Newborn Feeding
Objectives
3. Explain the physiologic characteristics of lactation.
4. Discuss the dietary needs of the lactating mother.
5. Compare the nutrients of human milk with those of cow’s milk.
7. Compare various maternal and newborn positions used during breastfeeding.
8. Identify principles of breast pumping and milk storage.
9. Illustrate techniques of formula feeding.
10. Discuss the various types of formula and their preparation.
Key Terms
colostrum (kă-LŎS-trŭm, p. 207)
engorgement (ĕn-GŎRJ-mĕnt, p. 206)
foremilk (p. 207)
galactogogues (găh-LĂK-tō-gŏgs, p. 204)
hindmilk (HĪND-mĭlk, p. 207)
lactation (lăk-TĀ-shŭn, p. 206)
latch-on technique (p. 211)
let-down reflex (p. 206)
milk-ejection reflex (p. 206)
oxytocin (ŏks-ē-TŌ-sĭn, p. 206)
prolactin (prō-LĂK-tĭn, p. 206)
satiety (să-TĪ-ĕ-tē, p. 208)
 http://evolve.elsevier.com/Leifer/maternity
http://evolve.elsevier.com/Leifer/maternity
For many women, breastfeeding or bottle feeding the newborn is a satisfying but sometimes anxiety-provoking task. Besides providing essential nutrition, feeding is an important mechanism in the formation of the newborn’s emotional development and the trusting relationship between the newborn and the mother or family. The decision whether to breastfeed or bottle (formula) feed is usually made during pregnancy.
Feeding the newborn should be an enjoyable and pleasurable task for both the newborn and the parent. It is a time when the parent and newborn can get to know each other. The nurse plays an important role in assisting the mother in either breastfeeding or bottle feeding her newborn. Education, including discussion of common concerns, will help the parents smoothly assume one of their important new tasks of parenting.
Cultural Influences
Cultural attitudes and beliefs vary about breastfeeding the newborn. Modesty and embarrassment may prevent the woman from breastfeeding in the hospital, and she may prefer to begin to breastfeed after she is home. This is often true of mothers from Asian and Muslim cultures. Mormon women believe that breastfeeding is an important part of motherhood. Mothers from some cultures believe that colostrum is unclean and therefore should not be given to newborns. Some recent or first-generation immigrants to the United States come from countries where breastfeeding is the norm and see formula as a symbol of a new way of life.
The hot-cold theory of health and illness is common to many cultures. Because the postpartum period is considered a “cold” condition, only approved “hot” foods are eaten after delivery. Chicken, honey, rice, and hot soup may be preferred, whereas salads and iced drinks will be refused even by a hungry mother. In some cultures, mothers use galactogogues (breast milk stimulators), and the nurse must be aware of such requests in the form of beer, brewer’s yeast, or sesame tea.
Health care personnel who casually ask whether women are planning to breastfeed or bottle feed may imply that they are equal in value if the advantages and disadvantages are not carefully explained (Table 11-1). Americans value fast food and may not realize the ready convenience and low cost of breast milk compared with formula. When a mother plans to return to work after the birth of the baby, she may not know that her breast milk can be easily expressed, stored, and fed by bottle by the caregiver. Although one of the goals of Healthy People 2010 was to have 75% of new mothers breastfeed, and the American Academy of Pediatrics (AAP, 2007) recommends breastfeeding as the optimum nutrition for newborns that should be continued through the first year and beyond, the final decision is with the parents. The nurse’s role is to educate the parents concerning their choices, promote feelings of confidence and competence in feeding techniques, and accept the feeding choice of the parents. Nurses should be alert to mothers who need encouragement if they desire to breastfeed but who may not do so because of a lack of knowledge and support.
Table 11-1
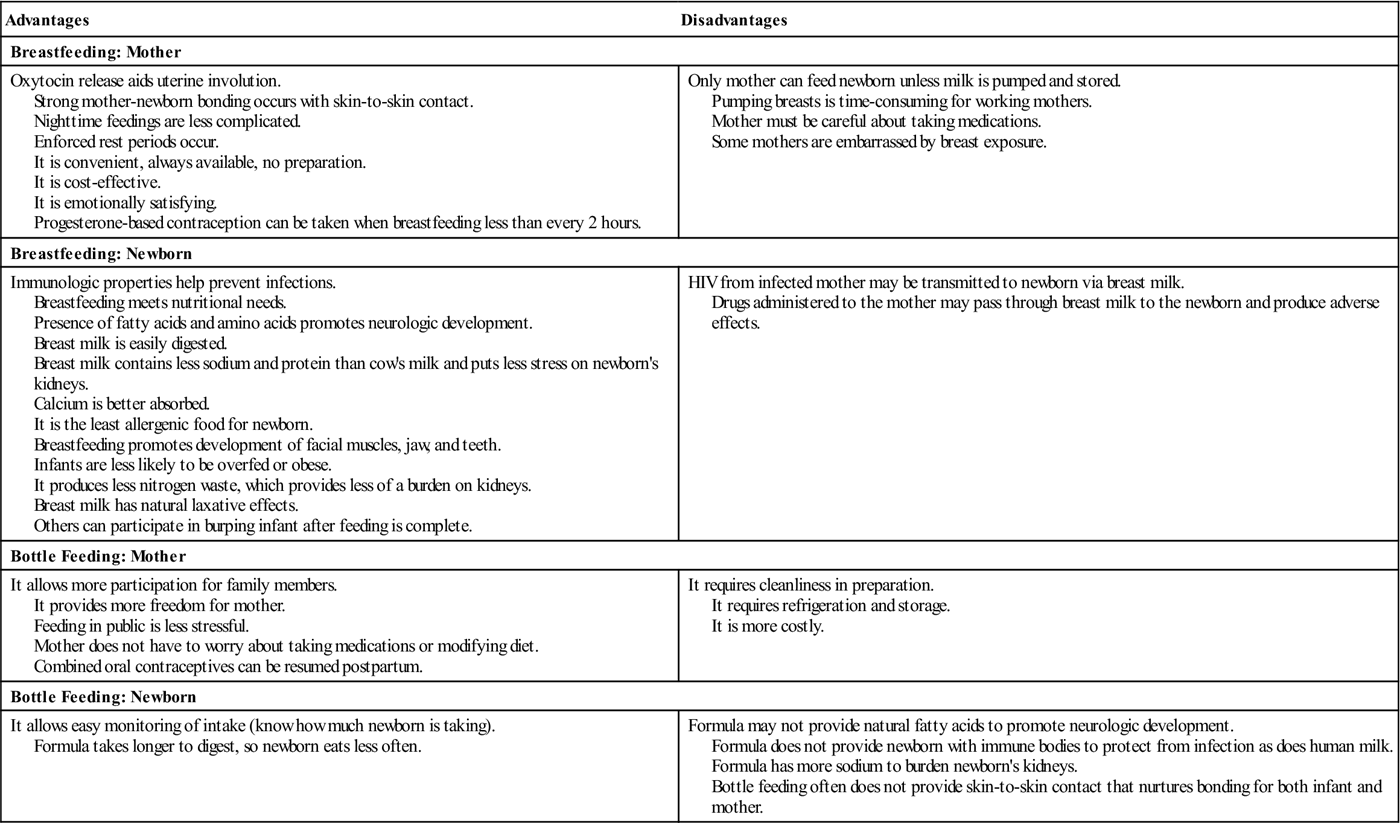
Advantages and Disadvantages of Breastfeeding and Bottle Feeding
| Advantages | Disadvantages |
| Breastfeeding: Mother | |
| Oxytocin release aids uterine involution. Strong mother-newborn bonding occurs with skin-to-skin contact. Nighttime feedings are less complicated. Enforced rest periods occur. It is convenient, always available, no preparation. It is cost-effective. It is emotionally satisfying. Progesterone-based contraception can be taken when breastfeeding less than every 2 hours. | Only mother can feed newborn unless milk is pumped and stored. Pumping breasts is time-consuming for working mothers. Mother must be careful about taking medications. Some mothers are embarrassed by breast exposure. |
| Breastfeeding: Newborn | |
| Immunologic properties help prevent infections. Breastfeeding meets nutritional needs. Presence of fatty acids and amino acids promotes neurologic development. Breast milk is easily digested. Breast milk contains less sodium and protein than cow’s milk and puts less stress on newborn’s kidneys. Calcium is better absorbed. It is the least allergenic food for newborn. Breastfeeding promotes development of facial muscles, jaw, and teeth. Infants are less likely to be overfed or obese. It produces less nitrogen waste, which provides less of a burden on kidneys. Breast milk has natural laxative effects. Others can participate in burping infant after feeding is complete. | HIV from infected mother may be transmitted to newborn via breast milk. Drugs administered to the mother may pass through breast milk to the newborn and produce adverse effects. |
| Bottle Feeding: Mother | |
| It allows more participation for family members. It provides more freedom for mother. Feeding in public is less stressful. Mother does not have to worry about taking medications or modifying diet. Combined oral contraceptives can be resumed postpartum. | It requires cleanliness in preparation. It requires refrigeration and storage. It is more costly. |
| Bottle Feeding: Newborn | |
| It allows easy monitoring of intake (know how much newborn is taking). Formula takes longer to digest, so newborn eats less often. | Formula may not provide natural fatty acids to promote neurologic development. Formula does not provide newborn with immune bodies to protect from infection as does human milk. Formula has more sodium to burden newborn’s kidneys. Bottle feeding often does not provide skin-to-skin contact that nurtures bonding for both infant and mother. |
Success or failure that a mother achieves in breastfeeding may determine her feelings about being an adequate mother; therefore, the choice to breastfeed is an important one. The mother needs to be comfortable with what she is doing and enjoy the experience for breastfeeding to be successful.
Americans value breastfeeding as a natural right and have supported laws that allow breastfeeding in public. Knowledge of breastfeeding laws can create a more supportive breastfeeding environment. Nurses play an important role in supporting breastfeeding legislation and educating parents concerning their rights and resources. As of 2004, only two states, Oregon and Utah, had met the Healthy People 2010 goals of having 75% of mothers’ breastfeed (Centers for Disease Control and Prevention [CDC], 2005).
Laws that foster a supportive environment for breastfeeding may encourage mothers to breastfeed even when not at home. Breastfeeding-supportive laws include clarification that breastfeeding is not part of indecent exposure, lewd conduct, or sexual misconduct in public (National Conference of State Legislators, 2010). A federal bill, H.R. 2236, may have allowed breast pumps to be a deductible medical expense. The National Alliance for Breastfeeding Advocacy (NABA) collaborates with many organizations to promote a supportive social environment for breastfeeding. Currently, NABA is designing a universal logo that is posted at public sites, such as airports, to indicate protected breastfeeding sites, much like the universal logo for men’s or women’s restrooms.
Maternal Nutrition During Lactation
The mother must maintain her own nutritional stores while providing for the infant through breastfeeding. The mother needs 500 calories more than her nonpregnant diet each day, selected from the various major food groups. Protein intake should be 65 mg/day, and calcium intake should match pregnancy requirements. Vitamin supplements taken during pregnancy are often continued during lactation. It is recommended that 8 to 10 glasses of noncaffeinated liquids be consumed each day. Some foods eaten by the mother may change the taste of her breast milk or cause the infant to have gas. If a mother suspects a certain food she consumes is causing fussiness or gas in the infant, she can eliminate it from her diet for a few days to determine whether the infant has fewer problems.
Many drugs taken by the mother can be passed to the infant via breast milk and should be taken on the advice of a health care provider only. In some cases, timing the drug dose so that it passes its peak of activity before the infant is put to the breast can reduce the amount delivered to the infant. See Chapter 4 for drug-risk categories, Chapter 5 for specific nutritional needs for pregnant and lactating women, and Chapter 21 for common herbs used or contraindicated during lactation.
Physiology of Lactation
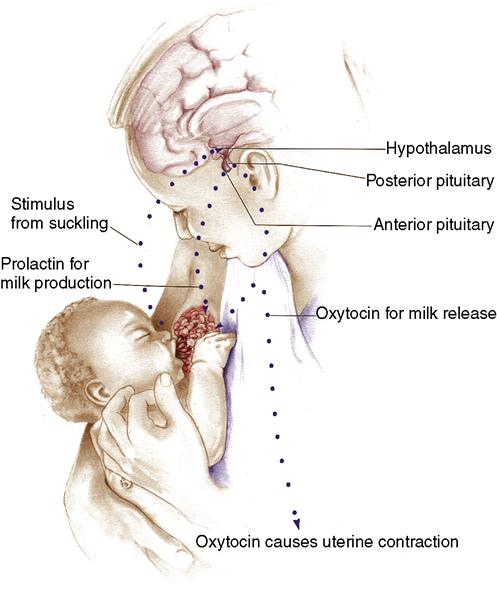
Lactation (the secretion of milk) is the end result of many interacting physiologic factors, including the development of breast tissue and duct system, primarily under the influence of hormones (estrogen, progesterone, and human placental lactogen [hPL]). In addition, hPL stimulates the alveolar cells of the breast to begin lactogenesis (milk production), so that, by the later part of pregnancy, the breasts secrete colostrum, a thick, creamy fluid. After the birth of the newborn and the delivery of the placenta, the hormones estrogen, progesterone, and hPL decrease rapidly, causing a rapid increase of prolactin secretion. Prolactin, secreted from the anterior pituitary gland, stimulates milk production, which is then enhanced by newborn suckling. Suckling also causes the posterior pituitary to secrete oxytocin, producing the let-down reflex, or milk-ejection reflex, which causes the milk to be delivered from the alveoli (milk-producing sacs) through the duct system to the nipple (Figure 11-1). The mother usually feels a tingling in her breasts when this reflex occurs. The woman also often feels abdominal cramping because oxytocin stimulates the uterus to contract, which helps with postpartum uterine involution.
By the third or fourth postpartum day the prolactin effect on the breast tissue is evident, and the hormone is present in sufficient amounts to cause engorgement (congestion or distention) of the breasts. At this time, milk begins to replace the colostrum. Once lactation has been established, suckling is the most important stimulus for the maintenance of milk production.
Breast Milk
Three types of milk are produced during the establishment of lactation: colostrum, transitional milk, and mature milk. Colostrum is produced for the first 3 or 4 postpartum days; it contains high levels of antibodies, protein, minerals, and fat-soluble vitamins. Although it is high in protein, it is fairly low in sugar and fat and is therefore easy to digest. It is rich in immunoglobulin (antibodies), which helps protect the newborn’s gastrointestinal tract from infections. Therefore, colostrum helps establish the normal intestinal flora in the intestines, and its laxative effect speeds the passage of meconium.
Transitional milk comes in the period between colostrum and mature milk, which is about 5 days to 2 weeks. The composition of the milk changes, and lactose, fat, and calories increase. Mature milk, the final milk produced, looks similar to skim milk (somewhat bluish), which leads some mothers to question whether their milk is rich enough to give to their newborns. Nurses need to explain that mature milk contains approximately 22.5 kcal/oz and is just right to meet the newborn’s needs (Table 11-2).
Table 11-2
Human Milk Versus Commercial Formula
| Nutrient | Human Milk | Cow’s Milk-Based Formula |
| Protein | Lower amount but sufficient; contains more lactalbumin (because easy digestible, provides ideal quantity) | Greater; contains more casein, which forms large curds that take longer to digest |
| Fat | Varies; lowest in morning and highest in afternoon; used rapidly because of enzyme lipase; easier to digest Contains omega-3 fatty acids to promote neurologic development | Fat poorly absorbed (commercial formulas often add fat source such as corn oil) |
| Carbohydrate | Lactose higher (7%) Lactose improves absorption of calcium; also promotes growth of normal bacterial flora in intestines | Lactose less (4.8%) Some formulas add DHA and fatty acids |
| Iron | Small amount but better absorption than cow’s milk Lactoferrin in human milk enhances iron absorption | Small amount |
| Calcium, phosphorus, sodium, and potassium | Lower amount of these minerals; imposes a lower solute load on newborn’s kidneys | Greater amount results in renal solute load |
| Immunoglobulins | IgA, IgG, IgM protect newborn from infections (diarrhea, respiratory infections, and gastroenteritis) | None |
| Antiallergic factors | Infants rarely allergic to human milk May protect from development of allergies (less eczema in newborns) | Allergy to cow’s milk possible |
The percentage of calories derived from protein is lower in breast milk than in formulas, with a greater proportion of calories from carbohydrates in the form of lactose. The amount of fat in breast milk varies during the feeding; there is more fat present in the hindmilk, the milk produced at the end of the feeding, than at the beginning (foremilk).
Breast milk contains enzymes that aid digestion. Lipase in breast milk helps the newborn digest fat. Fluoride is present in breast milk if the mother drinks fluoridated water. However, a supplement of fluoride may be prescribed in the form of newborn vitamins with fluoride if the family uses bottled water or well water. Fluoride is needed for the development of healthy tooth enamel.
The immunologic benefits include protection against several bacterial and viral diseases, especially those of the respiratory and gastrointestinal tracts. Lactoferrin, which is secreted in human milk, is believed to play a part in controlling bacterial growth in the gastrointestinal tract. Immunoglobulin A, present in colostrum and breast milk, protects against the development of many allergies. Immunoglobulins to the poliomyelitis virus are also present in the breast milk of mothers who have a passive immunity to the virus (see Table 11-2). Breast milk also contains long-chain polyunsaturated fatty acids and amino acids that promote eye and neurologic development. The level of docosahexaenoic acid (DHA) (an omega-3 fatty acid) in breast milk is directly related to the amount of DHA ingested by the mother in her diet. Sources of omega-3 fatty acids include fish such as salmon, herring, mackerel, and lake trout and oils such as canola, hempseed, soy, walnut, and soybeans (see Chapter 5). The World Health Organization (WHO) recommends adding DHA to formula feedings to benefit the central nervous system, cognitive, behavioral, and eye development of the newborn (Blanchard, 2006).
Breastfeeding
Preparing the Breasts
Flat or inverted nipples can be treated during pregnancy, but interventions can begin after birth. Flat nipples can be rolled between the mother’s fingers just before feeding to help them become more erect so that the newborn can more easily grasp them. Hoffman’s exercise can be started after the newborn is born. In Hoffman’s exercise, the fingers are placed on the areola and gently pulled apart to stretch the tissue. This helps release adhesions that may cause the nipple to be inverted. The exercise is repeated with movement of the fingers around the areola. Babies can usually learn to breastfeed even if the nipple is not completely erect. Newer ultra thin nipple shields are artificial nipples, usually made of a soft, thin material and worn over the nipple of the mother’s breast; they may be used in special cases such as nipple soreness or latch-on problems. However, prolonged use can result in decreased milk production because the maternal milk sinuses are not compressed adequately by the suckling newborn. Lengthy weaning of the infant to the natural breast nipple may also become a problem. The use of breast shields should be monitored by a lactation specialist.
Preparations for the mother include voiding, washing her hands, and assuming a comfortable position. The importance of the mother washing her hands before putting the newborn to the breast should be emphasized because the hands are the primary source for the spread of infection.
Many hospitals have a lactation specialist who is available to assist the woman in breastfeeding. On discharge, the mother should be given the telephone number of a referral group, such as the La Leche League, that will assist her with a telephone call if a problem arises. Lactation specialists also have private practices, making home visits for a consultation fee (Figure 11-2).
Frequency and Length of Feedings
Because breast milk is digested more quickly than formula (usually within 2 hours), the newborn needs to be fed every 2 to 3 hours. Also, in the beginning, the newborn’s stomach capacity is small. Newborns who are fed frequently during the daytime may, on average, have longer sleep periods during the night. Until meconium is passed, the newborn may consume 15 to 30 mL per feeding. By 1 week of age, the neonate will consume 60 to 90 mL during each feeding.
Readiness for feeding can be determined by observing the newborn’s behavior. Rooting, sucking, hand-to-mouth activity, crying, and alertness are clues that the newborn is hungry. Crying is often a late sign of hunger. Mothers often notice the sensation of the let-down reflex (tingling, fullness, stinging) or have milk leakage when they think of getting ready to nurse. This can also happen when they hear the newborn cry. The let-down reflex can be inhibited or stimulated by the mother’s state of mind (embarrassment or anxiety about breastfeeding). Generally, the newborn is placed for approximately 15 minutes of suckling on the first breast, followed by the other breast until the infant is satisfied. The mother should allow the first breast to completely empty before placing the infant on the other breast. Parents should be informed that short pauses in suckling are normal during nursing.
The average time for breastfeeding is 15 to 20 minutes per breast. If the feedings are too short, the infant may get only the foremilk and will be hungry sooner if he or she does not get to the richer hindmilk. Engorgement can occur if milk is not removed from the breast, and milk production will decrease if suckling is not adequate to empty the breast. The infant should be burped after feeding. The next breastfeeding session should begin on the breast opposite the one started at the last session (alternate starting breasts). The mother should be taught to take her cues from the newborn to determine when the newborn is full, such as the slowing of the newborn’s suckling pattern; the newborn falling asleep; and the mother’s breasts feeling soft and empty, which indicates satiety (fullness to satisfaction).
The anxious mother may ask how she can tell whether the newborn is getting enough milk. The nurse can help the parent listen for sounds of swallowing as the newborn sucks and identify changes in behavior that indicate newborn satiety, such as falling asleep after breastfeeding. Having at least six wet diapers and several stools in a 24-hour period is also indicative of adequate intake. Palpating the breasts before and after breastfeeding will also reveal a change from firm, engorged breasts to soft, “empty” breasts after breastfeeding. These signs of successful breastfeeding will be reinforced by the weight gain the newborn shows after the first week and during the follow-up clinic visits.
Teaching Feeding Techniques
Positioning
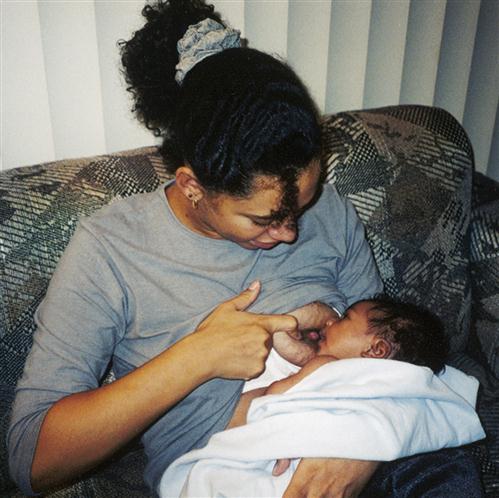
Both the mother and the newborn must be comfortable during breastfeeding. Using different positions is important because this varies the pressure points on the nipple and areola, which helps prevent nipple soreness. The mother may prefer the cradle hold, football hold, or side-lying position (Figure 11-3).
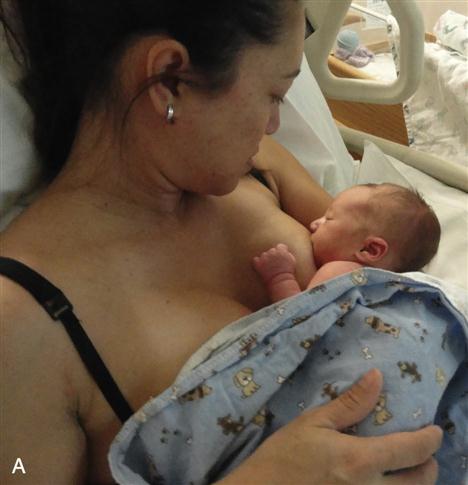
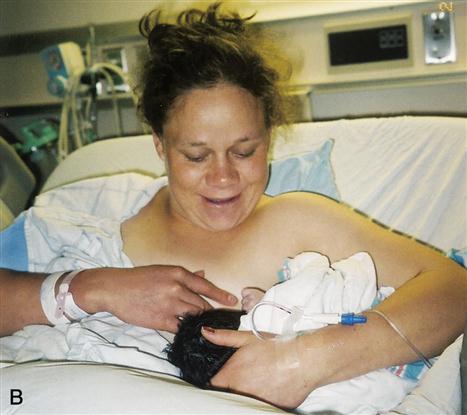
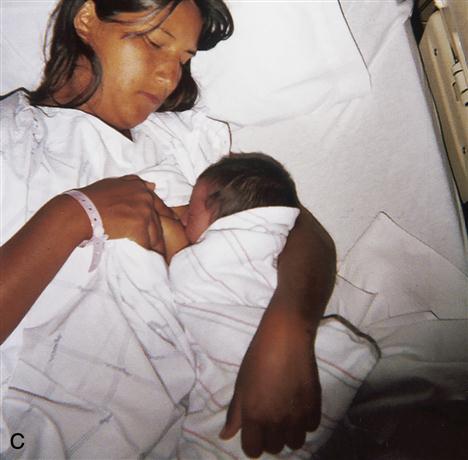
Some mothers prefer to sit up in bed or in a chair and hold the infant in a cradle hold with the infant’s head in the mother’s antecubital area. To prevent fatigue, the infant’s body can be supported by a pillow, and the mother’s arm should be supported by pillows or the armrest of the chair. The newborn must be in a chest-to-chest position with the mother to avoid the need to turn the head to latch on to the nipple. Turning of the infant’s head may interfere with swallowing and places pressure on the mother’s nipple, which can result in discomfort.
With the football hold, the mother supports the newborn’s head, with the body resting on pillows alongside her hip. This hold allows the mother to see the position of the newborn’s mouth on the breast; this position is helpful for mothers with large breasts. This position also avoids pressure against an abdominal incision.
The side-lying position avoids pressure on the episiotomy or the abdominal incision from a cesarean birth. Pillows are placed behind the mother’s back to increase her comfort. Folded blankets or pillows can be used to elevate the newborn to breast level so that there is no tension on the nipple. Pulling on the nipple can make it tender and sore. The newborn’s head and body should directly face the breast (Figure 11-4).
Hand Position
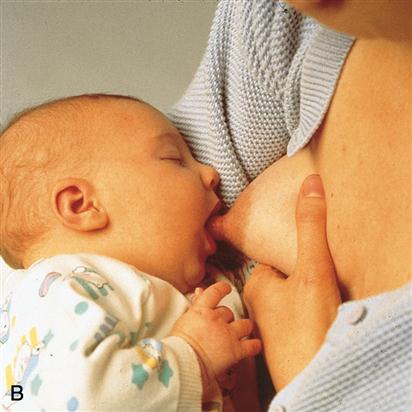
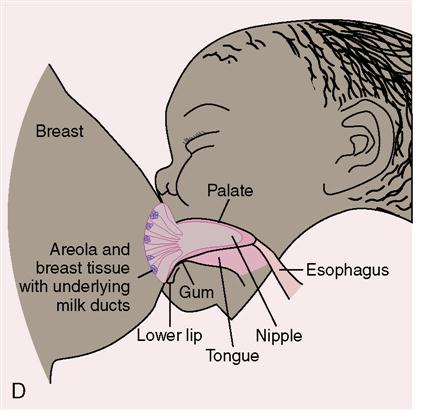
Once the newborn is properly positioned, the mother should hold her hand in a C position, supporting the breast from below and placing her thumb above the nipple and her fingers below the areola. It is important for the newborn to get enough of the areola in his or her mouth; otherwise, suckling will be directly on the nipple. For the newborn to obtain milk from the breast, the jaws must compress the milk sinuses beneath the areola (Figure 11-5). The tongue should be visible between the lower gum and breast. The lips are widely flanged and sealed around the breast, with an absence of clicking sounds as the newborn sucks. Because the newborn is a nose breather, make sure the newborn’s nose is not blocked by breast tissue. For women with large breasts, the breast tissue can be indented by the finger away from the newborn’s nose; however, care must be taken to avoid pulling the nipple out of the newborn’s mouth. The mother can elevate the newborn’s hips, which provides more breathing space.
Correct positioning before beginning to breastfeed is significant in getting a good start and preventing problems. Four separate elements that need consideration are (1) the alignment of both the mother’s and newborn’s bodies; (2) the position in which the mother holds the newborn; (3) the hand position for supporting the breasts; and (4) the newborn’s mouth, lip, and tongue positions.
Sucking Patterns
Newborns have different sucking patterns when they breastfeed. Some newborns suck several times before swallowing, and others swallow with each suck. A soft sound indicates that the newborn is swallowing milk (nutritive sucking). Noisy sucking, a clicking sound, or dimpling of the cheeks usually indicates improper mouth position and requires repositioning of the infant.
Initiating Breastfeeding
The ideal time to initiate breastfeeding is within 1 hour after birth, when the newborn is in the quiet-alert phase. After positioning the newborn to face the breast, the mother can slightly compress the breast and, with her thumb above and fingers below the areola, stroke or brush the nipple against the newborn’s lower lip or stroke the mouth. This stimulates the rooting reflex, causing the newborn to turn toward the nipple. As the newborn’s mouth opens wide, the mother quickly brings the newborn close to her so that the newborn can latch on to the areola (Skill 11-1). This is referred to as the latch-on technique. In other words, the mother guides the nipple into the newborn’s mouth, pulling the baby close to her. As much of the areola as possible should be in the newborn’s mouth to avoid sore nipples. Later, when her milk comes in, the mother can listen for the sound of swallowing (sometimes gulping) the milk (Clinical Pathway 11-1).
If the breasts are full, expressing some milk softens the breasts and makes it easier for the newborn to grasp the areola. Also, the breast can be softened by massage.
Removal from the Breast
The mother is taught to safely remove the newborn from the breast for burping, for switching to the other breast, and when the infant is finished being fed. To avoid trauma to the breast, the newborn should be removed properly. The mother should insert her finger into the corner of the newborn’s mouth to break the suction, and then remove the breast quickly before the newborn begins to suck again. Downward pressure on the newborn’s chin is another way to break the suction (Figure 11-6). The principles of teaching the mother how to breastfeed are listed in Table 11-3 and Nursing Care Plan 11-1 on p. 217.
Table 11-3
Teaching the New Mother How to Breastfeed
| Instruction | Rationale |
| Wash hands before feeding; wash nipples with warm water, no soap. | Prevents infection of the newborn and breast; plain water prevents nipple cracking and irritation. |
| Position self (sitting or side-lying). | Alternating positions facilitates breast emptying and reduces nipple trauma. |
| Sit comfortably in chair or raised bed with back and arm support; hold newborn by cradle hold or football hold supported by pillows. | Pillow support of mother’s back and arm and the newborn’s body in any position reduces fatigue; newborn is more likely to remain in correct position for nursing. |
| Lie on side with pillow beneath head, arm above head; support newborn in side-lying position. | Side-lying position reduces fatigue and pressure on abdominal incision. |
| Turn body of newborn to face mother’s breast. | Prevents pulling on nipple or poor position of mouth on nipple. |
| Stroke newborn’s cheek with nipple. | Elicits rooting reflex to cause newborn to turn toward nipple and open mouth wide. |
| Newborn’s mouth should cover entire areola. | Compresses ducts and lessens tension on nipples; suction is more even. |
| Avoid strict time limits for nursing; nurse at least 10 minutes before changing to other breast or longer if newborn is nursing vigorously. | Let-down reflex may take 5 minutes; a too-short feeding will give newborn foremilk only, not the hunger-satisfying hindmilk. Strict time limits do not prevent sore nipples. |
| Use safety pin on the bra strap as a reminder about which breast to start with at the next feeding. | Alternating which breast is used first increases milk production. |
| Lift newborn or breast slightly if breast tissue blocks nose. | Provides a small breathing space. |
| Break suction by placing finger in corner of newborn’s mouth or indenting breast tissue. | Prevents nipple trauma. |
| Nurse newborn after birth and every 2-3 hours thereafter. | Early suckling stimulates oxytocin from mother’s pituitary to contract her uterus and control bleeding. Breast milk is quickly digested. Early, regular, and frequent nursing reduces breast engorgement. Skin-to-skin contact promotes bonding. |
| Burp newborn halfway through and after feeding. | Rids stomach of air bubbles and reduces regurgitation. |
From Leifer, G. (2010). Introduction to maternity and pediatric nursing (6th ed.). Philadelphia: Saunders.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree