Value is the intersection of cost and quality in health care.
After completing this chapter, you should be able to:
• Define economics and health care economics.
• Compare the market for health care to a normal market for goods and services.
• Use a basic knowledge of health care economics to analyze trends in the health care delivery system.
• Describe what operating budget, personnel budget, and capital budget mean.
• Define economic research strategies.
• Describe what is meant by the term fiscal responsibility in clinical practice.
• Discuss strategies you will use to achieve fiscal responsibility in your clinical practice.
The rate of increase in U.S. national health care spending for 2013 was 3.6%, continuing a pattern of low growth following the economic recession for five consecutive years from 2009 to 2013 (Hartman et al., 2015). U.S. National health expenditures (NHE) in 2013 were $2.9 trillion, or $9255 per person, which comprises 17.4% of the gross domestic product (GDP) (Hartman et al., 2015). By the year 2024, those expenditures are projected to be $5.4 trillion and comprise 19.6% of GDP (Keehan et al., 2015).
The outcome of this large investment of resources in health and health care in the United States is variable. Many Americans do not receive the care they need, receive care that causes harm, or receive care without consideration of their preferences and values. The distribution of services is often inefficient and uneven across populations. Since 1999, annual reports by the Agency for Healthcare Research and Quality (AHRQ) have summarized the performance of the U.S. health care system and identified strengths and weaknesses (AHRQ, 2015). The specific goals are to achieve better care, smarter spending, and healthier people. The most recent report for 2014 indicates that access has improved and quality has improved for many priorities including patient safety, person-centered care, effective treatment measures for some conditions, and healthy living (AHRQ, 2015). However, many challenges remain in improving quality and reducing racial, ethnic, and income disparities (AHRQ, 2015). All of these clinical and financial measures of the health care system have implications for nursing practice.
What are the Trends Affecting the Rising Costs of Health Care?
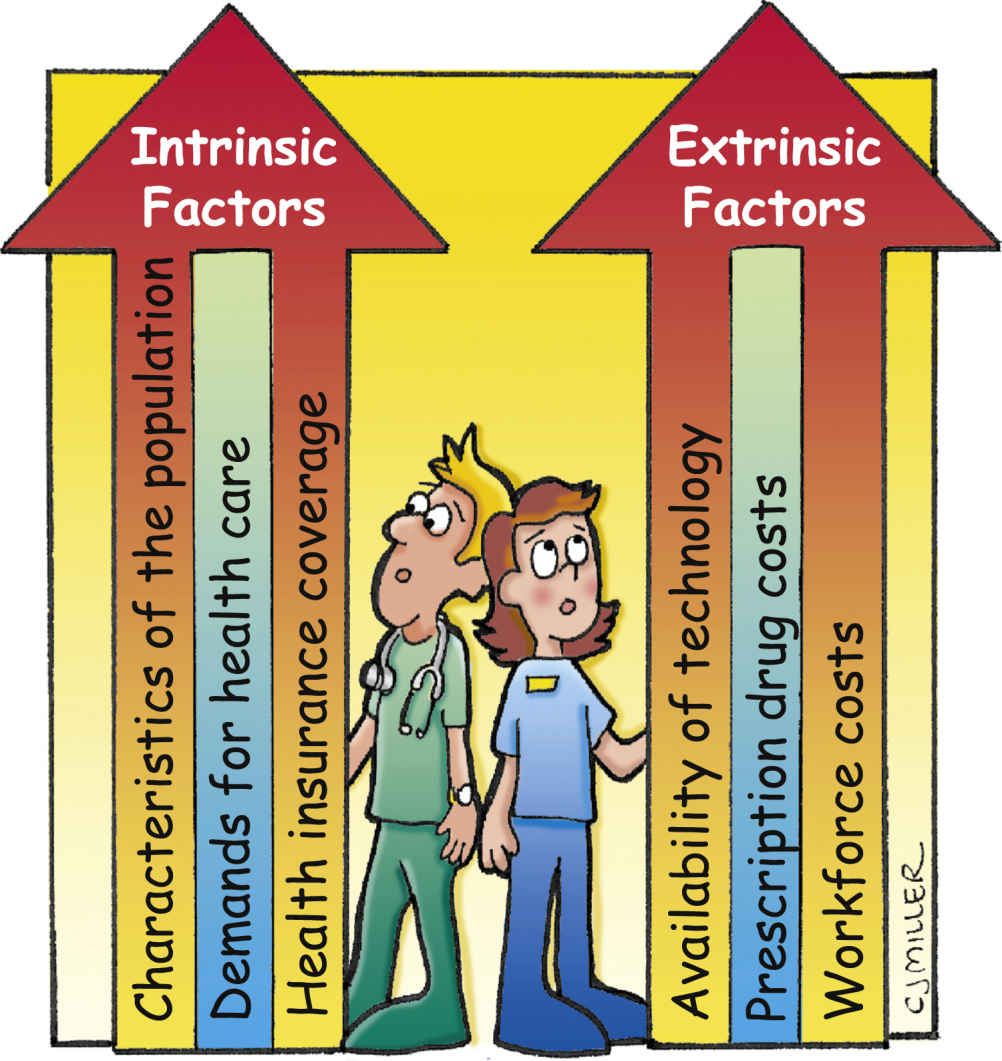
Both intrinsic and extrinsic factors contribute to the rising costs of health care. Intrinsic factors include characteristics of the population (the population is getting older and is requiring more of the health care system), the demand for health care, and health insurance coverage. Extrinsic factors include the availability of technology, prescription drug costs, and workforce costs (Fig. 16.1). The effects of the economic recession between 2008 and 2010 were high levels of unemployment, a decrease in private health insurance enrollment, an increase in Medicaid enrollment, and an increase in the number of uninsured people (Hartman et al., 2015). Economic trends, such as a recession, have both intrinsic and extrinsic effects.
Intrinsic Factors
The 2010 Census reported that there are 308.7 million people in the United States, a 9.7% increase from the 2000 Census (U.S. Census Bureau, 2011). Population projections based on the 2010 Census for the years 2012 to 2060 predict much slower growth during the next several decades and increased diversity in the U.S. population (U.S. Census Bureau, 2012). According to projections for 2012 to 2060, the population over age 65 is expected to more than double, and the population of the “oldest old,” over age 85, is expected to more than triple (U.S. Census Bureau, 2012). This is important information, because older people typically use increased health care resources and may not have the income to purchase them. During the projection period of 2009 to 2019, the Baby Boomers (citizens born between 1946 and 1964) will become eligible for Medicare health insurance. A critical challenge for the Medicare program will be to provide quality care for the increasingly aging population while keeping the program financially secure. The Affordable Care Act (ACA) of 2010 included reductions in Medicare payments to plans and providers and introduced system reforms including accountable care organizations (ACOs), medical homes, bundled payments, and value-based purchasing to improve quality and reduce costs (Kaiser Family Foundation Fact Sheet, 2015c). Medicare spending growth has slowed recently, averaging 4.1% between 2010 and 2014, compared to 9.0% between 2000 and 2010 (Kaiser Family Foundation Fact Sheet, 2015b).
Demand, in the economic sense, is the amount of health care services that a consumer wishes to purchase. Demand for health care may be influenced by illness, cultural-demographic characteristics, and economic factors, including income and health insurance (Feldstein, 2012). Health insurance coverage is one of the most important factors that influences the quantity of health services demanded (Feldstein, 2012). In 2014, the number of uninsured people was estimated at 32 million, a decrease of nearly 9 million since 2013 (Kaiser Family Foundation Fact Sheet, 2015a). With the 2014 implementation of the ACA Medicaid expansion and Health Insurance Marketplaces, it was estimated that 8.4 million Americans gained insurance coverage (Keehan et al., 2015). One of the first groups to gain expanded health insurance options under the ACA was young adults, age 19 to 25, who were allowed to remain as dependents on their parent’s private insurance until age 26. The uninsured rate for these young adults dropped from over 30% in 2009 to 19% in 2014 (McMorrow et al., 2015).
Extrinsic Factors
The availability of new medical technology has contributed to the rising costs of health care. If an organization does not offer technology that a competitor offers, it is likely that the market share (percentage of persons in an area selecting that institution) of the organization will decline. To attain a competitive edge, an organization needs to be an early adopter of expensive, new technology. Then, thinking sequentially, someone has to pay for the technology, and this cost will be passed on to consumers in the form of higher health care costs.
After slower growth in 2012, prescription drug spending increased by 2.5% in 2013. Factors influencing the increased spending included higher prices for brand-name and specialty drugs, new medicines, and increased utilization (Hartman et al., 2015). Another factor driving health care costs is hospital care expenditures, which increased 4.3% in 2013, a slightly lower increase than the 5.7% increase in 2012 (Hartman et al., 2015). Individuals’ out-of-pocket spending for health care increased to 12% of NHE in 2013 due to higher cost sharing in group health insurance plans and increased enrollment in consumer-directed health plans with high deductibles and copayments (Hartman et al., 2015). The Organization for Economic Cooperation and Development (OECD) compared health data for 34 industrialized countries in 2013 (OECD, 2015). In 2013, health spending was 16.4% of GDP in the United States, which was well above the OECD average of 8.9% (OECD, 2015). The United States spent $8713 per capita (per person) on health care in 2013, which is also well above the OECD average health spending per capita in 2013 of $3453 (OECD, 2015). In 2013, the United States continued to be number one in health care spending as a percent of GDP and also in per capita spending; however, the United States had an infant mortality rate of 6.0 deaths per 1000 live births, which is above the OECD average of 4.1, and a life expectancy of 78.8 years, which is more than 1.7 years less than the OECD average of 80.5 years (OECD, 2015).
What is the Effect of the Changing Economic Environment on Clinical Practice?
Because nurses belong to the largest health care profession and are thus in a position to influence health care costs, it is essential that all nurses understand basic concepts of economics and fiscal (money) management. This knowledge was previously taught in graduate courses for nurse managers or nurse executives. However, the world has changed! Nurses at the point of care in all settings will be challenged to maintain caring values and practices in relationships with patients and families while maintaining financial responsibility within the economic reality of limited resources (Cara, Nyberg, & Brousseau, 2011).
Introduction to Economics
A simple definition of economics is the allocation of scarce resources. An analogy might be made to the income that an individual earns. The paycheck is a limited, finite amount of money, and choices must be made about how to spend, or allocate, the money. Such choices might include rent, a car payment, food, clothing, and health insurance payments. Individuals may not be able to pay for all of the goods or services that they wish to have, so decisions must be made and priorities established.
Similarly, health care is a limited resource, and choices have to be made. The choices about health care that concern economists are made at the national level. Questions include How much does the country wish to spend on health care, what services does the country wish to provide, what is the best method for producing health care, and how will health care be distributed (Feldstein, 2012)?
What Are the Choices About Amount of Spending?
Currently, the United States is spending between 17% and 18% of its income on health care. As the payer for Medicare (the national health insurance program for people aged 65 years or older, some people younger than age 65 with disabilities, and people with end-stage renal disease) and Medicaid (a joint federal and state program that pays for medical assistance for certain individuals and families with low incomes and resources), the federal government is the nation’s largest purchaser of health care. Yet this amount does not fully meet the needs of the populations served under these programs, let alone provide for the health care needs of persons without insurance.
The Affordable Care Act of 2010
The ACA of 2010 was the largest mandated health care change since Medicare and Medicaid were introduced in 1965. The timeline for implementing the ACA was from 2010 through 2015. The provisions of the law addressed issues of access, quality, and cost in the U.S. health care system (Critical Thinking Box 16.1).
The ACA created a framework for increasing access to health coverage for Americans. Key features of the Affordable Care Act include:
• Provides state and federal-based health insurance marketplaces where individuals can purchase private insurance with premium and cost-sharing assistance based on income level. Requires all health plans to provide a standardized, easy-to-read uniform Summary of Benefits and Coverage (SBC), which gives consumers consistent information and allows them to compare what health plans offer when making choices of coverage
• Prohibits denial of coverage for children with preexisting conditions beginning in 2010 and for adults with preexisting conditions beginning in 2014
• Allows young adults up to age 26 to stay on their parents’ insurance policies
• Provides expanded Medicaid coverage for low-income children and adults
• Provides coverage for a range of preventive health services without any patient cost-sharing (co-payments, deductibles, or co-insurance) (Kaiser Family Foundation Issue Brief, 2015c)
Four years after its implementation, the ACA remains controversial, although progress has been made to increase access and affordability of health coverage for many Americans. Challenges include that many uninsured remain unaware of the requirement to have coverage and the subsidies available to make it more affordable, some uninsured are still left out of the expanded coverage, and there is uncertainty about the funding for maintaining coverage expansions in the future (Kaiser Family Foundation Issue Brief, 2015c).
What Are the Choices Regarding the Services Provided?
The state of Oregon passed legislation between the years 1989 and 1995 that provides an example of choices about the services provided to persons with Medicaid coverage. Consumers and providers of health and social services were charged with developing a ranked list of health care services, in the order of their benefit to the entire population being served, and reflecting community values. Coverage for all conditions at a certain level would be set by the state legislature and would be dependent on budget constraints. In the listing of services, treatment of premature infants, cleft palate, hip fracture, or stroke was covered, for example, whereas radial keratotomy, cosmetic dentistry, and treatment of varicose veins was not included (Oregon Health Authority, 2012). Although this is one type of rationing of health care, and Americans are typically opposed to any type of rationing system, it must be noted that the services denied under the Oregon plan are consistent with those denied reimbursement under other private and public insurance plans.
As it is for physicians, rationing of care is an important issue facing the nursing profession. The International Hospital Outcomes Study reported on rationing of nursing care. Researchers in Switzerland (Schubert et al., 2008) explored the association between the implicit rationing of nursing care and patient outcomes in Swiss hospitals. They found that, despite low levels of rationing of nursing care, rationing was a significant predictor for the six patient outcomes that were studied.
What Are the Choices About Methods to Produce Health Care?
One informal definition of managed care is the right care, in the right amount, by the right provider, in the right setting. This definition implies that there are several ways to provide health care. For example, a woman may choose to have an annual physical examination by a nurse practitioner, a certified nurse-midwife, a gynecologist, or a family practice physician. Each provides care from a different perspective and at a different price. In another example, certain procedures that were once performed only in hospitals are now done in outpatient settings, many with the addition of home health nursing. Lumpectomy and simple mastectomies are surgical procedures that are now handled in an outpatient setting, illustrating a different method of providing health care. Deciding the best method is subject to research and must include an analysis of the costs.
What Are the Choices About Allocation?
These decisions involve “who gets what.” The underlying question is Is health care a right or a commodity (like cars or clothing) to be allocated by the marketplace? The World Health Organization (WHO) states in its constitution that the enjoyment of the highest attainable standard of health is one of the fundamental rights of every human being (WHO, 2005). The American Nurses Association Health System Reform Agenda (2008) also affirms that health care is a basic human right and that a health care system should ensure universal access to essential health care services. In another document, the ANA Code of Ethics for Nurses (2015) states that nurses should provide care without consideration of the patient’s social or economic status. However, even if one believes that health care is a right, challenging questions remain. How much health care is a right? Who pays for the health care of people who cannot afford it? Let us assume that an instructor is teaching senior nursing students who all agree that health care is a right. The instructor then asks the students how much of their paycheck they would be willing to forfeit in taxes so that everyone could have this right to receive health care. It is rare that students are willing to subsidize others’ health care at a cost of more than one third of their own salaries.
Even beyond the costs of care is the question of allocation decisions—that is, who decides who receives what health care. Several responses are possible: the government, payers of health care, individuals, the marketplace, or rationing systems.
Government Allocation Decisions
Through its funding of Medicare, the government has made multiple allocation decisions. The U.S. government has decided it will pay for inpatient health care and some outpatient care for patients older than 65 years of age and for selected others. Unfortunately, many of the persons covered by Medicare have come to believe that Medicare covers “everything,” and this is not so. It is particularly challenging to nurses when elderly patients assume that they “have Medicare” and thus “nursing home care is paid for.” This is a frequent misinterpretation of Medicare coverage. There are many limitations to the services reimbursed by Medicare and many requirements that must be met before the government will make payment (Critical Thinking Box 16.2).
Payer Allocation Decisions
The ACA of 2010 required all health plans to provide coverage for applicants regardless of health status, gender, or any other factors. In addition, the ACA requires plans to cover a range of preventive health services without any patient cost sharing (Kaiser Family Foundation, 2015c). Within these overall guidelines, all insurance companies have rules about the services that will be covered or not covered and the requirements that must be met under their policies.
Most policies require preauthorization (preapproval) of services before the patient receives care, except in cases of emergency. For example, a physician’s office will typically communicate the need for a surgical procedure to the insurance company and obtain this approval. If the patient is admitted to the hospital in an emergency, however, this requirement is normally waived, and the hospital has a limited amount of time to gain the payer approval or reimbursement for the care or the claim may be denied.
Another restriction on resource allocation involves the process of concurrent utilization review (UR). This is a strategy used by managed care companies to control both costs and quality. The process requires that hospital staff, typically registered nurses, communicate the plan of care for a hospitalized patient to the payer or their representative. The payer then determines whether the care is appropriate, is medically necessary, and is covered under the terms of the policy or the contract with the provider (Murray & Henriques, 2003). For example, if a patient is admitted to the hospital the day before elective surgery, that day’s cost will almost certainly be denied reimbursement. Preoperative patient teaching and surgical preparation can be handled on an outpatient basis at a much lower cost than a day in the hospital.
Marketplace Allocation Decisions
A final alternative for the allocation of resources is the marketplace. This type of decision making implies that health care is a normal good, similar to a car or a piece of clothing, where an increase in income leads to an increase in demand for the good, and the rules of supply and demand apply. However, the market for health care includes some significant differences when compared to the market for normal goods.
Unpredictability of demand
The first difference in the market for health care is the unpredictability of demand. When a person is well, there is little demand for health care services. There is a great demand for health care when a person is ill, and the timing of illness is, of course, uncertain. Consider, for example, the case of a patient needing a heart transplant. A patient does not wait until the price comes down. Rather, the surgery is purchased at any price if a donor heart is available.
Consumer knowledge
Another difference in the health care market involves the knowledge of the consumer. If an individual is purchasing a coat or a car, the person usually knows a good deal about the item being purchased, or he or she consults Consumer Reports for further data. This is not the case in health care, about which patients tend to have limited knowledge and limited ability to interpret the available knowledge.
Barriers to entry to the market
Lack of price competition
The health care market, unlike the market for clothing and automobiles, does not engage in price competition. When, for example, have you heard of a sale on appendectomies or “2 for the price of 1” hip replacements? Of course, it does not happen. But more problematic is the fact that health care consumers frequently do not know the cost of their care—especially if an insurance provider is paying for it. In fact, many consumers indicate that they “never saw a bill” for their hospitalization. This is considered to be a measure of the quality of their insurance. Is there any other product that would be routinely purchased without knowledge of its price? The lack of this knowledge leads to predictable consumer health care purchasing behavior.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree