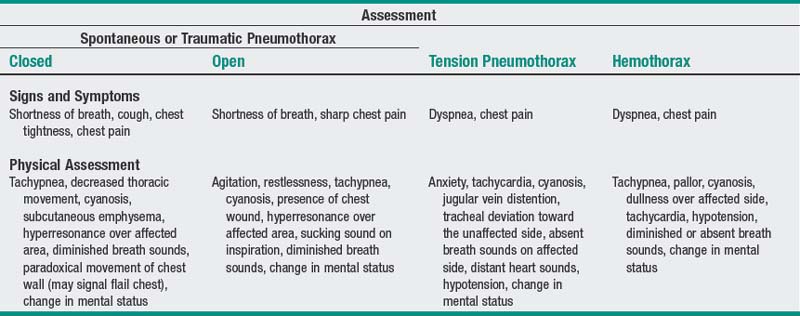
11 Pneumothorax/hemothorax
Complete blood count (CBC):
May reveal decreased hemoglobin proportionate to amount of blood lost in a hemothorax.
Nursing diagnosis:
Ineffective breathing pattern
| ASSESSMENT/INTERVENTIONS | RATIONALES |
|---|---|
| Assess patient’s mental, respiratory, and cardiac status at frequent intervals (q2-4h, as appropriate). | This assessment monitors patient’s status while chest drainage system is in place. The purpose of a chest drainage system is to drain air or fluid and reexpand the lung. Diminished breath sounds, along with tachycardia, restlessness, anxiety, and changes in mental status, are signs of respiratory distress that may occur as a result of chest drainage system malfunction. If these signs are present, prompt intervention is necessary to prevent further hypoxia and distress. |
| Assess and maintain closed chest drainage system as follows: < div class='tao-gold-member'> Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|