57 Cardiopulmonary resuscitation in the pacu
Antiarrhythmics: A group of drugs used to suppress abnormal rhythms of the heart.
Cardiopulmonary Arrest: The cessation of normal circulation of the blood because of failure of the heart to contract effectively.
Cardiopulmonary Resuscitation (CPR): An emergency procedure that is performed in an effort to return life to a person in cardiac arrest.
Chest Compression: An emergency procedure that is performed on a person in cardiac arrest in an effort to create artificial circulation by manually pumping blood through the heart.
Defibrillation: A treatment for the life-threatening cardiac arrhythmias that consists of delivering a therapeutic dose of electrical energy to the heart, which depolarizes a critical mass of the heart muscle, terminates the arrhythmia, and allows normal sinus rhythm to be reestablished via the patient’s sinoatrial node.
Differential Diagnosis: A systematic method, essentially a process of elimination, used to identify unknowns.
Vasopressors: Sympathomimetic drugs that mimic the effects of the sympathetic nervous system.
Cardiopulmonary emergencies are common in the postanesthesia care unit (PACU). PACU and perianesthesia nurses must keep their cardiopulmonary resuscitation (CPR) skills and knowledge base up to date to most effectively respond to this potentially devastating event. In October 2010, the American Heart Association (AHA) Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care (ECC) were published in Circulation. This CPR update was based on an international evidence-based evaluation process involving hundreds of resuscitation experts.1
Ethical issues related to cardiopulmonary resuscitation
Many patients are increasingly concerned about the inappropriate use of life-sustaining procedures that can have a dramatic effect on the length and quality of life. Consequently, increasing numbers of patients place limitations on medical treatments that may affect their lives in the future, through the use of living wills, advanced directives, do-not-resuscitate (DNR) orders, and no-CPR programs. Living wills allow a person to express preferences concerning end-of-life medical care. Some states have adopted DNR and no-CPR programs with focus on the use or extent of resuscitation efforts. Advanced directives are usually prepared by the physician attending critically or terminally ill patients who are unable to make decisions for themselves. These directives are based on the patient’s living will, if one exists. The patient’s right to limit medical interventions is firmly established in modern medical practice.2,3
The operating room, however, is one area in which restrictions on cardiopulmonary resuscitation have caused considerable ethical conflicts between patients and health care providers. Approximately 75% of all cardiac arrests in the operating room are related to specific anesthesia or surgical causes, such as an accidental overdose of an anesthetic agent. In these circumstances, resuscitation has been found to be highly successful. As such, many health care providers view honoring a patient’s DNR order as failure to treat a reversible process and thus similar to committing murder.3,4 One could argue that the same ethical dilemma exists in the PACU because it is so closely aligned with surgery. All the various ethical dilemmas concerning DNR orders that may arise in the PACU and other topics related to advanced directives are beyond the scope of this chapter. As such, PACU nurses must be thoroughly familiar with their individual institution’s policies and guidelines concerning these issues.
Cardiopulmonary resuscitation
Urgency of cardiopulmonary resuscitation
During cardiopulmonary arrest, time is a factor that profoundly influences patient outcomes. The probability of survival decreases rapidly with each minute of cardiopulmonary compromise. The survival rate from cardiac arrest caused by ventricular tachycardia decreases approximately 7% to 10% for each minute the patient is deprived of defibrillation.5 Therefore the PACU nurse must respond quickly and efficiently during all cardiopulmonary emergencies.
Indications for resuscitation
Respiratory compromise appears to be the primary cause of morbidity in the PACU. Respiratory compromise can result from residual anesthesia, upper airway obstruction, laryngeal edema, laryngospasm, bronchospasm, noncardiogenic pulmonary edema, and aspiration.6
One of the most common causes of upper airway obstruction in the postanesthetic patient results from mechanical obstruction from the tongue. This situation occurs when the tongue falls back into a position that mechanically obstructs the pharynx and thus blocks the passage of air to and from the lungs. The underlying cause of this obstruction may be the result of residual anesthetics, opioids, or muscle relaxants administered during surgery. The tongue may also be edematous from surgical manipulation, anatomic deformities, or allergic reaction. Clinical signs of this type of obstruction include snoring, flaring of the nostrils, use of accessory muscles for ventilation, retraction of the intercostal spaces and suprasternal notch, asynchronous movements of the chest and abdomen, tachycardia from hypoxia, and decreased oxygen saturation.3,6
Arterial carbon dioxide pressure (PaCO2) increases 6 mm Hg during the first minute of total obstruction, with an additional 3 to 4 mm Hg increase each passing minute.7 If the obstruction is not corrected, the patient’s condition will continue to deteriorate resulting in cardiopulmonary arrest. This occurrence is especially tragic when the obstruction could have been corrected by simply stimulating the patient to take deep breaths or by repositioning the airway via a chin lift or jaw thrust. (These maneuvers will be discussed in more detail later.) Additional techniques include the use of a nasal or oral airway. When deciding which of these two airways to use, the PACU nurse should remember that the nasal airway is usually less stimulating and thus tolerated better in the patient emerging from general anesthesia. The nasal airway should, however, not be used with patients with known or suspected basal skull fractures, because of the possibility of inadvertent intracranial placement of the airway. Nasal airways should also not be used with patients presenting with severe coagulopathy due to the increased incidence of nasal bleeding associated with insertion of the nasal airway.8
If the obstruction persists, advanced airway management procedures with the esophageal-tracheal Combitube, Laryngeal Tube or King LT, laryngeal mask airway, or endotracheal tube may be indicated. Obviously, prevention of cardiopulmonary arrest is more desirable than treatment. When a cardiopulmonary arrest does occur, emergency procedures must be administered rapidly and decisively before irreversible damage occurs.8
Emergency equipment
The routine use of various monitoring modalities in the PACU is invaluable for the diagnosis of many developing patient complications that could precipitate a cardiopulmonary arrest. The use of pulse oximetry, for example, can be extremely helpful in the diagnosis of problems concerning patient oxygenation, as in the case of a progressing airway obstruction. The use of a capnograph may be helpful in the early detection of adverse respiratory events such as hypoventilation. The routine use of an ECC monitor assists the nurse in identifying life-threatening arrhythmias such as pulseless ventricular tachycardia (VT), ventricular fibrillation (VF), asystole, and pulseless electrical activity (PEA). These and other monitoring modalities provide the nurse with a more definitive means of diagnosis and opportunity for early intervention.8
Management of cardiac arrest
Assess for responsiveness
At the first sign of potential trouble, the nurse should immediately assess the responsiveness of the patient. The last thing the nurse wants to do is prematurely call a code and start CPR only to find out that the patient had just fallen asleep and one of the electrocardiogram (ECG) leads was loose or disconnected. At the same time the PACU nurse is checking the patient’s responsiveness, the patient’s breathing status should also be assessed; this should be a visual inspection for abnormal (only gasping) or lack of breathing.9
Circulatory assessment
Once unresponsiveness has been confirmed and the emergency system has been activated, the PACU nurse should immediately precede with the AHA basic life support and advanced cardiac life support protocols. The nurse should now proceed to evaluate the patient’s circulatory status. For an adult and child, this assessment is performed by palpating the carotid artery for no more than 10 seconds. If the patient is an infant, the brachial artery should be palpated.9
If a pulse is detected, the patient’s lungs should be ventilated using one of the unit’s readily available bag-mask devices. Respirations should be delivered at a rate of one breath every 5 to 6 seconds or approximately 10 to 12 breaths/min. Each breath should be given over 1 second and cause a visible chest rise. The patient’s pulse should be checked every 2 minutes. This process should continue until the emergency response team can determine and correct the underlying cause of the respiratory arrest or initiate more advanced treatment.9
If no pulse is detected within 10 seconds, the 2010 AHA Guidelines for CPR and ECC state that cardiac arrest should be assumed and CPR initiated immediately. These guidelines recommend initiating a CPR sequence of (1) chest compressions, (2) airway, and (3) breathing (CAB). Anytime during this sequence, defibrillation should be initiated as soon as a defibrillator is available.9
Cardiopulmonary resuscitation
Chest compressions
As stated previously, cardiac arrest can be caused by four heart rhythms: VF, pulseless VT, PEA, and asystole. VF consists of disorganized electrical activity in which VT consists of organized electric activity of the ventricular myocardium. The electrical activity exhibited in these rhythms is insufficient to generate enough forward blood flow to sustain life. PEA encompasses a group of organized electrical rhythms with insufficient or absent mechanical ventricular activity. Although this rhythm may generate ventricular electrical activity on the monitor, the ventricle does not mechanically respond, resulting in the absence of a clinically detectable pulse. PEA has previously been referred to as electromechanical dissociation or nonperfusing rhythm. Asystole, also known as ventricular asystole, consists of the absence of detectable ventricular activity with or without atrial electrical activity.8
Ventricular fibrillation and pulseless ventricular tachycardia
During the first few minutes of witnessed VF cardiac arrest, the primary limiting factor for the delivery of oxygen to the heart and brain is blood flow and not arterial oxygen content. As a result, in the initial step of CPR, uninterrupted chest compressions take priority over positive pressure ventilation.8 External cardiac compression should be performed with the patient in a horizontal position on a firm surface. If a bed board is to be used, care must be taken not to delay the initiation of compressions while one is being retrieved. If the patient is on an air-filled mattress, the mattress should be deflated when performing CPR.10
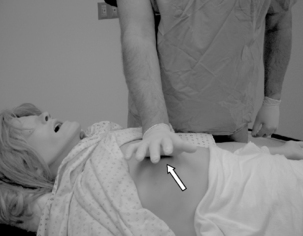
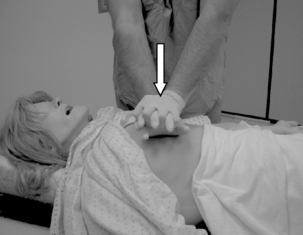
To begin compressions, the rescuer should be positioned at the patient’s side. The rescuer should place the heel of one hand on the center (middle) of the chest between the patient’s nipples (the lower half of the sternum; Fig. 57-1). The heel of the rescuer’s free hand should be placed on top of the hand already positioned on the patient’s chest. The rescuer should keep the arms straight with shoulders directly over the adult patient’s sternum. The adult sternum should be depressed at least 2 inches (5 cm; Fig. 57-2). Rescuers should “push hard, push fast” at a rate of at least 100 compressions/min. Evidence appears to support the premise that this rapid compression rate effectively benefits the patient in terms of blood flow and blood pressure. Interruptions to chest compression should always be minimized to as few as possible with each interruption lasting less than 10 seconds. The chest should be allowed to completely recoil after each compression. Incomplete recoil has been associated with high intrathoracic pressures and decreased hemodynamics, including decreased coronary perfusion, cardiac index, myocardial blood flow, and cerebral perfusion. If two rescuers are present, it is recommended that they rotate giving compressions every 2 minutes. This is done to prevent rescuer fatigue, which can lead to decreased compression effectiveness such as insufficient rate, depth of compression, and incomplete recoil of the chest. It has been found that significant fatigue and shallow compressions are common after 1 minute of CPR, although the rescuer might not recognize that fatigue affecting effective compressions is present. Rescuers should consider switching roles during any intervention that is associated with appropriate interruptions in chest compressions such as defibrillation. The rescuers should strive to accomplish this switch in less than 5 seconds.9 The actual ratio between ventilations and chest compressions will be discussed in the third segment of the CABs, which addresses breathing.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree