Principles of cardiopulmonary resuscitation
Maternal resuscitation
Learning outcomes
Having read this chapter, the reader should be able to:
This chapter focuses on maternal resuscitation and basic life support techniques. While maternal collapse is a rare event, associated with increased morbidity and mortality for the woman and her baby, the frequency of cardiac arrest in pregnancy is increasing (Vanden Hoek et al 2010). McDonnell (2009) suggests that cardiac arrest has an incidence of 1 : 30,000 during pregnancy. However the Royal College of Obstetricians and Gynaecologists (RCOG) suggest the true rate of maternal collapse lies somewhere between 0.14 and 6 per 1000 births (RCOG 2011). The midwife rarely undertakes cardiopulmonary resuscitation (CPR); thus it is vital the midwife undertakes regular training and practice to ensure she can do this effectively and efficiently when the need arises and can modify the CPR to accommodate the particular needs of the collapsed pregnant woman. There are two ‘patients’ involved in the resuscitation of a pregnant woman and the best chance for the baby to survive is afforded by maternal survival (Vanden Hoek et al 2010).
Cardiac arrest occurs when the heart stops contracting effectively, e.g. ventricular fibrillation, or at all (asystole). As a result, breathing will stop, although agonal breathing may be seen before cessation of respiration. Travers et al (2010) suggest that there is a substantially better outcome when cardiac arrest is due to ineffective contraction of the heart rather than no contraction.
The Chain of Survival refers to the coordinated set of actions linking the victim of a sudden cardiac arrest with survival. These are specifically:
When CPR is undertaken immediately, the likelihood of survival for someone with an out-of-hospital cardiac arrest can double or triple (Cha et al 2013, Chalkias et al 2013, Iwami et al 2012). Where cardiac compressions and defibrillation occur within 3–5 minutes of collapse, survival rates are 49–75% (Nolan et al 2010). Each minute that CPR is delayed, the likelihood of survival can decrease by approximately 10% (Yang et al 2014) and for each minute defibrillation is delayed the chances of surviving to discharge from hospital are reduced by 10–12% (Nolan et al 2010). Dellimore & Scheffer (2012) suggest post-CPR survival rates can be extremely low which they partly attribute to the poor quality of compressions – depth, rate and length.
Anticipation of collapse
The majority of pregnant women are healthy and at low risk of cardiac arrest but there is the potential for complications from childbearing which may be life threatening. It may be possible to anticipate collapse and be proactive to prevent it occurring. These include:
When a woman is unwell it is important she is observed and managed appropriately so that any deterioration in her condition is recognized early and treated promptly. The use of the modified early obstetric scoring chart will assist with this (p. 66) (RCOG 2011).
Equipment
In the hospital environment, resuscitation equipment should be readily available and is usually kept together in a resuscitation trolley that can be taken to the place where resuscitation is occurring. The trolley will be standardized across the hospital, with equipment always in the same place to make it easier for the resuscitation team to access what they need quickly. It is therefore important that equipment is not added, removed or rearranged. Midwives attending homebirths usually have equipment available for providing oxygen and ventilation breaths; the paramedic crew will bring other equipment as needed, e.g. defibrillator. Equipment and drugs should be checked regularly to ensure they are working effectively and are in date.
The Resuscitation Council (UK) (2013a) have a list of equipment that should be immediately available (within first few minutes of cardiorespiratory arrest) or accessible (available for prompt use when the need is determined by the resuscitation team) within the acute care hospital setting.
Accessible
• 70% alcohol/2% chlorhexidine wipes
• Intravenous (I.V.) extension set and connectors, ports, and caps
• Blood gas analyzer and testing strips
• CPR arrest record forms for patient records, audit forms and do-not-attempt-CPR (DNACPR) forms
There should also be an emergency drug box which may contain drugs required for anaphylaxis management (p. 151):
Initial assessment
Collapse may be witnessed or unwitnessed. With an unwitnessed collapse, resuscitation may be less successful because of the delay in commencing cardiac compressions. The woman may be seen to look unwell, e.g. pale, cyanosed and clammy, and appear to be unmoving. It is important to ensure it is safe to approach the collapsed woman. A quick visual assessment of the area around the woman should be undertaken for hazards such as a wet floor or dangling wires. Personal safety should be considered if there is a lot of body fluids around or the woman is in isolation and personal protective equipment donned as necessary (p. 79).
Assessing responsiveness
The midwife should approach the woman from the side and assess her responsiveness by gently shaking her shoulders (unless a neck or back injury is suspected) and talking loudly to her. Asking her a question such as ‘Are you all right?’ will usually rouse the woman if she is not unconscious. Bearing in mind that the woman may be hard of hearing in one ear, the midwife should direct her talking to both ears.
Calling for help
If there is no response, help should be sought immediately. In a hospital setting this can be through use of the emergency buzzer or calling for help. It is important to call for the resuscitation team if the hospital has one, using the standard emergency number 2222 (National Patient Safety Agency 2004). The call should include the name of the ward/clinical area and specific location, e.g. first side room. If the ward is locked, a staff member should be positioned at the doors ready to let the team in as they arrive. The Resuscitation Council (UK) (2013b) advise the resuscitation team should be activated within 30 seconds of the call for help. In the community setting a paramedic team should be summoned using the 999 call. If the address is difficult to find, use a family member, if possible, to stand at the driveway to flag down the ambulance. The front door should be left unlocked to enable the paramedic team to enter quickly.
If there is no emergency buzzer or phone available to call for help, the midwife should send someone to call for help or if she is on her own, she will need to leave the woman, make the emergency call or ring the emergency buzzer and then return and continue with the resuscitation. CPR then continues using the ABCD approach – airway, breathing, circulation and defibrillation.
Airway
According to Madams (2008) the tongue is the main airway obstruction in collapsed or unconscious women during the intrapartum period. Opening the airway may be all that is needed to enable the woman to resume breathing. Ideally the woman should be turned onto her back and her airway opened using a head tilt and chin lift so her head is slightly extended and her tongue prevented from falling back and obstructing the airway. This is achieved by placing a hand on the woman’s forehead and gently tilting her head back, then using fingertips under her chin to tilt her chin upwards. Occasionally a jaw thrust is required to maintain the open airway during ventilation (Madams 2008) or when a cervical spine injury is suspected (Soar & Davies 2010). The jaw thrust is undertaken with both hands by placing two or three fingers under the mandible and one at the angle of the jaw to push and lift the jaw forwards. Pressure on the soft tissue should be avoided as this can cause oedema which can occlude the airway. Alternatively an oropharyngeal airway can be used if it becomes difficult to maintain an open airway.
An oropharyngeal airway has three parts: flange, body and tip. The flange is the piece that protrudes from the mouth and rests against the lips preventing the airway from moving further into the pharynx once it is inserted. The body is curved and follows the curve of the roof of the mouth, resting on top the tongue. The distal end is the tip that sits at the base of the tongue.
It is important to use the correct size of airway and this is assessed either by holding the flange of the airway against the side of the woman’s mouth, with the airway held horizontally so that the curved part of the airway curves around the woman’s jaw. It should end at the bottom of her earlobe. Alternatively the flange is placed against the mid-point of the woman’s lips (philtrum), with the airway finishing at the angle of the jaw (more difficult in obese people). Large adults generally require a size 5–6, medium adults size 4–5, and small adults size 3–4.
Prior to inserting the airway, tilt the woman’s head backwards and hold the airway with the curve up, i.e. the opposite way up to its final position within the oropharynx. This will allow the curved body to depress the tongue, preventing it from being pushed backwards. The airway is inserted following the curve of the woman’s airway. As it reaches the junction of the hard and soft palates, the airway should be rotated 180° into the correct position, with the curve down, while continuing to move it further into the mouth. When the airway is lying in the oropharynx, the flange should sit between the woman’s teeth. The tilted, neutral head position should be maintained and chin support given as required. It is important to assess the position of the airway intermittently to ensure it has not dislodged.
Any debris seen in the mouth should be removed with a wide-bore suction catheter. It is not advisable to undertake a finger sweep as the woman may bite the fingers and there is a small risk of cross-infection from body fluids. Loose dentures should be replaced in the mouth, as they help to maintain the shape of the jaw and chin tilt/jaw thrust. If the dentures are poorly fitting and keep coming loose, they may need to be removed.
Breathing
No more than 10 seconds should be taken to assess if the woman is breathing. The midwife will do this by bringing her head close to the woman’s face and chest and looking for chest rise, listening for breath sounds and feeling for breath on her cheeks. When no breathing is noted, cardiac arrest is assumed as the cause and CPR commenced immediately. Abnormal breathing should be noted as agonal breathing/gasping is present during the first minute after a sudden cardiac arrest in 40% of cases (Koster et al 2010) and so should not prevent initiation of cardiac compressions (Sayre et al 2010). If the woman is not breathing, there is no need to determine whether a pulse is present, as this is often unreliable (Travers et al 2010).
‘Rescue breaths’ are not given before the commencement of cardiac compressions, as this will delay the initiation of compressions further and it is vitally important that compressions begin as soon as possible. If the cardiac arrest is non-asphyxial in nature, there will be a high oxygen content in the blood initially, rendering ventilation less important than compressions (Handley & Colquhoun 2010).
Circulation
Cardiac compressions increase the chance of survival by maintaining the blood supply to the heart and brain (Travers et al 2010). This is achieved only if there is adequate perfusion of the coronary arteries to oxygenate the myocardium and of the brain for a neurologically intact survival (Cunningham et al 2012). With each compression, coronary perfusion pressure gradually increases, and Cunningham et al (2012) suggest it takes 40–45 seconds of continuous compressions to achieve the optimal perfusion pressure. Each time compressions are interrupted there is a rapid decrease in aortic relaxation (diastolic) pressure which reduces both coronary and cerebral perfusion pressures; thus it is important to minimize interruptions to cardiac compressions (Beesems et al 2013).
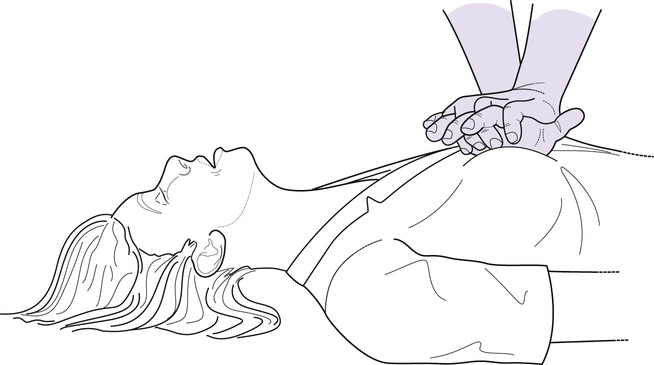
Cardiac compressions are undertaken by placing the heel of one hand in the centre of the chest, which positions the hand onto the lower half of the sternum (Sayre et al 2010). The heel of the second hand is placed on top of the first hand with the fingers interlocking to avoid pressure on the ribs (Koster et al 2010) (Fig. 55.1). Cha et al (2013) found cardiac output was increased when using manikins when the compressions were undertaken on the internipple line as opposed to the lower half of the sternum. However, Sayre et al (2010) suggest the use of the internipple line as a landmark is unreliable and this would be particularly so for women, as the position of their nipples vary according to the size of their breasts.