Chapter 2 T. Heather Herdman, RN, PhD, FNI and Shigemi Kamitsuru, RN, PhD, FNI Assessment is the first and the most critical step in the nursing process. If this step is not handled well, nurses will lose control over the subsequent steps of the nursing process. Without proper nursing assessment, there can be no nursing diagnosis, and without nursing diagnosis, there can be no independent nursing interventions. Assessment should not be performed merely to fill in the blank spaces on a form or computer screen. If this rings a bell for you, it’s time to take a new look at the purpose of assessment! During the assessment and diagnosis steps of the nursing process, nurses collect data from a patient (or family/group/community), process that data into information, and then organize that information into meaningful categories of knowledge, also known as nursing diagnoses. Assessment provides the best opportunity for nurses to establish an effective therapeutic relationship with the patient. In other words, assessment is both an intellectual and an interpersonal activity. As you can see in Figure 2.1, assessment involves multiple steps, with the goal being to diagnose and prioritize these diagnoses, which then become the basis for nursing treatment. Now, this probably sounds like a long, involved process and, frankly, who has time for all of that? In the real world, however, some of these steps happen in the blink of an eye. For instance, if a nurse sees a patient who is holding her lower abdomen and grimacing, he might immediately suspect that the patient is experiencing acute pain (00132). Thus, the movement from data collection (observation of the patient’s behavior) to determining potential diagnoses (e.g., acute pain) occurs in a split second. However, this quickly determined diagnosis might not be the right one – or it may not be the highest priority for your patient. Getting there does take time. Figure 2.1 Steps in Moving from Assessment to Diagnosis So, how do you accurately diagnose? Only by continuing to the further step of in-depth assessment – and the proper use of the data collected during that assessment – can you ensure accuracy in diagnosis. The patient may indeed be experiencing acute pain, but without in-depth assessment, there is no way for the nurse to know that the pain is related to intestinal cramping and diarrhea. This chapter provides foundational knowledge for what to do with all of that data you have collected. After all, why bother collecting it if you aren’t going to use it? In the next section, we will go through each of the steps in the process that takes us from assessment to diagnosis. But first, let’s spend a few minutes discussing the purpose – because assessment is not simply a task that nurses complete, we need to really understand its purpose so we can understand how it applies to our professional role as nurses. Nurses need to assess patients from the viewpoint of the nursing discipline to diagnose accurately and to provide effective care. What is the “nursing discipline”? Simply put, it is the body of knowledge that comprises the science of nursing. Diagnosing a patient based on his/her medical diagnosis or medical information is neither a recommended nor a safe diagnostic process. Such an overly simplified conclusion could lead to inappropriate interventions, prolonged length of stay, and unnecessary readmissions. Remember that nurses diagnose actual or potential human responses to health conditions/life processes, or a vulnerability for that response – the focus here is “human responses.” Human beings are complicated – we just don’t all respond to one situation in the same way. Those responses are based on many factors: genetics, physiology, health condition, and past experience with illness/injury. However, they are also influenced by the patient’s culture, ethnicity, religion/spiritual beliefs, gender, and family upbringing. This means that human responses are not so easily identified. If we simply assume that every patient with a particular medical diagnosis will respond in a certain way, we may treat conditions (and therefore use the nurse’s time and other resources) that do not exist while missing others that truly need our attention. It is possible that there may be close relationships between some nursing diagnoses and medical conditions; however, to date we do not have sufficient scientific evidence to definitively link all nursing diagnoses to particular medical diagnoses. For instance, there is no way to identify the patient’s ability for independent daily living or the availability/quality of family support, based on a medical diagnosis of myocardial infarction or osteoporosis. Nor can one assume that every patient with a medical diagnosis will respond in the same way: every patient who has experienced a mastectomy does not experience disturbed body image (00118), for example. Therefore, nursing assessment and diagnosis should be driven from the viewpoint of the nursing discipline. Unfortunately, in your practice, you will probably observe nurses who assign or “pick” a diagnosis before they have assessed the patient. What is wrong with this pathway to diagnosis? As an example, a nurse may begin to complete a plan of care based on the nursing diagnosis of anxiety (00146) for a patient undergoing surgery, before the patient has even arrived on the unit or been evaluated. Nurses working in surgical units encounter many preoperative patients, and those patients are often very anxious. Those nurses may know that preoperative teaching is an effective intervention in reducing anxiety. So, assuming a relationship between preoperative patients and anxiety could be useful in practice. However, the statement “preoperative patients have anxiety” may not apply to every patient (it is a hypothesis), and so it must be validated with each and every patient. This is especially true because anxiety is a subjective experience – although we may think the patient seems anxious, or we may expect him to be anxious, only he can really tell us if he feels anxious. In other words, the nurse can understand how the patient feels only if the patient tells the nurse about his feelings, so anxiety is a problem-focused nursing diagnosis which requires subjective data from the patient. What appears to be anxiety may actually be fear (00148) or ineffective coping (00069); we simply cannot know until we assess and validate our findings. Thus, before nurses diagnose a patient, a thorough assessment is absolutely necessary. There are two types of assessment: screening and in-depth assessment. While both require data collection, they serve different purposes. The screening assessment is the initial data collection step, and is probably the easiest to complete. The in-depth assessment is more focused, enabling the nurse to explore information that was identified in the initial screening assessment, and to search for additional cues that might support or refute potential nursing diagnoses. Most schools and healthcare organizations provide nurses with a standardized form – on paper or in the electronic health record – that must be completed for each patient within a specified period of time. For example, patients who are admitted to the hospital may need to have this assessment completed within 24 hours of admission. Patients seen in an ambulatory clinic may have a required assessment prior to being seen by the primary care provider (a physician or nurse practitioner, for example). Some organizations will have tools that enable completion of an assessment based on a particular nursing theory or model (e.g., Roy Adaptation Model), body system review, or some other method of organizing the data to be collected. The performance of the screening assessment requires specific competences for the accurate completion of various procedures to obtain data, and it requires a high level of skill in interpersonal communication. Patients must feel safe and trust the nurse before they will feel comfortable answering personal questions or providing answers, especially if they feel that their responses might not be “normal” or “accepted.” We say that the initial screening assessment may be the easiest step because, in some ways, it is initially a process of “filling in the blanks.” The form requires the patient’s temperature, so the nurse takes the temperature and inputs that data into the assessment form. The form requires that information is collected about the patient’s cardiac system, and the nurse completes all of the blank spaces on the form that deal with this system (heart rate, rhythm, presence of a murmur, pedal pulses, etc.). However, appropriate nursing assessment requires far more than this initial screening. Obviously, when the nurse reviews data collected during her assessment, and starts to recognize potential diagnoses, she will need to collect further data that can help her determine if there are other human responses occurring that are of concern, that indicate risks for the patient, or that suggest health promotion opportunities. The nurse will also want to identify the etiology or precipitating factors of areas of concern. It is quite possible that these in-depth questions are not included in the organization’s assessment form, because there is simply no way to include every possible question that might need to be asked for every possible human response! Let’s take a moment to consider the type of framework that supports a thorough nursing assessment. An evidence-based assessment framework should be used for accurate nursing diagnosis as well as safe patient care. It should also represent the discipline of the professional using it: in this case, the assessment form should represent knowledge from the nursing discipline. There is sometimes confusion over the difference between the NANDA-I Taxonomy II of nursing diagnoses and Gordon’s Functional Health Patterns (FHP) assessment framework (1994). The NANDA-I taxonomy was developed based on Gordon’s work; that is why the two frameworks look similar. However, their purposes and functions are entirely different. (See Chapters 3 and 4 for more specific information on the NANDA-I taxonomy.) The NANDA-I Taxonomy serves its intended purpose of sorting/categorizing nursing diagnoses. Each domain and class is defined, so the framework helps nurses to locate a nursing diagnosis within the taxonomy. On the other hand, the FHP framework was scientifically developed to standardize the structure for nursing assessment (Gordon, 1994). It guides the history-taking and physical examination by nurses, providing items to assess and a structure for organizing assessment data. In addition, the sequence of 11 patterns provides an efficient and effective flow for the nursing assessment. As stated in the NANDA-I Position Statement (2010), use of an evidence-based assessment framework, such as Gordon’s FHP, is highly recommended for accurate nursing diagnosis and safe patient care. It is not intended that the NANDA-I Taxonomy should be used as an assessment framework. The second step in the process is the conversion of data to information. Its purpose is to help us to consider what the data we collected in the screening assessment might mean, or to help us identify additional data that need to be collected. The terms “information” and “data” are sometimes used interchangeably, but the actual characteristics of data and information are quite different. In order to have a better understanding of assessment and nursing diagnosis, it is useful to take a moment to differentiate data from information. Data are the raw facts collected by nurses through their observations. Nurses collect data from a patient (or family/group/community) and then, using their nursing knowledge, they transform those data into information. Information can be seen as data with an assigned judgment or meaning, such as “high” or “low,” “normal” or “abnormal,” and “important” or “unimportant.” Figure 2.2 provides an example of how objective and subjective data can be converted to information through the application of nursing knowledge. Figure 2.2 Converting Data to Information: The Case of Caroline, a 14-year-old Female Seen in Ambulatory Clinic It is important to note that the same data can be interpreted differently depending on the context, or the gathering of new data. For example, let’s suppose that a nurse checks the body temperature of Mr. W who was just admitted to the hospital with an infected surgical wound and difficulty breathing. The thermometer indicates his temperature is 37.5 °C/99.5 °F, via the axillary route. This plain fact is given meaning by comparing it to accepted normal values, as the nurse processes data into information: Mr. W has a slight fever. However, what if the nurse learns that when Mr. W was seen in the ambulatory clinic two hours ago, his temperature was 39.0 °C/102.2 °F? With this new piece of data, the current temperature data can be reinterpreted: Mr. W’s temperature has decreased (it is improving). When documenting assessment, therefore, it is important to include both data and information. Information cannot be validated by others if original data are not provided. For example, simply indicating “Mr. W had a fever” is not clinically useful. How severe was the fever? How were data gathered (oral, axillary, core temperature)? Documentation that shows that Mr. W had a fever of 37.5 °C/ 99.5 °F, via the axillary method, enables another nurse to compare new temperature readings against the previous ones, and to identify if the patient is improving. Nurses collect and document two types of data related to a patient: subjective and objective data. While physicians value objective over subjective data for medical diagnoses, nurses value both types of data for nursing diagnoses (Gordon, 2008). What is the difference between subjective and objective data? The dictionary (Merriam-Webster, 2014) defines subjective as “based on feelings or opinions rather than facts”; objective means “based on facts rather than feelings or opinions.” One thing you should be careful of here is that when these terms are used in the context of nursing assessment, they have a slightly different meaning from this general dictionary definition. Although the basic idea remains the same, “subjective” does not mean the nurse’s feelings or opinions, but that of the subject of nursing care: the patient/family/group/community. Moreover, “objective” signifies those facts observed by the nurse or other healthcare professionals. In other words, the subjective data come from verbal reports from the patient regarding perceptions and thoughts on his/her health, daily life, comfort, relationships, and so on. For instance, a patient may report “I have had severe back pain for a week,” or “I don’t have anyone in my life with whom I can share my feelings.” Sometimes, however, the patient is unable to provide subjective data, and so we must rely on other sources, such as family members/close friends. Parents may provide useful information about their child’s behavior based on their daily observations and knowledge. An example might be a parent telling the nurse that “She usually curls up in a ball and rocks herself when she hurts.” Nurses can use this information to validate the baby’s behavior, and such behavior can be used as subjective data. Nurses collect these subjective data through the process of history-taking or interview. History-taking is not merely asking the patient one question after another using a routine format. In order to obtain accurate data from a patient, nurses must incorporate active listening skills, and use open-ended questions as much as possible, especially as follow-up questions when potentially abnormal data are identified. The objective data are those things that nurses observe about the patient. Objective data are collected through physical examinations and diagnostic test results. Here, “to observe” does not only mean the use of eyesight: it requires the use of all senses. For example, nurses look at the patient’s general appearance, listen to his lung sounds, they may smell foul wound drainage, and feel the skin temperature using touch. Additionally, nurses use various instruments and tools with the patient to collect numerical data (e.g., body weight, blood pressure, oxygen saturation, pain level). In order to obtain reliable and accurate objective data, nurses must have appropriate knowledge and skills to perform physical assessment and to use standardized tools or monitoring devices.
From Assessment to Diagnosis
What Happens during Nursing Assessment?
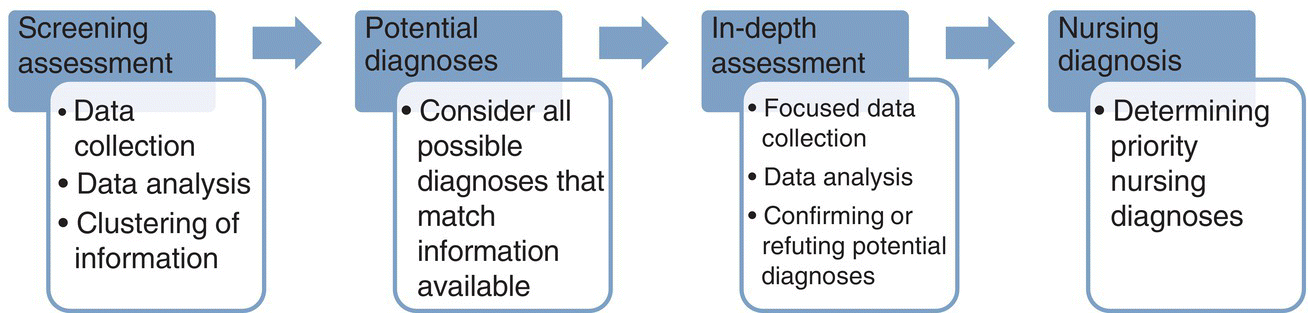
Why Do Nurses Assess?
The Screening Assessment
Not a Simple Matter of “Filling in the Blanks”
Assessment Framework
Should we use the NANDA-I taxonomy as an assessment framework?
Data Analysis
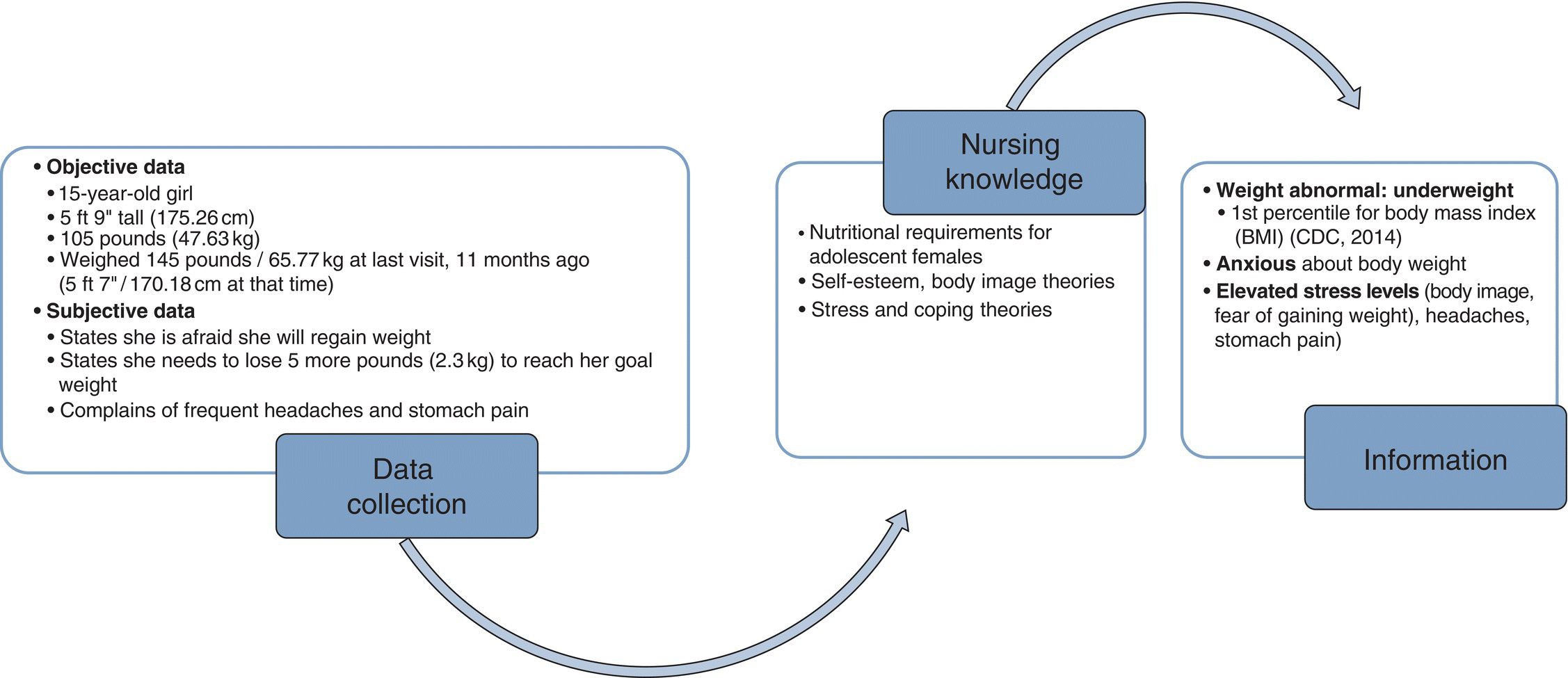
Subjective versus Objective Data
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


