndrome). The opportunity for genetic counseling should be available to all (see Chapter 6). Preconception health promotion provides women and their partners with information that is needed to make decisions about their reproductive future. Preconception care guides couples on how to avoid unintended pregnancies, identify and manage risk factors in their lives and their environment, and identify healthy behaviors that promote the well-being of the woman and her potential fetus. It has been estimated that 31% of pregnant women experience some complications of pregnancy, including mental health issues (mostly depression) and factors that lead to the need for cesarean birth (HealthyPeople.gov, 2012b). In addition, 12% of births result in preterm infants and 8.2% result in low-birth-weight infants (HealthyPeople.gov, 2012a). The components of preconception care such as health promotion, risk assessment, and interventions are outlined in Box 3-3. A woman’s entry into health care is often associated with pregnancy, for either diagnosis or actual prenatal care. Early entry into prenatal care (i.e., within the first 12 weeks) allows for identification of the woman at risk for complications and initiation of measures to prevent problems or treat them if they arise. The U.S. Department of Health and Human Services (2012) has emphasized the importance of early and consistent prenatal care to improve outcomes for both mother and infant. Major goals of prenatal care are listed in Box 3-4 and should be addressed in the first visit. Extensive discussion of pregnancy is found in Unit 3. More than half of the pregnancies in the United States each year are unintended (Taylor, Levi, and Simmonds, 2010), and the majority of these occur in women who either do not use contraception or who experienced a contraceptive failure. Education is the key to encouraging women to make family planning choices based on preference and actual benefit-to-risk ratios. Providers can influence the user’s motivation and ability to use the method correctly (see Chapter 5). Steps toward prevention of infertility should be undertaken as part of ongoing routine health care, and information about how women may prevent some causes of infertility is especially appropriate in preconception counseling. Primary care providers can undertake initial evaluation and counseling before couples are referred to specialists. For additional information about infertility, see Chapter 5.
Assessment and Health Promotion
Female Reproductive System
External Structures
Internal Structures
The Bony Pelvis
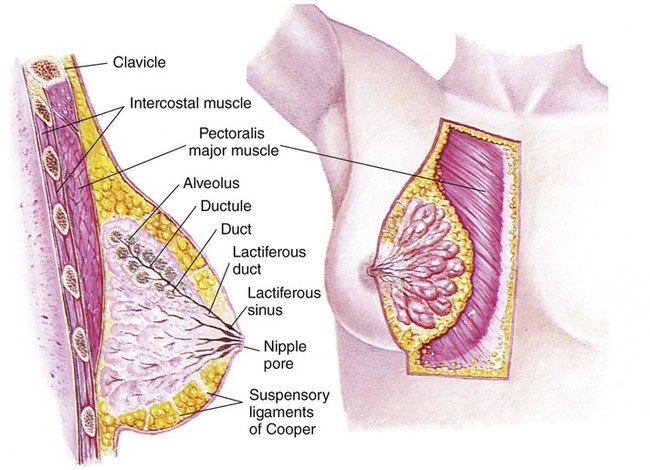
Breasts
Menstruation
Menarche and Puberty
Menstrual Cycle
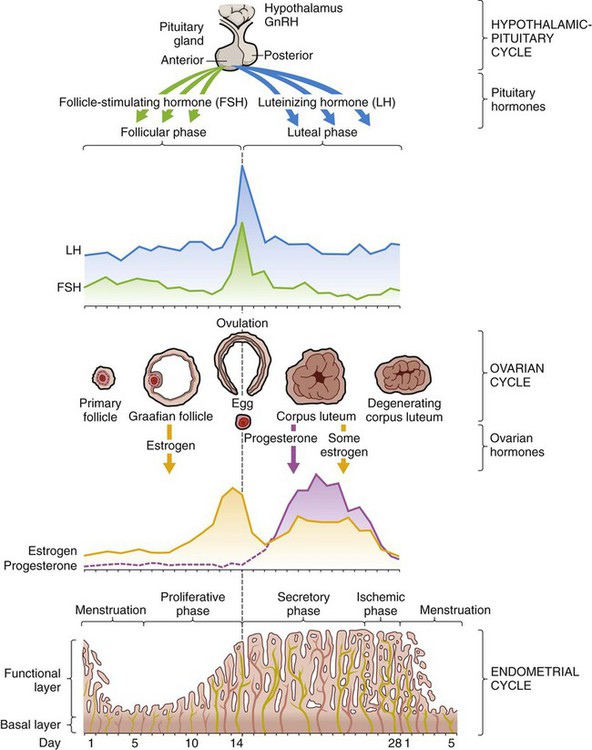
Endometrial Cycle
Hypothalamic-Pituitary Cycle
Ovarian Cycle
Prostaglandins
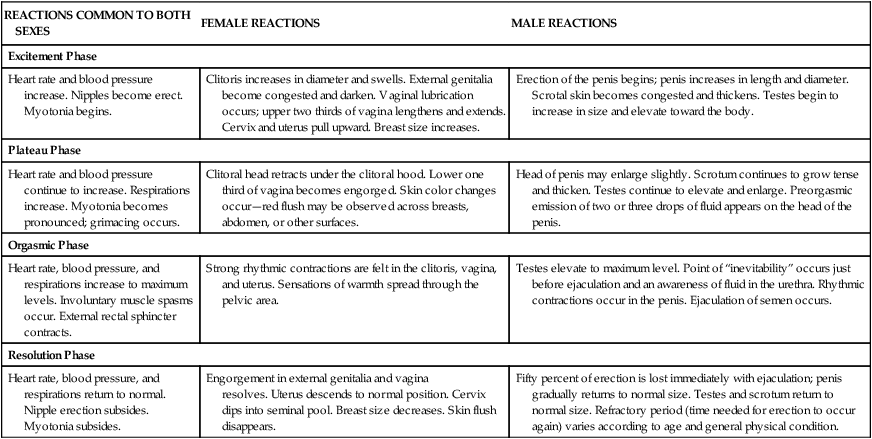
Sexual Response
REACTIONS COMMON TO BOTH SEXES
FEMALE REACTIONS
MALE REACTIONS
Excitement Phase
Heart rate and blood pressure increase. Nipples become erect. Myotonia begins.
Clitoris increases in diameter and swells. External genitalia become congested and darken. Vaginal lubrication occurs; upper two thirds of vagina lengthens and extends. Cervix and uterus pull upward. Breast size increases.
Erection of the penis begins; penis increases in length and diameter. Scrotal skin becomes congested and thickens. Testes begin to increase in size and elevate toward the body.
Plateau Phase
Heart rate and blood pressure continue to increase. Respirations increase. Myotonia becomes pronounced; grimacing occurs.
Clitoral head retracts under the clitoral hood. Lower one third of vagina becomes engorged. Skin color changes occur—red flush may be observed across breasts, abdomen, or other surfaces.
Head of penis may enlarge slightly. Scrotum continues to grow tense and thicken. Testes continue to elevate and enlarge. Preorgasmic emission of two or three drops of fluid appears on the head of the penis.
Orgasmic Phase
Heart rate, blood pressure, and respirations increase to maximum levels. Involuntary muscle spasms occur. External rectal sphincter contracts.
Strong rhythmic contractions are felt in the clitoris, vagina, and uterus. Sensations of warmth spread through the pelvic area.
Testes elevate to maximum level. Point of “inevitability” occurs just before ejaculation and an awareness of fluid in the urethra. Rhythmic contractions occur in the penis. Ejaculation of semen occurs.
Resolution Phase
Heart rate, blood pressure, and respirations return to normal. Nipple erection subsides. Myotonia subsides.
Engorgement in external genitalia and vagina resolves. Uterus descends to normal position. Cervix dips into seminal pool. Breast size decreases. Skin flush disappears.
Fifty percent of erection is lost immediately with ejaculation; penis gradually returns to normal size. Testes and scrotum return to normal size. Refractory period (time needed for erection to occur again) varies according to age and general physical condition.
Barriers to Entering the Health Care System
Financial Issues
Cultural Issues
Gender Issues
Caring for the Well Woman Across the Life Span: The Need for Health Promotion and Disease Prevention
Adolescents
Teenage Pregnancy
Young and Middle Adulthood
Parenthood After Age 35
Approaches to Care at Specific Stages of a Woman’s Life
Preconception Counseling and Care
Pregnancy
Fertility Control and Infertility
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Nurse Key
Fastest Nurse Insight Engine
Get Clinical Tree app for offline access