29 Postanesthesia care complications
Acute Myocardial Infarction: Occurs when an area of heart muscle dies or is permanently damaged because of an inadequate supply of oxygen to that area.
Anaphylactic Reactions: Anaphylaxis is a severe whole-body allergic reaction that occurs rapidly and causes a life-threatening response that involves the whole body.
Aspiration: The inhalation of either oropharyngeal or gastric contents into the lungs.
Awareness During Anesthesia: Occurs when a person is aware of some portion of the procedure (sometimes even pain) during general anesthesia; can cause long-term psychologic effects and symptoms of posttraumatic stress.
Bradycardia: A heart rate of less than 60 beats/min (adult) with a regular rhythm and P waves present.
Bronchospasm: Narrowing of the bronchi and bronchioles from smooth muscle contraction that results in wheezing, coughing, and decreased oxygen exchange.
Delayed Emergence (Awakening): Patient emergence from anesthesia is delayed; failure to emerge can be classified as the result of drug effects, metabolic disorders, or neurologic disorders.
Dilutional Hyponatremia: Absorption of irrigating solutions through open blood vessels (during prostate resection) or perforation of the uterine or bladder wall that leads to circulatory overload from water intoxication. May also be caused by excessive free water intake, excess sodium losses, or inappropriate antidiuretic hormone secretion.
Emergence Excitement: A condition characterized by restlessness, disorientation, crying, moaning, irrational talking, and inappropriate behavior.
Hemolytic Transfusion Reactions: An ABO-incompatible blood reaction that precipitates a hemolytic reaction that results in agglutination, or clumping, of red blood cells, which blocks the patient’s capillaries and thus obstructs the flow of blood and oxygen to vital organs.
Hemorrhage: Rapid, copious blood loss.
Hypertension: A blood pressure increased 20% to 30% above the baseline blood pressure.
Hyperthermia: A core temperature of more than 38° C.
Hypotension: A blood pressure that is less than 20% to 30% of the baseline blood pressure.
Hypothermia: A core temperature of less than 36° C.
Hypoventilation: A decrease in respiratory rate and tidal volume that leads to an increase in partial pressure of carbon dioxide (PaCO2).
Hypoxemia: A PaO2 of less than 60 mm Hg.
Laryngospasm: An involuntary partial or complete closure of the vocal cords, caused by secretions, or stimulation or irritation of the laryngeal reflexes during emergence.
Malignant Hyperthermia (MH): A pharmacogenetic (autosomal dominant inheritance) disorder of muscle metabolism involving hypermetabolism that can be triggered by succinylcholine or the volatile anesthetics.
Noncardiogenic Pulmonary Edema: Respiratory disorder that most commonly occurs after an obstructive event that results in pulmonary capillary leakage and pulmonary edema.
Nonhemolytic Febrile Reactions: Most often caused by sensitivity to leukocytes and platelets and seen most often in patients who have received multiple transfusions.
Perforated Viscus: Internal organs perforated during the operative procedure.
Plasma Cholinesterase Deficiency: An uncommon genetic disorder that renders the patient with an inability to metabolize succinylcholine, resulting in prolonged skeletal muscle paralysis and apnea of 2 hours or more.
Pneumothorax: An accumulation of air or gas in the pleural space.
Postdischarge Nausea and Vomiting (PDNV): Nausea or vomiting that occurs after discharge from the health care facility after ambulatory surgery.
Postdural Puncture Headache: A headache that typically develops 24 to 48 hours after lumbar puncture from a spinal needle placement or unintentional dural puncture during an epidural placement.
Postoperative Nausea and Vomiting (PONV): Nausea or vomiting that occurs within the first 24 hours after inpatient surgery.
Pulmonary Edema: Increase in lung fluid as a result of leakage from pulmonary capillaries into the interstitium and alveoli of the lung; leads to impaired gas exchange and may cause respiratory failure.
Pulmonary Embolism: A sudden blockage of an artery in the lungs by fat, air, clumped tumor cells, or a blood clot; usually a blood clot that traveled to the lung from the leg.
Spinal Epidural Hematoma: A hematoma after spinal procedures or surgery; blood accumulates between the spinal dura and bone compressing nerves; without prompt treatment, it can cause permanent neurologic deficits.
Tachycardia: A heart rate greater than 100 beats/min (adult) with a regular rhythm and P waves present.
Transfusion-Related Acute Lung Injury (TRALI): Rare but devastating complication of blood component therapy; findings are similar to adult respiratory distress syndrome and consist of hypotension, fever, dyspnea, and tachycardia.
Respiratory complications
Airway management and respiratory care are first in the mind of the perianesthesia nurse when patients arrive in the postanesthesia care unit (PACU). Avoidance of postoperative pulmonary complications, including atelectasis, pneumonia, respiratory failure, and exacerbation, helps to reduce patient morbidity and mortality rates. The perianesthesia nurse works to prevent these serious longer-term complications by maintaining and improving the patient’s respiratory function in the immediate postanesthesia period of care. Some patients are at greater risk for developing these complications. Primarily these risk factors are related to the patient or the procedure. Box 29-1 lists the most common risk factors supported by evidence.1
BOX 29-1 Risk Factors for Postoperative Pulmonary Complications
Data from Smetana GW, et al: Preoperative pulmonary risk stratification for noncardiothoracic surgery: systematic review for the American College of Physicians, Ann Intern Med 144:581–595, 2006.
Laryngospasm
Laryngospasm is an involuntary partial or complete closure of the vocal cords, caused by secretions or stimulation or irritation of the laryngeal reflexes during emergence. Wheezing, reduced compliance, stridor (partial), paradoxical chest or abdominal movements, and absence of ventilation (complete) are signs and symptoms of laryngospasm. Ventilation is decreased or absent, and oxygenation of the patient is difficult as carbon dioxide builds (PaCO2 increases). Treatment includes airway maneuvers (chin lift/jaw thrust), elevation of the head of bed to maximize respiratory excursion, and application of a bag-valve-mask for continuous positive pressure with oxygen. Secretions need to be carefully removed with suction. The patient may need reintubation to secure the airway if mask ventilation is difficult. Medications include succinylcholine and can include other neuromuscular blocking agents and lidocaine. When the patient has received a neuromuscular blocking agent, the patient may need sedation to reduce anxiety related to apnea, muscle relaxation, and awareness.
Aspiration
Identified as a high-risk low-frequency occurrence, aspiration may be observed in the postanesthesia setting. The patient with a nasal or oropharyngeal airway in place and returning gag reflexes may become nauseated and vomit. In a nonresponsive state and supine position, the patient is at greater risk for aspiration. Types of aspirates include large particle, clear acidic or nonacidic fluid, foodstuff or small particle, and contaminated material. In addition, foreign bodies such as teeth or blood may be aspirated. Symptoms include unexplained tachypnea and tachycardia, cough, bronchospasm, hypoxemia, atelectasis, interstitial edema, hemorrhage, and acute respiratory distress syndrome. The aspiration can trigger laryngospasm, infection, and pulmonary edema. Prevention of aspiration is preferred. Patients at risk should be identified before surgery and premedicated. Patients at risk are patients with emergent procedures, known full stomachs, or history of gastroesophageal reflux disease; those older than age 65 years; and women in labor. Medications include histamine blockers, nonparticulate antacids, and anticholinergic agents. During surgery, rapid sequence induction and nasogastric tube placement may help to minimize the risk of aspiration. After surgery, maintenance of the endotracheal tube until airway reflexes have returned and positioning of the patient with the head to the side or in a left lateral decubitus position can aid in decreasing the risk of aspiration. If aspiration occurs, hypoxemia should be corrected and hemodynamic stability maintained. The patient may need reintubation and suctioning and mechanical ventilation. Arterial blood gases assist in planning respiratory management of the patient. A chest radiograph is obtained, but findings may be inconclusive initially; radiographic findings may lag behind clinical signs by 24 hours after the suspected aspiration event. Prophylactic antibiotics or steroids are not recommended. Tracheal secretions should be cultured; if results are positive, antibiotics can be prescribed.
Noncardiogenic pulmonary edema
Noncardiogenic pulmonary edema may be the result of upper airway obstruction, laryngospasm, bolus dosing with naloxone, incomplete reversal of neuromuscular blockade, or a significant period of hypoxia. When the cause is obstructive in origin, two types of postobstructive pulmonary edema (POPE) have been identified: type I and type II.2 Both are present with acute respiratory distress. Type I usually occurs within 60 minutes of a precipitating event, but onset can be delayed up to 6 hours. Type I POPE may follow postextubation laryngospasm, epiglottitis, croup, choking or foreign body, strangulation, hanging, endotracheal tube obstruction, laryngeal tumor, goiter, mononucleosis, postoperative vocal cord paralysis, migration of the urinary catheter balloon used for tamponade epistaxis, near drowning, and intraoperative direct suctioning of an endotracheal tube adapter.3 Type II POPE develops soon after relief of chronic upper airway obstruction, such as after tonsillectomy or adenoidectomy, removal of upper airway tumor, choanal stenosis, and hypertrophic redundant uvula.3
Signs and symptoms include hypoxemia, cough, failure to maintain oxygen saturation levels, tachypnea, and frothy sputum. Treatment includes supplemental oxygen administration and maintenance of a patent upper airway. CPAP may be used. Patients with an inability to maintain a patent airway may need intubation and mechanical ventilation with PEEP. For patients with significant compromise, hemodynamic support and continued observation in an intensive care unit may be needed. Patients with noncardiogenic pulmonary edema typically recover rapidly after the intense initial phase and leave the critical care unit within approximately 24 to 36 hours and without permanent sequelae from the event.
Pulmonary embolism
Patients predisposed to development of pulmonary emboli include patients who are obese or immobile, who are undergoing pelvic or long bone procedures, and who have a history of congestive heart failure or malignant disease.4 Signs and symptoms can include tachypnea, pleuritic chest pain, hemoptysis, breathlessness, and a sense of impending doom. Treatment is supportive for correction of hypoxemia and hemodynamic instability. Intravenous heparin and morphine sulfate can be given to help stabilize the pulmonary capillary membrane. Prevention of venous thromboembolism and subsequent pulmonary emboli development includes subcutaneous unfractionated heparin, low–molecular-weight heparins, or intermittent or sequential compression devices.
Cardiovascular complications
Major cardiovascular perioperative risks are identified as myocardial infarction, heart failure, and death. Clinical predictors of increased perioperative cardiovascular complications are listed in Box 29-2.5
BOX 29-2 Clinical Predictors of Increased Perioperative Cardiovascular Complications
Active cardiac conditions—major (delay or cancel surgery unless emergent)
Data from Fleisher LA, et al: 2009 ACCF/AHA focused update on perioperative beta blockade incorporated into the ACC/AHA 2007 guidelines on perioperative cardiovascular evaluation and care for noncardiac surgery, J Am Coll Cardiol 54(22):e13–e118, 2009.
Tachycardia
Sinus tachycardia occurs commonly in the postanesthesia setting. Causes include hypoxia, hypercarbia, hypovolemia, sepsis, hyperthermia, heart failure, pain, drugs, and psychologic stress. Treatment includes administration of supplemental oxygen, ventilation support, and evaluation of fluid and cardiac status. If the condition results from pain, medication with analgesics is the treatment. Sedatives may be needed if the condition is from anxiety or stress. If the patient is hyperthermic, the patient’s core temperature is lowered with recommended cooling devices. Tachycardia in patients with coronary artery disease can increase the risk of myocardial ischemia.
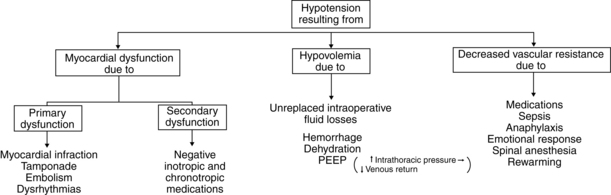
Hypotension
Hypotension is defined as blood pressure that is less than 20% to 30% of the baseline blood pressure.6 Causes range from use of an inappropriately sized cuff, to hypovolemia, myocardial dysfunction, and a decrease in systemic vascular resistance (Fig. 29-1). Management and treatment of hypotension in the PACU includes use of a cuff of the appropriate size, administration of supplemental oxygen, initiation of fluid resuscitation, stoppage of drug infusions if causative, and elevation of the legs. Inotropic agents or vasopressor or vasoconstrictive agents may be ordered.
Hypertension
Hypertension is defined “as persistent elevation of systolic blood pressure greater than 140 mm Hg or a diastolic blood pressure greater than 90 mm Hg or requires an antihypertensive treatment.”7 Too small or narrow of a cuff can result in abnormally elevated blood pressures. Pain, stress, hypoxemia, hypercarbia, fluid overload, delirium, drugs, bladder, bowel or stomach distention, or hypothermia can cause hypertension. Many of the patients in PACU in whom hypertension develops have preexisting hypertension. The elevation in blood pressure is usually benign and short lived; however, the hypertension can precipitate myocardial ischemia in the patient with coronary artery disease as a result of stimulation of the sympathetic nervous system. Treatment for hypertension includes use of an appropriately sized cuff and identification and management of the underlying cause first. This condition may necessitate ventilatory support and oxygen administration, analgesics or sedatives, bladder decompression, and antihypertensive agents.
Patients who have had a cervical or thoracic spinal cord injury (above T6) are at risk for developing autonomic dysreflexia, which is a massive uninhibited sympathetic cardiovascular response to noxious stimuli (e.g., bowel or bladder overdistention) characterized by paroxysmal hypertension, pounding headache, facial flushing, sweating, temporal or neck vessel engorgement, nasal congestion, blurred vision, chill bumps, chills, nausea, and occasional bradycardia. Treatment includes elimination of the precipitating stimuli if known and elevation of the head of bed. Pharmacologic treatment may be needed to reduce the blood pressure if the blood pressure remains elevated after these measures. Medications for the treatment of hypertension include nifedipine, nitrates, captopril, prazosin, phenoxybenzamine hydrochloride, prostaglandin E2, and sildenafil.8
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree