32 Care of the ear, nose, throat, neck, and maxillofacial surgical patient
Ankyloglossia (Tongue Tied): A short lingual frenulum that may cause difficulty with suckling in the infant and subsequent speech impairment. It is treated surgically with clipping of the frenulum.
Cochlear Implant: A prosthesis with an internal electrode is surgically implanted into the cochlea so that an external microphone later can be applied for stimulation of the eighth cranial nerve and provision of sound for a deaf person.
Electrocautery Unit: A snare heated with electricity for the purpose of cauterization of small vessels to bleeding or for cutting tissue, without blood loss.
Endoscopy: Nasal surgery performed with direct vision with endoscopic equipment.
Ethmoidectomy: Removal of ethmoid bone.
Fenestration: Reconstruction of the outer and middle parts of the ear by means of a new drum or skin flap; creation of a new window into the internal ear mechanism with a newly established drum or skin flap.
Glossectomy: Removal of the tongue.
Intranasal Antrostomy (Antral Window): Creation of an opening in the lateral wall of the nose under the middle turbinate and the removal of the anterior end of the inferior turbinate.
Labyrinthectomy: Opening of the labyrinth to destroy the inner ear in an attempt to relieve medically uncontrollable symptoms of unilateral Meniere disease.
Laryngectomy: Removal of the larynx; total laryngectomy is the complete removal of the cartilaginous larynx, the hyoid bone, and the strap muscles connected to the larynx and the possible removal of the preepiglottic space along with the lesion.
Laryngofissure: Opening of the larynx for exploratory, excisional, or reconstructive procedures.
Laryngoscopy: Direct examination of the interior of the larynx with a laryngoscope.
Mastoidectomy: Removal of mastoid air cells and of the tympanic membrane. Radical mastoidectomy also involves removal of the malleus, incus, chorda tympani, and mucoperiosteal lining.
Myringotomy: Incision of the tympanic membrane with direct vision and insertion of tubes for facilitation of drainage.
Ossiculoplasty: Reconstruction of the ossicular chain.
Palatouvuloplasty: The reconstruction of the posterior section of the palate and the uvula.
Radical Antrostomy (Caldwell-Luc Operation): Use of an incision into the canine fossa of the upper jaw and exposure of the antrum for removal of bony diseased portions of the antral wall and contents of the sinus; establishment of drainage by means of a counteropening into the nose through the inferior meatus to create a large opening in the nasoantral wall of the inferior meatus, which ensures adequate gravity drainage and aeration and permits removal of all diseased tissue in the sinus with direct vision.
Semi-Fowler Position: The patient is in an inclined position, with the upper half of the body raised with elevation of the head of the bed by approximately 30 degrees.
Sensorineural Hearing Loss: The sound is conducted normally through the external and middle ear, but a defect in the inner ear or auditory nerve results in a loss or deficit in hearing.
Serosanguineous: A discharge from the body that is composed of serum and blood.
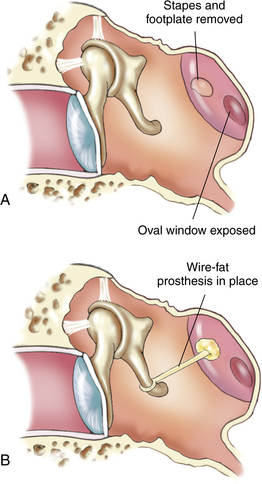
Stapedectomy: Removal of the stapes, followed by the placement of a prosthesis.
Stents: A rod for supporting tubular structures.
Submucosal Resection: Removal of either cartilaginous or osseous portions of the septum that lie between the flaps of the mucous membrane and the perichondrium for establishing an adequate partition between the left and right nasal cavities, thereby providing a clear airway for both the internal and the external cavities and the parts of the nose.
Tonsillectomy and Adenoidectomy (T&A): Surgical removal of the tonsils and adenoids.
Tracheostomy: Opening of the trachea and insertion of a cannula through a midline incision in the neck below the cricoid cartilage.
Tympanoplasty (Myringoplasty): Reconstruction of the tympanic membrane.
The patient with ear, nose, and throat (ENT) dysfunction presents many challenges to the perianesthesia nurse. These patients often have a difficult airway for management (see Chapter 30), which in itself can be challenging. These patients also often have abnormal or dysfunctional anatomy that presents major concerns and requires enhanced awareness of the “normal” anatomy of the structures associated with ENT surgical procedures. In addition, the patient emerging from maxillofacial surgery, which usually consists of dental or plastic surgery, needs close monitoring of airway patency and clearance along with management of the pain associated with those surgical procedures in a way that does not depress respiratory status. The perianesthesia nurse who manages these types of surgical procedures needs a strong knowledge of airway anatomy and physiology and excellent skills in the management of a difficult airway. Finally, the perianesthesia nurse must also manage the behavioral component of patients who undergo ENT or maxillofacial surgery. These patients have all kinds of emotions: from fright because of wiring of the jaw to fear because of the tight bandaging and pain. Because patients who undergo ENT and maxillofacial surgery present a great challenge to the perianesthesia nurse, a complete review of this category of surgical patients is presented. The reader is encouraged to read Chapters 12 and 30 as follow-up; they present more information on the respiratory system and airway management.
Surgery on the ear
Otologic surgery has been revolutionized by antibiotics, the operating microscope, new and more delicate instruments, and an increased understanding of the anatomic structures involved (Fig. 32-1). New methods have been devised for the surgical treatment of hearing loss with correction of conduction apparatus abnormalities, and selected patients can now be surgically relieved of the disabling symptoms of sensorineural hearing loss.
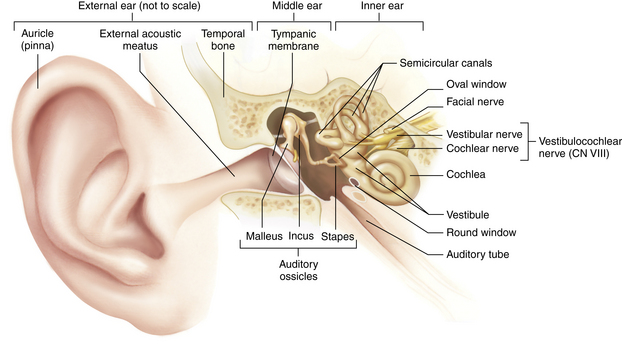
FIG. 32-1 Frontal section through outer, middle, and internal ear. CN, Cranial nerve.
(From Thibodeau GA, Patton KT: Anatomy and physiology, ed 7, St. Louis, 2010, Mosby.)
Most otologic procedures are performed in the day surgery arena. The immediate postanesthesia care for patients who have undergone surgery on the ear is generally the same, regardless of the procedure. Immediate postoperative complications are rare. Occasionally excessive bleeding may occur, especially if a large blood vessel has been entered during the operation. If bleeding has occurred, the incident should be reported to the postanesthesia care unit (PACU) nurse who provides care for the patient on admission. Immediate postanesthesia assessment should follow the same format as for any patient who undergoes general anesthesia.1 In addition, postanesthesia assessment should include testing for function of the facial nerve. The patient should be instructed to frown, smile, wrinkle the forehead, close the eyes, bare the teeth, and pucker the lips.2 An inability to perform these actions indicates injury to the facial nerve and should be appropriately indicated in the patient’s medical record and reported to the surgeon.
If surgery has been performed near the brain (e.g., the inner ear), check for clear fluid in the ear or on the dressings that may indicate cerebrospinal fluid leakage. Aseptic technique for all dressings and protection from infection are especially important elements in the care of the patient who has undergone surgery on the ears, because infection can be transmitted easily to the meninges and the brain. The outer ear is highly vascular and susceptible to circulatory damage and excoriation. The outer ear may even become necrotic if circulation is impaired by poor positioning or excessive pressure of a dressing. Assessment of the dressing should therefore include proper positioning.2,3
Nausea, vertigo, and nystagmus commonly occur in patients after ear surgery. The patient may minimize discomfort by remaining in the position ordered, moving slowly, and avoiding quick jerky movements.2,3 The patient should be advised to take slow, deep breaths through the mouth to minimize nausea. Antiemetic drugs and sedatives, such as a 5-HT3 antagonist (e.g., ondansetron [Zofran]) may be ordered for prevention or treatment of nausea and vertigo. The nurse should avoid jarring the bed. When approaching the patient, the nurse should place a hand on top of the patient’s head as a reminder not to turn suddenly when the nurse speaks. Sudden turns should be avoided, and movement should be slow in patient transport. Particular attention must be paid to maintaining the integrity of the airway should nausea and vomiting occur.
Special considerations
Myringotomy
Myringotomy is the most common procedure performed on infants and small children; it is performed for eustachian tube dysfunction. Often these children will exhibit frequent ear infections or symptoms of pain, poor coordination, hearing loss, or speech delays.4 After a hole in the tympanic membrane is created with a myringotomy blade, the surgeon will place a tube to maintain patency. There are several types of tubes and are placed according to the surgeon’s preference.5
Special pediatric considerations must be given in the immediate postanesthesia phase to airway management, safety, parental involvement, and outpatient teaching.3 This procedure is commonly bilateral in children; however in adults it is commonly unilateral.4 A small piece of sterile cotton can be placed loosely in the external ear to absorb the drainage that commonly occurs. The cotton should be changed when saturated to avoid contamination.
Mastoidectomy
A firm bulky dressing is placed over the ear and held in place with a circular head bandage after mastoidectomy.5 This dressing may be reinforced, if necessary, but should be changed only by the physician. Minimal serosanguineous drainage may be expected, but bright bloody drainage should be reported to the surgeon.
The patient should be placed in a position of comfort, usually on the nonoperative side. Grafts are often taken from the arm or leg for radical mastoidectomy, and the donor sites should be assessed for drainage and treated according to facility or department policy and surgeon preference. Dizziness and vertigo are common after mastoidectomy and can be treated with the previously mentioned measures.2,3
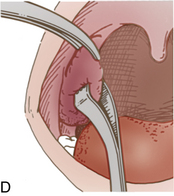
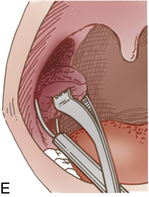
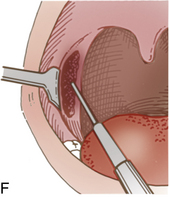
Stapedectomy
Patients who have undergone stapedectomy are usually admitted to the PACU with ear packing in place; this packing should not be disturbed5 (Fig. 32-2). Occasionally patients have vertigo after surgery. Patients should be advised to avoid blowing the nose, coughing, and sneezing.
Cochlear implant
Patients who have undergone a cochlear implant need the same postanesthesia care as any other patient for ear surgery. Verification of the integrity of the facial nerve is important. These patients do not have hearing immediately after surgery and need emotional support and a means of communication such as pen and paper, white board and markers, or a sign language interpreter.3
Surgery on the nose and sinuses
Nasal and sinus surgery can be accomplished with local or general anesthesia. The disposition of the patient is determined by the nature and type of surgery and anesthesia and by the perianesthesia course related to complications and sedation required in the PACU.6 Although no longer common with the use of endoscopic procedures, overnight observation of the patient in an inpatient setting may be necessary before discharge from the hospital. An inpatient stay may be considered for patients with comorbidities such as obstructive sleep apnea because they will have some difficulty with use of the CPAP machine owing to the nasal splints or packing.7 The anatomy of the nasal cavity is shown in Fig. 32-3.
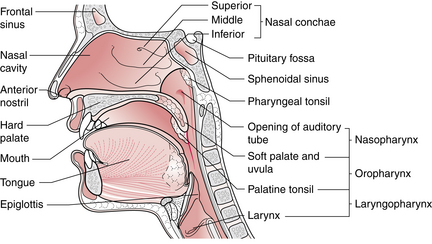
FIG. 32-3 Sagittal section of the nose, mouth, pharynx, and larynx.
(From Watson R: Anatomy and physiology for nurses, ed 13, London, 2011, Baillière Tindall.)
Nasal surgery
Conscious patients admitted to the PACU after nasal surgery, such as septoplasty or functional endoscopic sinus surgery, should be placed in a semi-Fowler position to promote drainage, reduce local edema, minimize discomfort, and facilitate respiration. Some postoperative serosanguineous drainage is expected; however, the nurse should observe closely for gross bleeding.2 Loss of vision is a complication that may indicate orbital hematoma required immediate attention by the surgeon. The patient is usually admitted with one or both nostrils packed and a mustache dressing in place to catch any drainage from the packing.5 The position of the nasal packs and the amount of drainage should be checked frequently. The mustache dressing may be changed as necessary; two or three changes within a 4-hour period are not unusual. Another method commonly used to facilitate postoperative drainage is the insertion of nasal stents. This approach affords more comfort and permits nasal breathing.
The back of the patient’s throat should be checked frequently for blood. Frequent belching (from the accumulation of blood in the stomach), frequent swallowing, and the classic signs of hemorrhage, such as tachycardia, are additional signs of unusual bleeding.3 The patient should be instructed not to blow the nose or swallow secretions, but to spit them into a basin. An ample supply of disposable tissues along with an emesis basin should be placed within easy reach of the patient.
Airway obstruction or laryngeal spasm can occur if a postnasal pack accidentally slips out of place.1 A flashlight, scissors, and a hemostat for emergency removal of nasal packing and emergency airway equipment must be kept readily available at the patient’s bedside.
Sinus surgery
After surgery on the sinuses, the patient is usually admitted to the PACU with packing or splints in place. Reports of feelings of numbness in the upper lip and teeth are not unusual. After general anesthesia, the patient should be positioned well on one side to prevent aspiration of drainage. The conscious patient should be placed in a semi-Fowler position, with the head elevated 45 degrees to promote drainage and minimize edema. The same general care, including oral hygiene and instructions to the patient not to blow the nose, should be followed as for the patient with nasal surgery.1–3
Surgery on the tongue
The tongue occupies a large portion of the floor of the mouth. Surgery on the tongue generally involves excision of benign or malignant lesions, correction of congenital anomalies, or repair of traumatic lacerations. Lesions may be excised without associated neck dissection; however, when the lesion is malignant, surgical treatment usually involves a combined operation that may include radical neck dissection and resection of both the mandible and the tongue.2,5
Maintenance of the airway is the most crucial nursing concern. Suctioning equipment with soft-tipped catheters must be immediately available at the bedside.1,3 The patient should be instructed to allow saliva to run out of the mouth. A wick of gauze is placed in the patient’s mouth to assist in the elimination of secretions. Swelling of the tongue can occur and obstruct the airway; therefore an intubation tray should be readily available.
Because of the vascular nature of the tongue and oral cavity, postoperative bleeding may be a problem. If excessive bleeding occurs, local pressure should be applied until the surgeon can be notified and repair can be performed in the operating room.
Throat surgery
Surgery on the throat and neck is generally accomplished with general anesthesia.6 Aside from routine care and assessment, specific postanesthesia care for the patient who has undergone surgery on the throat involves: (1) close observation for bleeding from the surgical site; (2) maintenance of a patent airway; (3) prevention of aspiration of secretions; and (4) awareness of possible cerebral neurologic complications that may develop.
The most common procedures are tonsillectomy, either alone or in combination with adenoidectomy, and tracheostomy.8 Other procedures that are performed on the throat include laryngoscopy with or without biopsies and laryngectomy.
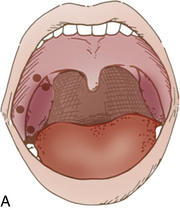
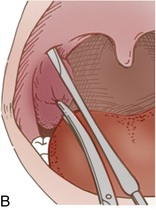
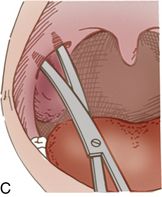
Tonsillectomy and adenoidectomy
Most patients who undergo tonsillectomy (Fig. 32-4) and adenoidectomy (T&A) are children and young adults. However, the number of the young children for T&A continues to be reduced each year as a result of excellent antibiotic treatment. Patients who have undergone T&A and are admitted to the PACU fully conscious can be positioned on their backs with the head elevated 45 degrees. Patients who return after general anesthesia and who are unconscious or semiconscious must be placed in the tonsillar position—well over on the side with the face partially down. The Trendelenburg position can be used to facilitate drainage. The patient’s airway and chest expansion must be in full view of the nurse to ensure maximal respiratory integrity at all times. In this position, secretions are easily drained from the mouth.2 An oral airway should be left in place until the swallowing reflex has returned and the patient can handle secretions. The patient should be advised to spit out secretions as much as possible and to try not to cough, clear the throat, blow the nose, or talk excessively. An ice collar can be applied to minimize pain and postoperative bleeding. The administration of cool humidified air to the patient after T&A provides comfort, helps to minimize swelling, and supplies oxygen. As soon as oral intake is permitted, ice chips should be offered to moisten the throat and reduce swelling.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree