Chapter 48 EMERGENCY CARE
RECOGNISING AN EMERGENCY
An emergency is a situation requiring immediate action. Recognising an emergency is the first step in responding. You may become aware of an emergency because of certain things you observe (Australian Red Cross 1998), such as unusual noises, sights, smells, signs or behaviours.
UNUSUAL NOISES
RESPONDING TO AN EMERGENCY
In an emergency situation your involvement as a nurse may be critical, as staffing levels are frequently at a minimum and all personnel are called on to give assistance. In a health care environment, strict emergency protocol is laid out and should be firmly adhered to. When working as a nurse it is part of your responsibility to ensure that you are familiar with each facility’s protocol. All the relevant information will be located in the facility’s policy and procedure manuals, commonly located at the nurse’s station, or electronically on the facility’s intranet site.
BARRIERS TO ACTION
See Clinical Interest Box 48.1. However, the worst thing to do is nothing!
PRIORITIES OF ACTION IN AN EMERGENCY
The following four emergency action principles (Australian Red Cross 1998) should guide the nurse’s actions in an emergency:
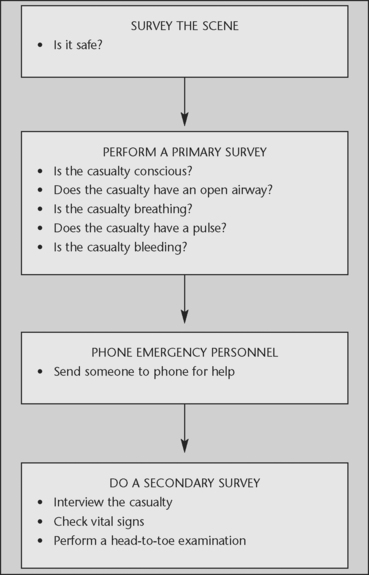
Implementing these principles (Figure 48.1) provides safety for you and for others and ensures that critical care is given to those who need it.
Survey the scene
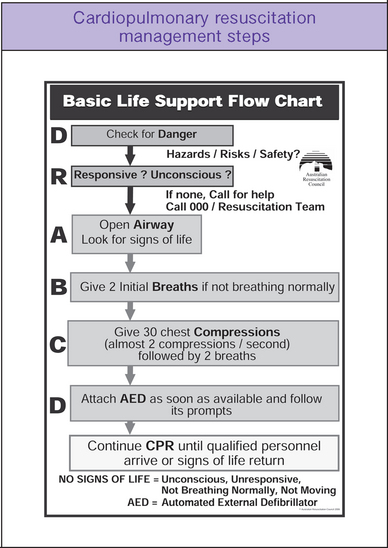
When it becomes apparent that an emergency has occurred and you decide to respond, you must ensure that the scene is safe for you and for others. Take the time to look at the scene and observe for anything that may pose a threat to your safety and that of the casualty or other bystanders. If any dangers are evident, do not approach the scene — call emergency personnel immediately for help. If you decide that the area is safe, then proceed to perform the primary survey. Figure 48.2 shows the basic life support flow chart that should be followed when attending all emergencies.
Primary survey
In every emergency situation you must first look for conditions that are an immediate threat to the casualty’s life. These are briefly mentioned here and will be discussed in more detail under ‘Resuscitation’. Clinical Interest Box 48.2 lists some definitions the first aider must be familiar with. In the primary survey, check for:
CLINICAL INTEREST BOX 48.2 Definitions to know
| BLS | basic life support |
| RB | rescue breathing |
| ECC | external cardiac compression |
| CPR | cardiopulmonary resuscitation |
| D | danger |
| R | response |
| A | airway |
| B | breathing |
| C | compression |
| D | defibrillation (if available) |
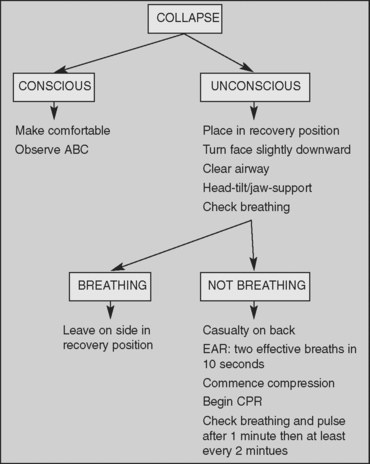
RESUSCITATION
Resuscitation is the preservation of life by establishment and/or maintenance of airway, breathing and circulation. The objective of resuscitation techniques is to ensure adequate supply of oxygen to the brain, not only to preserve life but also to prevent the damage to brain cells that results from lack of oxygen (Australian Red Cross 1998). Clinical Interest Box 48.3 presents more detail on resuscitation.
CLINICAL INTEREST BOX 48.3 Resuscitation
The central focus of resuscitation is the protection of the brain and heart from ischaemia, and the steps involved in resuscitation are systematic and implemented in order of priority. The principles of basic life support (BLS) include: (i) establishing and maintaining an airway; (ii) breathing; and (iii) circulation — the objective being to provide the brain and heart with an oxygenated blood supply. If a defibrillator is available, defibrillation is performed by attaching an AED (Automated External Defibrillator), and following the prompts (Australian Resuscitation Council [ARC] 2006).
Airway management
The steps involved in airway management include:
Recognition of airway obstruction
If the airway is partially or completely occluded, attempts to breathe result in:
Compression
As the pulse check is no longer used to identify the need for chest compressions, CPR — rescue breathing and chest compressions — is given to all victims requiring resuscitation, that is, victims not displaying signs of life (ARC 2006):
Position yourself vertically above the casualty’s chest, and with straight arms, press down on the sternum (St John Ambulance 2007).
Ratio of compressions to inflations
CPR is continued until the casualty shows signs of life (breathing, moving or responding), or until appropriate assistance arrives (ARC 2006).
Breathing
Compression
RESCUE BREATHING
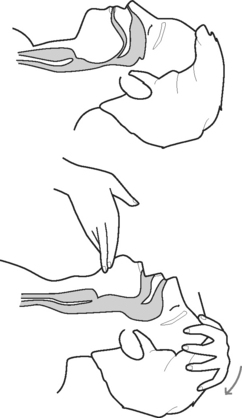
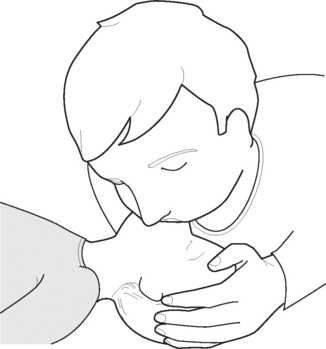
Figures 48.3, 48.4, 48.5 and 48.6 show the correct technique for ensuring effective rescue breathing.
Rescue breathing can be given:
EXTERNAL CARDIAC COMPRESSIONS
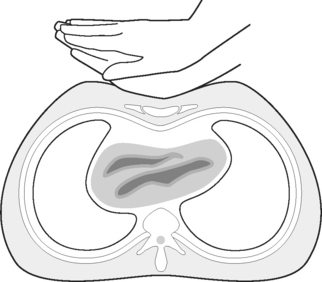
When the heart stops beating, circulation of the blood stops. Performing external cardiac compressions (ECC) provides an artificial pumping mechanism, which when carried out effectively, distributes blood around the body. Figures 48.7 and 48.8 show the correct location of ECC on an adult and child. ECC provides an artificial blood circulation by exerting rhythmic pressure at regular intervals (Figure 48.9) compressing the heart between the sternum and the spinal column.
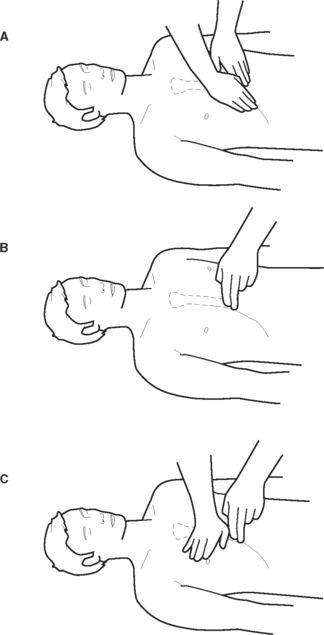
Figure 48.7 Location of ECC point in an adult. Proper hand position for CPR
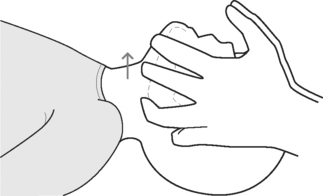
B: Moving fingers along the rib cage to the notch
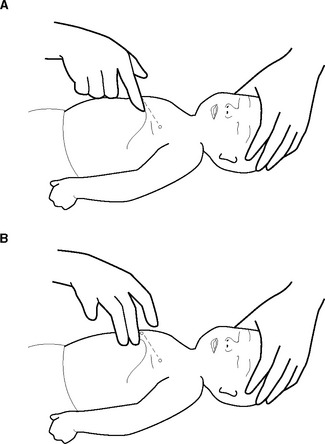
Figure 48.8 Location of ECC point in a child. Locating hand position for infant chest compressions
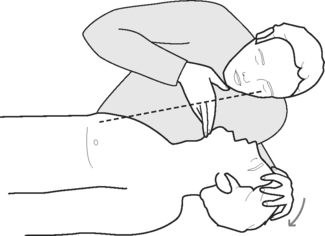
A: Drawing an imaginary line between the nipples
B: Placing 2 fingers on the sternum about 1 finger-width below the imaginary line
PRINCIPLES OF EMERGENCY CARE
Every emergency situation must be assessed, and appropriate measures taken in the sequence most logical for that particular situation. A variety of factors influences the actions taken and the order in which they are taken; for example, the presence of life-threatening circumstances, the availability of assistance, the location where the emergency occurs and the availability of transport. Clinical Interest Box 48.4 outlines the emergency response steps. The general principles of emergency care are:
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree