Chapter 10 Stabilization for Trauma and Dissociation
Trauma is an inescapable part of the human experience, and affects all dimensions of the person. Trauma dysregulates and disconnects the person physiologically, emotionally, spiritually, cognitively, interpersonally, and socially. Trauma refers to an extremely stressful event or situation that is experienced as overwhelming to the individual (Allen, 2005), and as a result, the experience/memory is stored dysfunctionally in the brain (Shapiro, 2001). Shapiro (2001) broadened the concept of trauma to include any negative event that has a lasting effect on the self. These negative events may be “small t” traumas or “big T” traumas. The latter coincides more closely with the current Diagnostic and Statistical Manual of Mental Disorders, fourth edition, text revision (DSM-IV-TR) criteria for posttraumatic stress disorder (PTSD) (Shapiro, 2001), such as natural disasters or rape. Chapter 1 provides a more comprehensive list of possible traumatic events.
This chapter further explicates the care of individuals who have suffered significant trauma and elaborates psychotherapeutic strategies for care using the Treatment Hierarchy Framework presented in Chapters 1 and 2, which also review the Adaptive Information Processing (AIP) model. In this chapter, the spectrum of traumatic responses is discussed. Diagnoses that reflect trauma include acute posttraumatic stress disorder (ASD), PTSD, borderline personality disorder (BPD), dissociative disorders (DDs), disorders of extreme stress not otherwise specified (DESNOS), somatoform disorders, and psychosomatic disorders. Goals of treatment and evidence-based research are highlighted. Interventions are aimed toward safety, developing dual awareness through mindfulness, and managing physiologic arousal. Resources for stage 1 (stabilization) are presented along with components of evidence-based psychotherapies, such as cognitive-behavioral therapy (CBT) and eye movement desensitization and reprocessing (EMDR), for stage 1. Clinical vignettes illustrate how to work with these patients.
Spectrum of Traumatic Response
Psychological trauma is thought to underlie or contribute to a wide range of psychiatric disorders and medical problems (Briere & Scott, 2006; Felitti et al., 1998; Hennessey et al., 2004; Morrison et al., 2003; Stien & Kendall, 2006). Most people who have significant trauma histories do not develop PTSD (see Chapter 1). However, the effects of major and minor traumas are cumulative and can significantly compromise functioning and lead to mental health problems, psychiatric disorders, and physical disorders (Scaer, 2005; Shapiro, 2001). An individual’s response and the long-term sequelae of trauma are highly individualistic and depend on the nature of the traumatic events, their frequency, the person’s age, the person’s development stage, genetic vulnerability, prenatal factors, gender, past experiences, preexisting neural physiology, cognitive deficits, emotional maturity, coping skills, hardiness, relationships with others, sociocultural factors, and a host of other factors (Antai-Otong, 2002; Scaer, 2005; Briere & Scott, 2006; Steinberg & Schnall, 2000).
The spectrum of the traumatic stress response is highlighted in Figure 10-1. Traumatic stress disorders include several diagnoses that result from one or more traumatic events and often include symptoms of intrusive thoughts, avoidant behavior, and hyperarousal. These symptoms can be thought of as state-dependent memories that result from earlier experiences with a traumatic situation. These memories are stored differently from normal memories; are not integrated with other, more adaptive networks; and may be encoded in sensations and images rather than in verbal narrative and context. What cannot be taken in cannot be linked to other experience.
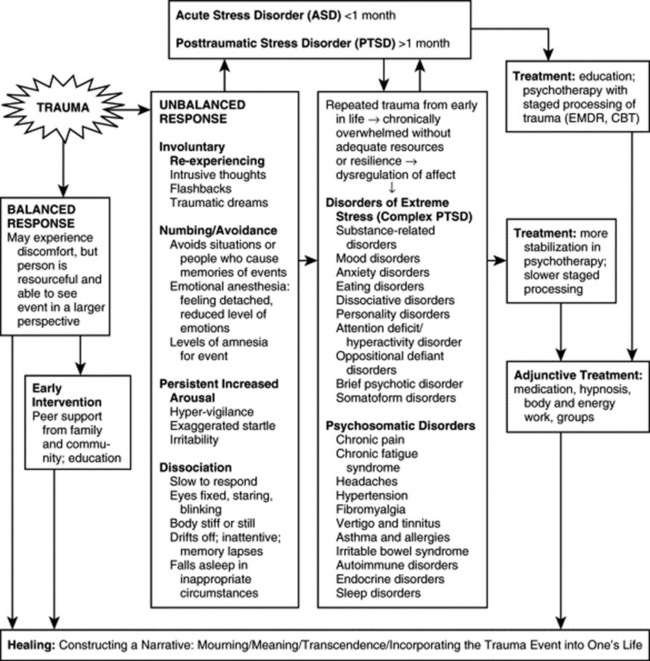
Figure 10-1 Spectrum of traumatic stress response.
(Adapted from Davis, K. & Weiss, L. [2004]. Traumatology: A workshop on traumatic stress disorders. Hamden, CT: EMDR Humanitarian Assistance Programs.)
This unprocessed trauma leads to unexpected re-experiencing or intrusive thoughts related to the trauma, the numbing of awareness or avoidance of situations or circumstances that are associated with the trauma, and a persistent increase in physiologic arousal. The patient may alternate between denial or numbing and experiencing intrusive thoughts or images (Horowitz, 2003). Table 10-1 lists common numbing and intrusive symptoms. During denial states, increased activity such as work, sports, or sexual activities may take place, and to quell the intrusive states, substances such as alcohol may be used. Intrusive emotional states reenact the stressor, and through overgeneralization, situations that before the trauma were neutral are infused with anger, fear, and sadness (Horowitz, 2003). Chapter 2 explained the neurophysiology of these cycles. Although these symptoms might have been adaptive at the time of the trauma, their contribution to the present can create significant problems for the person in identity and interpersonal relationships, affect dysregulation, and create cognitive distortions.
Table 10-1 Intrusive and Numbing Symptoms
| Feature | Intrusive Symptoms | Numbing Symptoms |
|---|---|---|
| Perception and attention | Hypervigilance; increased startle reactions; sleep and dream disturbances | Daze; selective inattention; inability to appreciate significance of stimuli |
| Consciousness of ideas and feelings related to the event | Repetitive thoughts, emotions and behaviors (e.g., images, nightmares, ruminations) | Amnesia; avoidance of thinking about event |
| Information processing | Confused, pressured, or disorganized when thinking about the event; overgeneralization of stimuli so it seems related to the event; preoccupation with event and inability to concentrate on anything else | Loss of realistic sense of appropriate connection with the world; constriction of thought; inflexibility of purpose; use of fantasy to counteract reality |
| Emotional attributes | Emotional attacks related to the event or to reminders | Emotional numbness; frantic overactivity; withdrawal; cannot decide how to respond to consequences of event |
| Somatic attributes | Hyperarousal with bowel pain, diarrhea or constipation; fatigue, headache, muscle pain, cramps, tremors; palpitations, increased pulse or hypertension; restlessness | Excessive sleeping; lethargy; hibernating |
Adapted from Horowitz, M. J. (2003). Treatment of stress response syndromes. Washington, DC: American Psychiatric Publishing.
In addition to the triad of hyperarousal, avoidance, and intrusive thoughts, one of the most disturbing symptoms for the patient is dissociation. Many clinicians view dissociation as on a continuum, with some dissociation considered a normal experience for most people. For example, we dissociate when we go to the movies, get “lost” in a good book, daydream, “space out” during a lecture, or drive from point A to point B without paying attention to how we got there. One study of the general population found 25% of people report mild to severe episodes of dissociation (Steinberg & Schnall, 2000). People can experience dissociation from mild daydreaming and spacing out to depersonalization and derealization episodes to total unresponsiveness, although they are awake and responsive to their environment (Allen, 2005). Severe episodes of dissociation occur in DDs when they interfere with social or occupational functioning. Dissociative identity disorder (DID), formerly called multiple personality disorder, is an extreme version of dissociation.
Significant dysfunctional states are characterized by a disconnection of thoughts, emotions, sensations, and behaviors. Dissociation indicates that neural networks are functioning independently and separately, that the networks are unintegrated, and that information processing has been disrupted. Dissociative states reflect discrete memory networks that have not been linked to other dimensions of consciousness. Dissociation is thought to be primarily a right brain phenomenon (Schore, 1994, 1997, 2006). Those who suffer from severe dissociation are those who have suffered significant trauma. Putnam (1989) provides an excellent definition of dissociation from his seminal book on multiple personality disorders: “a normal process that is initially used defensively by an individual to handle traumatic experiences [that] evolves over time into a maladaptive or pathological process” (p. 9). Box 10-1 describes patient-reported signs of dissociation, and Box 10-2 lists the observable signs of dissociation that the clinician may notice.
Box 10-1 Patient-Reported Signs of Dissociation
 Things look different, tunnel vision, colors too vivid or washed out
Things look different, tunnel vision, colors too vivid or washed out
 Things sound different, muffled or too loud, “tinny” or echoing
Things sound different, muffled or too loud, “tinny” or echoing
 Things seem to move in slow motion or fast forward
Things seem to move in slow motion or fast forward
 Emotions become flat, numb; no feelings
Emotions become flat, numb; no feelings
 Feeling out of touch with surroundings
Feeling out of touch with surroundings
 Feeling like an observer of current circumstances
Feeling like an observer of current circumstances
 People or the world does not seem real; feeling like a stranger in a familiar place
People or the world does not seem real; feeling like a stranger in a familiar place
 Feeling of watching things from outside the body
Feeling of watching things from outside the body
Box 10-2 Observable Signs of Dissociation
 Behavior that is an inappropriate response to stimuli, such as falling down after a loud noise; disorientation
Behavior that is an inappropriate response to stimuli, such as falling down after a loud noise; disorientation
 Eyes fixed, staring into space, blinking rapidly without focusing, or staring downward
Eyes fixed, staring into space, blinking rapidly without focusing, or staring downward
 Person drifts off, goes away, spaces out, blanks out, or loses track of what is happening
Person drifts off, goes away, spaces out, blanks out, or loses track of what is happening
 Person falls asleep in inappropriate circumstances
Person falls asleep in inappropriate circumstances
Adapted from Schiraldi, G. (2000). The posttraumatic stress disorder sourcebook, New York, McGraw-Hill; Scaer, R. (2005). The trauma spectrum: Hidden wounds and human resiliency. New York: W. W. Norton.
Dissociation is also considered a primitive type of defense in that as anxiety rises, the person may dissociate in an effort to avoid the perceived threat. Memories or information encoded in one state are not available to that person in another state. Neurophysiologically, the parasympathetic branch of the autonomic nervous system contributes to dissociation when the person experiences overwhelming stress. In this process, heart rate and blood pressure are reduced, and endogenous opioids are released (Stien & Kendall, 2006). This is a state of resignation or freeze in that the person cannot escape and the body responds by dissociating emotionally and mentally. This state may be associated with anhedonia, which is an inability to achieve or experience pleasure, and abulia, which is a state of profound apathy and inability to make decisions (Scaer, 2005).
This physiologic state gets “locked into” the brain with all the attending sensations that occurred at the time of the event. This state-dependent dissociation results in fragmented memories disconnected from words and instead stored as images, sounds, smells, and body sensations. Later similar experiences triggered by internal or external stimuli may activate this material (Shapiro, 2001, 2002). For example, internal stimuli such as the activation of a physiologic state such as anxiety or pain may serve as a trigger along with external stimuli such as a sound or smell. The dissociated patient may cycle rapidly between arousal with hypervigilance and then numbing confusion, and it may be difficult to distinguish whether the person is aroused or numb. The trauma victim “experiences repetitive episodes of sympathetic arousal that in turn reflexively trigger deep parasympathetic dissociation. The trauma victim lives in a state of involuntary and disruptive autonomic instability and cycling” (Scaer, 2005, p. 195).
Dissociative states may include flashbacks that are disturbing to the patient, and they may occur automatically when the intensity of feeling becomes too strong (Perry, 2002) or when triggers to the original trauma are encountered. Flashbacks reflect dissociated implicit capsules of memories (Howell, 2005). “The inability to integrate traumatic memories causes the person to fixate at the time of the trauma and impairs the integration of new memories” (Steinberg & Schnall, 2001, p. 42). Adults who experience trauma are not as likely to dissociate memories as children, because a child’s brain does not have the associated neural networks needed to process the overwhelming affects that occur in trauma, particularly with repeated sexual trauma. In general, “the younger the child when trauma occurs, the more likely it is that the event will be dissociated” (Steinberg & Schnall, 2000, p. 26). The more overwhelming the trauma, the more likely is the tendency to dissociate. Dissociation is pathologic when it becomes the primary response to stress (Stien & Kendall, 2006) or becomes problematic to the person.
Dissociation is thought to underlie most psychiatric disturbances, including substance abuse, eating disorders, depression, panic anxiety, generalized anxiety, phobias, obsessive-compulsive anxiety and personality disorders, conversion disorders, brief psychotic disorders, and other psychiatric disorders. Although these are considered trauma-related diagnoses (Briere & Scott, 2006; Howell, 2005), some trauma diagnoses are linked more specifically with dissociation and extreme trauma. The DSM-IV describes the specific criteria for each diagnosis (APA, 2000). The following diagnoses are those considered most closely linked with trauma and dissociation.
Acute Stress Disorder
ASD is a relatively new diagnosis in the DSM-IV. The essential features of ASD include anxiety and dissociation after direct exposure to a traumatic stressor or through witnessing or learning about a traumatic event that resolves within 4 weeks. There are fewer hyperarousal and avoidance symptoms than for PTSD and more dissociative symptoms such as psychic numbing, detachment, depersonalization, and derealization. Approximately 80% of those who meet the criteria for ASD will have PTSD within the next 6 months (Bryant & Harvey, 2000). If the symptoms persist after 4 weeks, the diagnosis may change to PTSD.
Posttraumatic Stress Disorder
The DSM-IV describes PTSD as the result of having been exposed firsthand or as a witness to an extreme situation or episode that causes “intense fear, helplessness, or horror” (APA, 2000, p. 463). Intrusive thoughts and recollections, avoidance behaviors, and states of hyperarousal must be present for at least 1 month after the traumatic event. If symptoms last less than 3 months, acute PTSD is diagnosed; if symptoms last longer than 3 months, chronic PTSD is diagnosed. Intrusive states include nightmares and flashbacks, which are fragments of distressing recollections, along with the physical components of the trauma (i.e., smell, physical sensation, taste, emotion, sound, and visual image). Avoidance behaviors include feelings of detachment, not thinking about the event, staying away from places that remind the person of the event, not remembering part or all of the event, diminished participation in pleasurable activities, not feeling (i.e., psychic numbing), and believing that as a result of the event, the person will not have a normal life. Hyperarousal may manifest by bursts of anger, agitation or irritability, difficulty concentrating, hypervigilance, difficulty falling or staying asleep, and an exaggerated startle response.
DSM-IV field trials have found that PTSD does not cover the extent of the problems experienced by those with this diagnosis, because somatization, dissociation, and affect dysregulation are all highly correlated (van der Kolk & Pelcovitz, 1999). Seventy-nine percent of patients with a diagnosis of PTSD have at least one other axis I diagnosis (Kessler et al., 1999). Epidemiologic studies have found that predisposing factors contributing to the diagnosis of PTSD include family and self-history of psychiatric illness, child abuse experiences, female gender, parental poverty, separation and divorce of parents before the child’s age of 10, job instability, and previous history of traumatic events (Horowitz, 2003; van der Kolk et al., 1996).
Borderline Personality Disorder
The diagnosis of BPD has developed a pejorative connotation among mental health providers. Many studies indicate that these individuals have suffered severe and extended childhood trauma, neglect, and loss (Herman, 1992; Herman et al., 1989). This disorder is characterized by a pattern of instability of interpersonal relationships, self-image, and affects and by marked impulsivity beginning in early adulthood. Often, severe dissociative symptoms are present with parasuicidal behaviors and chronic feelings of emptiness.
Dissociative Disorders
If the trauma is severe or prolonged or occurs early in life, PTSD and DDs are likely to develop. DDs are thought to be far more common than previously thought. A study of outpatients seeking psychotherapy found 29% of the 84 subjects tested had a diagnosis of DD after being interviewed with a structured interview for DDs (Foote et al., 2006). Only 5% of these subjects had been diagnosed with a DD before the interview. Steinberg and Schnall (2000) estimate that the 1-year prevalence rate for the general population is probably around 10%, which is the same as that for major depression and generalized anxiety disorder. DDs include DSM-IV diagnoses of dissociative amnesia, dissociative fugue, depersonalization disorder, DID, and DD NOS. Patients with DID almost universally suffer from comorbid PTSD (Chu et al., 2005).
Disorders of Extreme Stress
If the trauma is particularly prolonged or severe, pervasive personality problems develop. This is usually what we call complex PTSD or DESNOS (Herman, 1992). Herman (1992), in her ground-breaking book, coined the term complex posttraumatic syndrome to refer to survivors of childhood abuse who may accumulate a number of diagnoses, including bipolar disorder, depression, anxiety disorders, substance abuse disorders, eating disorders, BPD, somatization disorder, and DDs, in their encounters with the mental health system. Stien and Kendall (2006) add attention deficit hyperactivity disorder (ADHD) and oppositional defiant disorder (ODD) to this list as diagnoses related to complex trauma for children. Some are secondary diagnoses, such as substance abuse and eating disorders; they are categorized as secondary because the problems represent attempts by the traumatized person to cope with the effects of the trauma (Chu, 1998).
Brain and hormonal changes may occur as a result of early, prolonged trauma, and these changes contribute to long-term difficulties with memory, learning, and regulating impulses and emotions. In DSM-IV trial studies, seven clinical issues for DESNOS were identified as most relevant, and these are not included in the PTSD diagnosis (van der Kolk & Pelcovitz, 1999). Although not a DSM-IV diagnosis, DESNOS is thought to capture most people who have suffered significant and severe early trauma. These issues include difficulties with self-regulation and impulses, including self-destructive activities; problems in information processing, particularly with dissociation; personal identity issues such as self-blame, shame, and being permanently damaged; somatization of external stress manifesting in the body as disease or physical disorders; problems in interpersonal relationships and being dysfunctionally attached to perpetrators (Dworkin, 2005; van der Kolk & Pelcovitz, 1999). These individuals, referred to as the chronically disempowered by Chu (1998), are often survivors of childhood abuse and usually require long-term treatment extending over several years.
Somatoform Disorders
Somatic complaints have been identified as one of the most clinically relevant symptoms for trauma victims (van der Kolk & Pelcovitz, 1999). Those with significant somatic symptoms that are not caused by a medical condition are diagnosed under the general heading of somatoform disorder with one of the following diagnoses in the DSM-IV-TR: somatization disorder, conversion disorder, pain disorder, hypochondriasis, body dysmorphic disorder, undifferentiated somatoform disorder, and somatoform disorder not otherwise specified. These individuals have an excessive preoccupation with bodily dysfunction and manifest a variety of physical problems, such as neurologic (especially headaches) and gastrointestinal symptoms, chronic pain, and sexual dysfunction that cannot be explained based on their medical condition. Conversion reactions include paralysis, anesthesia, blindness, and deafness (Briere & Scott, 2006). Trauma, dissociation, and physical symptoms are inexorably linked, and there is a preoccupation with somatic problems. This may be especially true for many cultures that have somatization and dissociation syndromes. These are listed in the DSM-IV-TR Glossary of Culture-Bound Syndromes and include the following: Latin-American cultures with ataque de nervious and susto, Malaysia with latah, the Philippines with silok or mali-mali, Eskimo communities with pibloktoq, China with shenkur and dhat, Korea with shin-byung, and West Africa with brain fag (APA, 2000).
Psychosomatic Disorders
Psychosomatic disorders most likely overlap and are closely aligned with somatoform disorders but not specifically delineated in the DSM-IV-TR because they are considered medical illnesses. Psychosomatic disorders have significant physiologic changes in various tissues or organs in the body that are thought to be caused by childhood trauma or overwhelming stress. Psychosomatic disorders are induced by emotions and are mediated by the immune-peptide, autonomic-peptide, and neuroendocrine-peptide systems (Sarno, 2006). Sarno posits that these individuals are “repressors”; those who have a psychosomatic disorder subjectively do not experience painful and dangerous emotions and instead repress anger and anxiety. These emotions are thought to be too disturbing for the person if made conscious.
Psychosomatic medical illnesses include tension myositis syndrome, which often manifests as back and neck pain; carpal tunnel syndrome; chronic fatigue syndrome; rheumatoid arthritis; fibromyalgia; allergies; asthma; psoriasis; eczema; acne; irritable bowel syndrome; tension and migraine headaches; vertigo and tinnitus; endocrine and autoimmune disorders; sleep-disordered breathing; and paroxysmal and essential hypertension (Hoffman, 2006; Leonard-Segal, 2006; Mann, 2003, 2006; Rashbaum & Sarno, 2003; Rochelle, 2006; Scaer, 2005; Sarno, 2006).
Scaer (2005) posits that the parasympathetic freeze response combined with autonomic dysregulation and abnormal cycling underlie somatoform and psychosomatic disorders. He considers these to be the diseases and disorders of trauma. Although these diseases and disorders are associated with the presence of specific genes, he believes that they are primarily caused by early childhood and complex traumas that activate latent genetic tendencies (Scaer, 2005). Because individuals with these disorders most often seek medical attention and usually do not seek psychotherapy and medical researchers are not particularly interested in psychology, there is no solid evidence base for psychotherapy as a first-line treatment. However, there is anecdotal evidence for the efficacy of insight-oriented psychotherapy and EMDR for some of these trauma-related medical problems. Scaer categorizes these disorders and diseases based on the predominant feature of their abnormal function (Scaer, 2005), as shown in Table 10-2.
Table 10-2 Diseases and Disorders of Trauma
| Diseases and Disorders | Examples of Abnormal Function |
|---|---|
| Diseases of abnormal autonomic regulation | Fibromyalgia, irritable bowel syndrome, chronic fatigue syndrome, gastroesophageal reflux disease, mitral valve prolapse or dysautonomia syndrome, multiple chemical sensitivities, migraine headache |
| Syndromes of procedural memory | Whiplash syndrome, cumulative trauma disorder, tics, phantom limb pain, chronic pain, premenstrual dysphoric syndrome, postpartum depression or psychosis |
| Diseases of somatic dissociation | Reflex sympathetic dystrophy, interstitial cystitis, chronic pelvic pain |
| Disorders of endocrine and immune system regulation | Hyperthyroidism, diabetes, rheumatoid arthritis, systemic lupus erythematosus, Sjögren’s syndrome, Graves’ disease, Hashimoto’s thyroiditis, multiple sclerosis |
| Disorders of cognition and sleep | Attention deficit disorder, sleep disordered breathing, sleep apnea, narcolepsy, cataplexy, hypnogogic hallucinations, sleep paralysis |
Adapted from Scaer, R. (2005). The trauma spectrum: Hidden wounds and human resiliency. New York: W. W. Norton.
Goals of Treatment
Patients with significant trauma histories come to treatment with a range of disturbing symptoms and present significant diagnostic and treatment challenges. The complexity of symptoms and multiple diagnoses confuse and challenge clinicians who care for this population. In general, the goals of treatment for PTSD can be applied to those who suffer from other trauma-related diagnoses. These are delineated in the American Psychiatric Association’s practice guidelines for PTSD (2004) and include reducing the severity of symptoms, preventing or treating trauma-related comorbid conditions that are present, improving adaptive functioning, restoring a psychological sense of safety and trust, protecting against relapse, and integrating the danger experienced into a constructive schema of risk, safety, prevention, and protection.
Because trauma aborts normal development, and consequently, interpersonal, professional, and educational opportunities are lost, assisting the person in restoring and promoting progress in the affected areas is important. Maturational social coping skills may be impaired, particularly for those who suffered trauma in childhood. McFarlane and van der Kolk (1996) observe that trauma causes the person to abandon hope because the person is unable to look beyond him/herself to plan for the future. Clinical signs of recovery include being able to talk about the trauma without feeling upset or numb, functioning in daily life, feelings of being safe and confident, being in healthy relationships without feeling vulnerable, taking pleasure in life, having the ability to rely on self and others, experiencing minimal dissociation, managing emotions, feeling deserving, and being able to plan for the future.
Although these outcomes may seem daunting for patients who are chronically disempowered, they are achievable by following a progression of interventions that build on a strong foundation of safety and stabilization. Symptom outcome measures used for assessment can be used to track progress during treatment and to help determine whether the goals of treatment have been met. Tables 10-3 and 10-4 present dissociation and trauma assessment and outcome instruments. Screening tools include the Impact of Event Scale (IES) and the Dissociative Experience Scale (DES), both of which are included in Chapter 4. The Modified PTSD Symptom Scale (MPSS-SR) and the Trauma and Attachment and Belief Scale (TABS) are also self-report instruments but more elaborate than a brief screening tool. Clinician administered interviews include the Structured Interview for DSM-IV Dissociative Disorders–Revised (SCID-D), the Clinician-Administered PTSD Scale (CAPS), and the Structured Interview for Disorders of Extreme Stress (SIDES). The CAPS is the most widely used structured interview for PTSD, whereas the SIDES was developed to address the complex symptoms that develop as a result of trauma that are not captured by other tools for the diagnosis of PTSD, and it should be used whenever significant and severe trauma is reported. All the clinician-administered interviews require at least an hour to complete.
Table 10-3 Assessment and Outcome Instruments for Dissociation
| Instrument | Purpose and How to Obtain |
|---|---|
| Dissociative Experiences Scale (DES) (Bernstein & Putnam, 1986) | Most often used self-report screening tool for dissociation Included in Chapter 4 |
| Structured Interview for DSM-IV Dissociative Disorders–Revised (SCID-D) (Steinberg, 1994) | Most widely used structured interview for dissociative disorders; evaluates the presence, type, and severity of dissociative symptoms (Interviewers guide to the structured clinical interview for DSM-IV dissociative disorders. Washington, DC, American Psychiatric Publishing) |
Table 10-4 Assessment and Outcome Instruments for Trauma
| Instrument | Purpose and How to Obtain |
|---|---|
| Impact of Event Scale-revised (IES-R)(Weiss & Marmar, 1997) | Most widely used self-report screening tool for single-incident trauma, 22 items Included in Chapter 4 |
| Modified PTSD Symptom: Self-Report Version (MPSS-SR)(Falsetti et al., 1993) | Self-report 17-item symptom checklist of posttraumatic stress disorder (PTSD) symptoms; especially useful for patients with multiple traumas or when trauma history is unknown; is not keyed to a specific trauma Sherry Falsetti, PhD, Medical University of South Carolina, Crime Victims Research and Treatment Center, Medical University of North Carolina, 171 Ashley Avenue, Charleston, SC 29425-0742 |
| Trauma and Attachment Belief Scale (TABS)(Pearlman, 2003) | Self-report scale that evaluates the needs and expectation of trauma survivors in relation to others; taps into underlying assumptions regarding relationships Western Psychological Services, 12031 Wilshire Boulevard, Los Angeles, CA 90025-1251; telephone: 310-478-2061; fax: 310-478-7838; website: www.wpspublish.com |
| The Structured Interview for Disorders of Extreme Stress (SIDES) (Pelcovitz et al., 1997) | Clinician administered 45-item tool that measures the symptom clusters of disorders of extreme stress not otherwise specified (DESNOS) HRI Trauma Center Research Department, c/o Dr. J. Hopper, 227 Babcock Street, Brookline, MA 02116; website: bvanderk@traumacenter.org |
| The Clinician Administered PTSD Scale (CAPS) (Blake et al., 1995) | The most widely used clinician-administered structured interview for PTSD; assesses frequency and intensity of symptoms and effect on social and occupational functioning Assessment Requests, National Center for PTSD (116D), VA Medical Center, 215 North Main Street, White River Junction, VT 05009; website: www.ncptsd.va.gov/publications/assessment/caps.html |
Appropriate symptom scales such as the clinical rating scales included in Table 4-6 in Chapter 4 may also be used. Although all of these measures and the instruments in Tables 10-3 and 10-4 target specific symptoms and manifestations of trauma, the effects of trauma are profound, pervasive, wide ranging, and affect all dimensions of the person: emotional, intellectual, physical, relational, spiritual, vocational, environmental, and psychological. Holistic outcome measurements rather than symptom-specific instruments may more accurately reflect healing. Examples of measures reflecting holistic outcomes may include quality of life, self-efficacy, overall health status, connection to others (i.e., sense of belonging or social support), spiritual well-being, and resilience. Outcome measures are further discussed in Chapter 14.
Evidence-Based Interventions
Empirical research supports the efficacy of CBT and EMDR for treatment of PTSD (Davidson & Parker, 2001; Hembree & Foa, 2000; Rauch & Cahill, 2003). A multidimensional meta-analysis revealed that most patients treated with CBT or EMDR improved significantly (Bradley et al., 2005). Practice guidelines for PTSD and DID include CBT and EMDR as effective treatment modalities (APA, 2004; Department of Veterans Affairs & Department of Defense, 2004; ISSD, 2005). Box 10-3 provides the websites for these guidelines. According to APA guidelines, CBT and EMDR are considered sole treatment interventions, whereas other modalities are considered adjuncts to either of these approaches. Box 10-4 provides a summary of the APA guidelines.
Box 10-3 Practice Guidelines for Trauma
 Treating Patients with Acute Stress Disorder and Posttraumatic Stress Disorder (2004): www.psych.org/psych_pract/treatg/quick_ref_guide/PTSD_ASD_QRGStandalone.pdf
Treating Patients with Acute Stress Disorder and Posttraumatic Stress Disorder (2004): www.psych.org/psych_pract/treatg/quick_ref_guide/PTSD_ASD_QRGStandalone.pdf
 International Society for the Study of Dissociation (ISSD, 2005): Guidelines for Treating Dissociative Identity Disorder in Adults: www.issd.org/indexpage/treatguide1.htm
International Society for the Study of Dissociation (ISSD, 2005): Guidelines for Treating Dissociative Identity Disorder in Adults: www.issd.org/indexpage/treatguide1.htm
 The VA/Department of Defense Practice Guidelines for PTSD: www.oqp.med.va.gov/cpg/PTSD/PTSD_Base.htm
The VA/Department of Defense Practice Guidelines for PTSD: www.oqp.med.va.gov/cpg/PTSD/PTSD_Base.htm
Box 10-4 Psychotherapeutic Interventions for Trauma
* Evidence-based research indicates these methods are effective as sole treatments. † From American Psychiatric Association. (2004). Practice guidelines for the treatment of patients with acute stress disorder (ASD) and posttraumatic stress disorder (PTSD). American Journal of Psychiatry 161(Suppl.), 1-57.
Eye Movement Desensitization and Reprocessing
EMDR has emerged as one of the most innovative and effective approaches to treat symptoms of PTSD in the past decade. Dr. Francine Shapiro (2001) developed EMDR in the late 1980s as a behavioral technique and it is now viewed as an integrative 8 stage approach to psychotherapy. It is based on a comprehensive three-pronged approach, which includes earlier life experience, present-day stressor (i.e., triggers), and desired thoughts and actions for the future. The therapist guides the patient in processing affective, cognitive, or somatic material with procedures and protocols which include some form of bilateral stimulation during a session. The bilateral stimulation may take the form of eyes moving horizontally back and forth, sounds alternating in each ear or alternate tapping on each hand or knee. The goal is to bring the trauma to an “adaptive resolution.” Chapter 11 discusses processing, the evidence-base research for EMDR, and the protocol, and it provides information regarding EMDR post–master’s certification.
Numerous practice guidelines include EMDR as an efficacious treatment for trauma (APA, 2004; Bleich et al., 2002; Crest, 2003; Department of Veterans Affairs & Department of Defense, 2004; Dutch National Steering Committee, 2003; Foa et al., 2000; INSERM, 2004; NICE, 2005; Sjoblom et al., 2003). When comparing exposure and CBT and EMDR, it has been found that all are equally effective. However, EMDR is less time intensive and requires no homework between sessions (Ironson et al., 2002, Lee et al., 2002; Power et al., 2002; Rothbaum et al., 2005; Taylor et al., 2003). Studies of single trauma, in contrast to complex multiple trauma, indicate a 77% to 100% remission of PTSD after three to six EMDR sessions (Lee et al., 2002).
Body and Energy Work
Although not evidence based, body and energy work are thought to be important adjuncts to trauma treatment. A number of trauma experts advocate using body therapies because trauma memories are stored in the brain and manifested in the body (Levine, 2001; Rothschild, 2000; Scaer, 2005; van der Kolk, 2003). van der Kolk reasons that because adults typically process information in a top-down manner (i.e., from their cortex [thinking brain] to the amygdala [emotional brain]), bottom-up therapy from the emotional brain to the thinking brain is important to access trauma memories in a more efficient way (2003). Because psychotherapy is largely a left brain cortex activity, body therapies are thought to be more likely to be effective and access areas involved where implicit memory is stored (e.g., amygdala). Somatic-based therapies are discussed further in Chapter 11.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree

















