T
Tracheostomy
Description
A tracheostomy is a surgically created stoma (opening) in the trachea to establish an airway. It is used to (1) bypass an upper airway obstruction, (2) facilitate removal of secretions, or (3) permit long-term mechanical ventilation.
Most surgical tracheostomies are done in the operating room using general anesthesia. These are typically done electively on patients already intubated who require prolonged mechanical ventilation. When swelling, trauma, or upper airway obstruction prevents endotracheal intubation, an emergent surgical tracheostomy may be performed at the bedside.
A minimally invasive percutaneous tracheostomy can also be performed at the bedside using local anesthesia and sedation and analgesia. A needle is placed into the trachea, followed by a guide wire. The opening is progressively dilated until it is large enough for insertion of a tracheostomy tube.
■ The patient can eat with a tracheostomy because the tube enters lower in the airway (Fig. 24). Speaking is also permitted once the tracheostomy cuff can be deflated.
When the patient can adequately exchange air and expectorate secretions, the tracheostomy tube can be removed. Close the stoma with tape strips and cover it with an occlusive dressing. Instruct the patient to splint the stoma with the fingers when coughing, swallowing, or speaking.
Nursing management
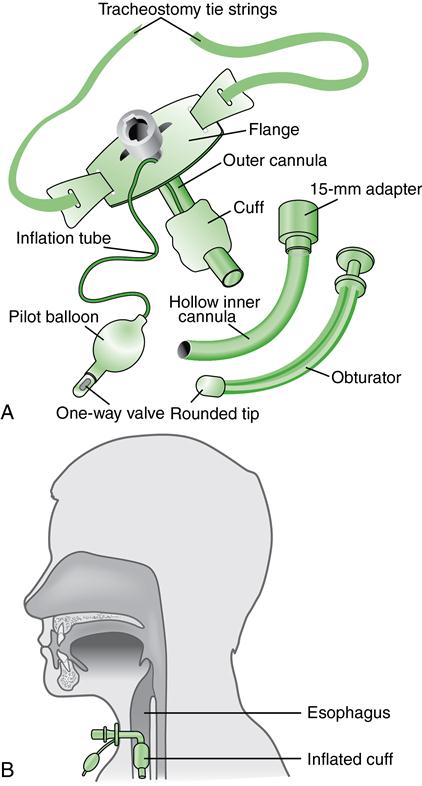
Before the tracheotomy, explain to the patient and family the purpose of the procedure and inform them that the patient will not be able to speak if an inflated cuff is used. A variety of tubes are available to meet patient needs (see Fig. 25). Characteristics and nursing management of tracheostomies are described in Table 27-5, Lewis et al.: Medical-Surgical Nursing, ed. 9, p. 508.
Care should be taken not to dislodge the tracheostomy tube during the first 5 to 7 days when the stoma is not mature (healed).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree