17. Principles of elimination management
obtaining urinary and stool specimens
CHAPTER CONTENTS
24-hour urine collection131
Urine specimens from the baby131
Role and responsibilities of the midwife133
Summary133
Self-assessment exercises133
References133
LEARNING OUTCOMES
Having read this chapter the reader should be able to:
• describe the procedure for obtaining a catheter specimen, a mid-stream specimen and a neonatal specimen of urine
• describe how a 24-hour urine collection is taken
• describe how a stool specimen is obtained
• summarise the midwife’s role and responsibility in relation to specimen collection.
Specimens should be obtained correctly to increase the reliability of the results. The midwife may be best placed to appreciate that a specimen is indicated, but care should be taken to avoid unnecessary specimen collection as it is resource heavy and can be stressful for the woman. This chapter considers how the range of urine and stool specimens is obtained.
Catheter specimens of urine
Urine may be taken from a catheterised woman for the purposes of urinalysis (e.g. infection screening) but occasionally a catheter may be inserted (often residual) to obtain an uncontaminated specimen (e.g. protein urinalysis when pre-eclamptic). This section focuses on obtaining a catheter specimen of urine (CSU) from an indwelling catheter. It is important that the following principles are applied:
• sterility, for both accuracy of the result and prevention of infection
• maintaining a closed drainage system, also for prevention of infection (specimens should only be taken when absolutely necessary)
• fresh urine is screened
• correct technique, sample bottle and dispatch to laboratory within the required time for the nature of the test
• recording of the test to avoid duplication
• collected in a manner that protects staff, including laboratory staff (Higgins 2008a).
Depending on the manufacturer, the type of urinary drainage bag will determine the way in which the specimen is taken:
• a resealing rubber ‘window’ port in the tubing
• a needle-less port in some part of the tubing or drainage bag (Fig. 17.1).
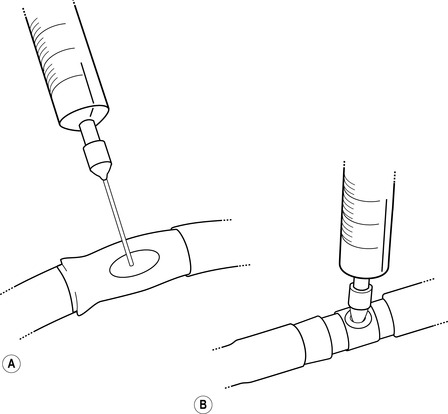 |
| Figure 17.1 • A Rubber resealing needle sampling port. B needle-less sampling port |
Wilson & Coates (1996) found that using an alcohol-impregnated wipe did not destroy bacteria. Its use is questionable, but recommended at this time. Pratt et al (2007) state that an aseptic technique must be used when obtaining a CSU.
PROCEDURE: catheter specimen of urine
• Gain informed consent and gather equipment:
○ sterile specimen pot (correct one for the nature of the test required)
○ sterile gloves
○ 20 mL sterile syringe (and 25 g orange needle if it is a resealing port, with portable sharps box)
○ alcohol-impregnated swab
○ gate clamp.
• Ensure privacy.
• Examine the tubing for fresh urine; if none present apply the gate clamp below the level of the port and wait a few minutes for urine to collect.
• Wash hands and apply gloves.
• Wipe the port (both sorts) with the swab for 30 seconds (Wilson 1998) and allow to dry for 30 seconds (Steggall 2007).
• Resealing port: insert the needle into the rubber port taking care not to pierce out through the other side.
• Needle-less port: insert the syringe firmly into the port.
• Both: withdraw the required amount of urine (10–20 mL usually).
• Resealing: discard the needle (non-touch technique) using the sharps box.
• Place urine carefully into the specimen pot. Wipe the port for 30 seconds with the swab. Dispose of syringe correctly.
• Remove the clamp.
• Remove gloves and wash hands.
• Label the specimen correctly and dispatch to the laboratory, often within 1 hour; this will depend on the nature of the test (if delayed, refrigeration is sometimes acceptable).
• Document the findings and act accordingly.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


