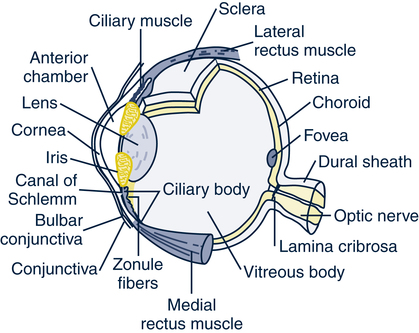
Sabrina Friedman, MSN, PhD, EdD, FNP, CNS On completion of this chapter, the reader will be able to: 1. Describe age-related changes in the senses. 2. Compare and contrast cataracts and glaucoma and the associated nursing interventions. 3. Compare and contrast retinal disorders and the medical and nursing management of each disorder. 4. Identify nursing interventions for older adults with low vision. 5. Describe the proper method for instilling eye medications. 6. Describe the proper method for removing impacted cerumen. 7. Identify safety measures for older clients with vertigo. 8. Identify nursing interventions for older clients with xerostomia. 9. Describe potential hazards for older adults with diminished senses of vision, hearing, and touch. 10. Conduct a sensory system assessment and describe the normal findings. 11. Describe aural rehabilitation methods to use with older adults who are hearing impaired. 12. Identify how activities of daily living are affected by sensory changes. Vision plays an integral part in a person’s ability to function in the environment. Visual acuity (the ability to see clearly) is an important part of performing activities of daily living (ADLs); dressing, grooming, cooking, sewing, driving, and reading are all tasks that involve the use of eyesight (Fig. 31–1). Normal age-related changes in the external and internal eye have been well documented. The eyelids lose tone and become lax, which may result in ptosis of the eyelids, redundancy of the skin of the eyelids, and malposition of the eyelids. Eyebrows may turn gray and become coarser in men, with outer thinning in both men and women. The conjunctiva thins and yellows in appearance. In addition, this membrane may become dry because of diminished quantity and quality of tear production. The sclera may develop brown spots. The cornea yellows and develops a noticeable surrounding ring, made up of fat deposits, called the arcus senilis. The pupil decreases in size and loses some of its ability to constrict. Changes related to aging that decrease the size of the pupil and limit the amount of light entering the eye also occur in the iris. The lens increases in density and rigidity, affecting the eye’s ability to transmit and focus light. Peripheral vision decreases, night vision diminishes, and sensitivity to glare increases (Roach, 2001; Brodie, 2003). The yellowing of the lens results in difficulty identifying certain colors, especially cool colors such as blue, green, and violet (Lueckenotte, 1998). Ophthalmoscopic examination of the retina may reveal the following changes: blood vessels narrow and straighten; arteries seem opaque and gray; and drusen, localized areas of hyaline degeneration, may be noted as gray or yellow spots near the macula (Lueckenotte, 1998). Two common complaints of older adults, floaters and dry eyes, are discussed in the following section. Flashers occur when the vitreous fluid inside the eye rubs or pulls on the retina and produces the illusion of flashing lights or lightning streaks. Flashers that appear as jagged lines, last 10 to 20 minutes, and are present in both eyes are likely to be caused by a spasm of blood vessels in the brain called a migraine. These flashers commonly occur with advancing age, but they warrant prompt medical attention if they increase in number, if a large number of new flashers appears, or if partial loss of side vision is noted (Kollarits, 1998). The nurse should refer a client who experiences any of the above symptoms to an ophthalmologist for a comprehensive eye examination. If no cause is found for the floaters and flashers, the nurse should teach the client about the condition and how to live with it. Clients should be taught to look up and down to get the floaters out of the field of vision. In addition, the nurse should provide the client with the printed information instruction sheet titled “Aging and Your Eyes” so he or she may learn more about floaters and flashers (Kollarits, 1998) (Box 31–1). Treatment consists of tear replacement or conservation. Tears can be replaced by instilling an over-the-counter artificial tear preparation to lubricate the eye and replace missing moisture. This type of preparation may be used as often as necessary, especially before activities that require significant eye movement. Solid inserts that gradually release lubricants throughout the day are also available. An ophthalmologist can conserve the naturally produced tears by temporarily or permanently closing the lacrimal drainage system. Other methods of conservation include use of a humidifier when the heat is on, wraparound glasses to reduce evaporation of eye moisture caused by wind, and avoidance of smoke (Kollarits, 1998). Nursing care is aimed at encouraging the client to adjust to the glasses by wearing them and following up with a visit to the ophthalmologist every 2 years. Clients can be provided with an “Aging and Your Eyes” pamphlet (see Box 31–1) for information about presbyopia. Also, clients and their families can be taught eye health promotion and prevention techniques (see Health Promotion/Illness Prevention Box: The Eye). eyeball. Entropion (turning inward) results in the eyelashes rubbing against the eye, causing corneal abrasion. The lower lashes may not be visible and can cause watering and redness of the eye. Both can be treated by minor same-day outpatient surgery performed by an ophthalmologist. The prognosis for complete recovery and cessation of symptoms is excellent (Brodie, 2003). Glaucoma is the second leading cause of blindness in the United States and the first cause of blindness among blacks. Although glaucoma can occur at any age, those most at risk are adults older than age 60 (Roach, 2001; Gohdes, Balamurugan, Larsen, & Maylahn, 2005). The most common form has few, if any, symptoms and may cause partial vision loss before it is detected. This major public health problem affects approximately 3 million older Americans and is associated with over 120,000 blind older adults (Ebersole, Touhy, Hess, et al, 2008). Chronic open-angle glaucoma, the most common type (making up 90% of all primary glaucoma), develops slowly. Degenerative changes in Schlemm’s canal obstruct the escape of aqueous humor, resulting in increased IOP. This type of glaucoma can damage vision so gradually and painlessly that a person is unaware of a problem until the optic nerve is badly damaged. Visual loss begins with deteriorating peripheral vision (O’Neil, 2002). Potential nursing diagnoses for the client with glaucoma include • Sensory/perceptual alterations (visual) related to decreased peripheral vision • Knowledge deficit: glaucoma causes and treatments related to lack of exposure and inexperience • Pain related to increased IOP • Potential for infection related to eye drop instillation • Dressing and grooming self-care deficit related to visual impairment Nursing management is aimed at teaching the client that glaucoma is a chronic condition requiring lifelong medical treatment. Any current visual loss is permanent, but further loss can be prevented by following the care guidelines outlined in Box 31–2. If medication is unable to control rising IOP, surgical intervention may be necessary. Trabeculectomy requires overnight hospitalization. Postoperative nursing care for the client who has had a trabeculectomy includes (1) routine postanesthesia care, (2) protection of the operative eye with an eye patch or a shield, proper positioning of the client on the back or on the side of the inoperative eye, and the use of a call light and side rails, (3) administration of pain medications and cold eye compresses to maintain comfort, (4) monitoring of the eye for increased IOP, bleeding, or infection, and (5) assistance and teaching of safe, independent performance of ADLs (Monahan, 2006). Nursing diagnoses for the client with cataracts include • Sensory/perceptual alterations (visual) related to a hard and cloudy lens • Anxiety related to uncertain surgical outcome • Knowledge deficit: cataracts related to lack of exposure • Potential for injury related to changes in visual acuity • Dressing/grooming self care deficit related to inability to see body and face clearly enough to maintain appearance of clothes and cosmetics Expected outcomes for a client with cataracts include 1. The client will have cataract surgery when it is recommended by an ophthalmologist. 2. The client will ask questions about preoperative and postoperative care and report satisfaction with information. 3. The client’s affected eye will be free from increased IOP, stress on the suture line, hemorrhaging, and infection. 4. The client will verbalize appropriate home care activities to avoid and activities to do after cataract surgery. 5. The client will demonstrate correct administration of eye drops. 6. The client will avoid falling, bumping into objects, and having automobile accidents before and after surgery. 7. The client will dress and groom himself or herself when vision returns. corrective glasses. The client and family will arrange assistance with ADLs for the first 24 to 48 hours after surgery, or they will notify the home health agency. Age-related macular degeneration (AMD) is the leading cause of blindness among older adults in the United States. It does not cause total blindness but results in loss of close vision. AMD is a poorly understood disease that causes damage to the macula, the key focusing area of the retina. The cells within the macula diminish in functional ability with age, and replacement of the damaged cells is decreased, causing irreversible damage to the macula (Roach, 2001). As a result, there is a decline in central visual acuity that makes daily tasks requiring close vision nearly impossible. Peripheral vision is retained. AMD is viewed as a disease that is becoming an epidemic among older adults (Bressler et al, 2004). • Dry macular degeneration. Also known as involutional macular degeneration, this condition is caused by breakdown or thinning of macular tissue related to the aging process. Vision loss is gradual. • Wet macular degeneration. Also known as exudative macular degeneration, this type of AMD results when abnormal blood vessels form and hemorrhage on the retina. Vision loss may be rapid and severe. AMD is almost exclusively a disorder of whites and is more common in women than in men. Cases tend to cluster in families. Smoking, low dietary intake of antioxidant vitamins and zinc, and sun exposure are some modifiable risk factors (Taylor, 2002). Symptoms of macular degeneration include • Sensory/perceptual alterations (visual) related to damaged macula or retina • Knowledge deficit: effect of diabetes on eyes caused by lack of exposure to accurate information • Knowledge deficit: retinal detachment condition, surgery, preoperative and postoperative care, and home care after surgery
Sensory Function
Vision
Age-Related Changes in Structure and Function
Common Complaints
Floaters and Flashers
Dry Eyes
Common Problems and Conditions
Presbyopia
Ectropion and Entropion
Glaucoma
Chronic Open-Angle Glaucoma
Nursing Management
![]() Assessment
Assessment
![]() Diagnosis
Diagnosis
![]() Intervention
Intervention
Nursing Management
![]() Assessment
Assessment
![]() Diagnosis
Diagnosis
![]() Planning and Expected Outcomes
Planning and Expected Outcomes
![]() Evaluation
Evaluation
Retinal Disorders
Age-Related Macular Degeneration
Nursing Management
![]() Assessment
Assessment
![]() Diagnosis
Diagnosis
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Sensory Function
Get Clinical Tree app for offline access