CHAPTER 16 Progress in nursing: multidisciplinary and shared care
When you finish this chapter you should be able to:
Scope of practice
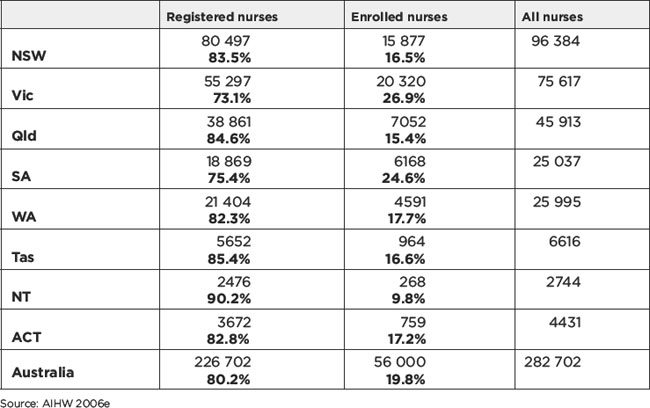
Table 16.1 shows the number of registered nurses (RNs) and enrolled nurses (ENs) in Australia in 2004. Most of the nursing workforce in Australia is comprised of RNs (80.2% of the nursing workforce). The Northern Territory has the highest ratio of RNs to ENs, with 90.2% of the nursing workforce being RNs. Victoria and South Australia have the highest proportion of ENs to RNs, with approximately one-quarter of the nursing workforce in these states working as ENs. In addition, over 49 000 people identified themselves as unlicensed care workers in the 2001 census, accounting for 20.7% of people providing nursing services. This number increased from 18.4% in 1996, suggesting greater use of unlicensed staff to provide care (Australian Institute of Health and Welfare [AIHW] 2003).
Career structure
The career structure is a pathway for career progression for nurses. It draws on the ‘clinical ladder’ system in the US and is influenced by the ‘Dreyfus Model of Skill Acquisition’, adapted to nursing by Benner (1984). The career structure or pathway was introduced to provide a framework for career progression and remuneration for nurses based on an individual nurse meeting defined criteria of skill, competence, professional expertise and education. The rationale for implementing a clinical ladder or career structure was, in part, to recognise nurses who choose to remain at the bedside or in clinical practice rather than go into administration and management or education positions (Zimmer 1972; Gagen 1984; Silver 1986a; Walker 2005). In the early 1970s and 1980s many nursing organisations began to explore the possibility of developing a clinical ladder. The Australian Nursing Federation (ANF) in South Australia was one of the first Australian organisations to develop a career structure. The career structure which they developed was piloted in 1985 and implemented in 1987, and provided a model for other states and territories (Koch et al 1999). The South Australian Career Structure Model delineated five levels of nursing professionals based on skill.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


 Pause for reflection
Pause for reflection