CHAPTER 13 Care for Patients with Special Needs
Section One Providing Nutritional Support
 Nutritional Assessment
Nutritional Assessment
Dietary History
Signs and Symptoms/Physical Findings
Anthropometric Data
BMI
BMI values of 19-25 are appropriate for 19-34 yr olds, whereas BMI values of 21-27 are appropriate for individuals older than 35 yr of age. Obesity is defined as BMI greater than 27.5, with severe or morbid obesity greater than 40. A BMI of 16-18.5 is considered mild to moderate malnutrition, whereas a value lower than 16 indicates severe malnutrition.
Estimating Nutritional Requirements
Calorie estimation
Prevents overfeeding, and calculates the total calorie intake as follows:
| Average nourished patient | 25 total calories per kg of body weight |
| Mildly stressed patient | 30 total calories per kg of body weight |
| Severely stressed patient | 35 total calories per kg of body weight |
| Morbidly obese patient | 18 total calories per kg of body weight |
Distribution of calories
 Nutritional Support Modalities
Nutritional Support Modalities
Overview/Pathophysiology
Terms associated with formulas for oral supplements or enteral delivery
TABLE 13-1 DESCRIPTIVE TERMS ASSOCIATED WITH TYPES OF ENTERAL FORMULAS
| TERM | DEFINITION |
|---|---|
| Isotonic | Formula having an osmolarity of 300 mOsm/L, which is the same as blood |
| Osmotic gradient between the formula and the blood flow within the intestines is equal | |
| Hypertonic | Formula having an osmolarity greater than 300 mOsm/L, usually in the range of 450-600 mOsm/L; osmotic gradient between the formula and the blood flow within the intestines is unequal, and the formula will pull fluid into the intestines during the digestive process |
| Osmolarity | Referred to as mOsm/L and describes the osmotic gradient between blood and the intestines; normal level found in the blood is300 mOsm/L |
| Caloric density | Number of calories delivered to patient in each mL of liquid feeding |
| Ranges from 0.5-2 kcal/mL | |
| Modular | Consists of a single nutrient that may be combined with other modules (nutrients) to treat specific deficits (e.g., protein, carbohydrate, or fat) in an individual |
Nutritional composition
TABLE 13-2 NUTRITIONAL COMPOSITION OF ENTERAL FORMULAS AND ORAL SUPPLEMENTS
| COMPONENT | TYPE | DESCRIPTION |
|---|---|---|
| Protein | Polymeric | Standard, complete protein nitrogen source |
| Hydrolyzed | Reduced into smaller forms to assist with absorption | |
| Elemental/free amino acids | Simple amino acids that require no further digestion and are ready for absorption | |
| Usually increases formula osmolarity; bitter taste | ||
| Carbohydrate | The most easily digested and absorbed component in enteral formulas; 80% of all carbohydrate is broken down and absorbed as simple glucose in the normal intestine; most commercially available formulas are lactose free | |
| Fat | Long-chain triglycerides | Provide an isotonic, concentrated energy source |
| Medium-chain triglycerides | Used for patients with impaired fat digestion and absorption; no stimulation of pancreatic lipase secretion | |
| Omega-3 fatty acids | Addition of fish oils to improve immune function of the body by producing eicosapentaenoic acid | |
| Fiber | Soy polysaccharide is most commonly added to enteral formulas as a treatment for diarrhea, although its usefulness has not been proven with research; because fiber is absorbed in the large intestine, a patient with an ileostomy would not benefit; formula viscosity increases with fiber, and it should be delivered via an enteral tube 10F or larger with an enteral feeding pump |
Types of feeding tubes
Gastrostomy tubes
Exit stomach directly through abdominal wall and are usually anchored with either a balloon or a disk on the inside of the stomach. Generally they are 12F or larger. Composition may be polyurethane, silicone, or rubber, and these tubes may contain multiple ports for insertion of air into the balloon, delivery of medications, and the main lumen. Initially a physician in the radiology, endoscopy, or surgery department performs the insertion. When the tube is placed by a physician in the radiology or endoscopy department, the common term used to describe the tube is percutaneous endoscopic gastrostomy (PEG). Reinsertion by a nurse is determined by hospital policy.
Gastrostomy-jejunostomy tubes
BOX 13-1 presents nursing care guidelines for enteral tubes.
BOX 13-1 GENERAL NURSING CARE GUIDELINES FOR ENTERAL TUBES
 Best patency is maintained with regular flushing of the tube before and after each medication, before and after each intermittent feeding, and routinely during continuous feedings.
Best patency is maintained with regular flushing of the tube before and after each medication, before and after each intermittent feeding, and routinely during continuous feedings. Flush tube with water using 25-50 mL, depending on physician prescription and patient’s underlying medical condition. Dark cola also has been suggested as a potential agent for flushing tubes.
Flush tube with water using 25-50 mL, depending on physician prescription and patient’s underlying medical condition. Dark cola also has been suggested as a potential agent for flushing tubes. Because of impurities and bacteria in tap water, sterile water has been suggested for high-risk patients, including infants and older adults, and for any tube feeding that enters the body in the small intestine. (Check agency policy for type of water used to flush enteral feeding tubes in your patient population.)
Because of impurities and bacteria in tap water, sterile water has been suggested for high-risk patients, including infants and older adults, and for any tube feeding that enters the body in the small intestine. (Check agency policy for type of water used to flush enteral feeding tubes in your patient population.) If the enteral tube becomes clogged, it is best to identify whether the change in flow was related to formula buildup within the tube or a chemical reaction from medications being administered through the tube. If the tube is clogged with formula, products that have been suggested for declogging it are dark cola, hot water, and pancrease or other commercially available enzymatic medication pushed down the tube, using a push-pull method and correct syringe size recommended by the manufacturer. If the tube has become clogged with medications, hot water may be used via the aforementioned push-pull method. Mechanical devices are also available for declogging a tube, but use may be restricted to trained individuals within the institution. (Check with agency policy for type of declogging recommended in enteral feeding tubes.)
If the enteral tube becomes clogged, it is best to identify whether the change in flow was related to formula buildup within the tube or a chemical reaction from medications being administered through the tube. If the tube is clogged with formula, products that have been suggested for declogging it are dark cola, hot water, and pancrease or other commercially available enzymatic medication pushed down the tube, using a push-pull method and correct syringe size recommended by the manufacturer. If the tube has become clogged with medications, hot water may be used via the aforementioned push-pull method. Mechanical devices are also available for declogging a tube, but use may be restricted to trained individuals within the institution. (Check with agency policy for type of declogging recommended in enteral feeding tubes.) Always insert smallest-bore tube possible to minimize complications. A large-bore nasogastric tube may be used temporarily in the stomach until a small-bore tube can be placed; a small-bore tube must be inserted if intestinal placement is required for delivery of the formula.
Always insert smallest-bore tube possible to minimize complications. A large-bore nasogastric tube may be used temporarily in the stomach until a small-bore tube can be placed; a small-bore tube must be inserted if intestinal placement is required for delivery of the formula. When anchoring the tube in place, ensure adequate skin protection and observe for pressure on the skin.
When anchoring the tube in place, ensure adequate skin protection and observe for pressure on the skin. Nasal tubes may result in pressure on the nares if the tube is taped too tightly to the nose. (Check with agency policy for frequency of nasal assessment recommended for nasal enteral feeding tubes.)
Nasal tubes may result in pressure on the nares if the tube is taped too tightly to the nose. (Check with agency policy for frequency of nasal assessment recommended for nasal enteral feeding tubes.) Gastric tubes may result in an increase in reflux or damage to the stoma if the tube is angled and pulled flat against the abdominal wall. Some newer tubes are being designed with an angle to facilitate taping to the abdominal wall.
Gastric tubes may result in an increase in reflux or damage to the stoma if the tube is angled and pulled flat against the abdominal wall. Some newer tubes are being designed with an angle to facilitate taping to the abdominal wall. If bumpers are used with a gastric tube, check with manufacturer or agency policy to identify whether it is necessary to routinely rotate the bumper around the tube while inspecting the skin daily.
If bumpers are used with a gastric tube, check with manufacturer or agency policy to identify whether it is necessary to routinely rotate the bumper around the tube while inspecting the skin daily. If bumpers are used with a gastric tube, a dressing may not be necessary and may be avoided under the bumpers to prevent too much pulling on the tube. A dressing under a bumper may cause internal and external anchoring devices to become too tight and may thereby produce some vascular insufficiency to the abdominal wall.
If bumpers are used with a gastric tube, a dressing may not be necessary and may be avoided under the bumpers to prevent too much pulling on the tube. A dressing under a bumper may cause internal and external anchoring devices to become too tight and may thereby produce some vascular insufficiency to the abdominal wall. If inserting a small-bore feeding tube, always verify initial placement in the stomach or small intestine with x-ray film before initiating the feeding.
If inserting a small-bore feeding tube, always verify initial placement in the stomach or small intestine with x-ray film before initiating the feeding. Verify with pharmacy that medications are appropriate for administration via an enteral feeding tube. Change in route or delivery form may be necessary to maintain medication effects. For example:
Verify with pharmacy that medications are appropriate for administration via an enteral feeding tube. Change in route or delivery form may be necessary to maintain medication effects. For example: Time-released medications may have to be changed to a short-acting form because time-released medications should not be crushed.
Time-released medications may have to be changed to a short-acting form because time-released medications should not be crushed. A medication that is absorbed in the stomach may have to be reevaluated when the distal tip of the tube is in the small intestine.
A medication that is absorbed in the stomach may have to be reevaluated when the distal tip of the tube is in the small intestine.Feeding sites
Duodenum, jejunum
BOX 13-2 and TABLE 13-3 present guidelines for administration of enteral products.
BOX 13-2 GENERAL NURSING CARE GUIDELINES FOR ADMINISTRATION OF AN ENTERAL FORMULA
 If the individual has a history of glucose intolerance or is taking medications that may cause hyperglycemia, or if an increase in blood glucose is noted on serum electrolyte values, routine monitoring of the glucose should include bedside assessments q4h and treatment appropriate for maintaining glucose within normal limits.
If the individual has a history of glucose intolerance or is taking medications that may cause hyperglycemia, or if an increase in blood glucose is noted on serum electrolyte values, routine monitoring of the glucose should include bedside assessments q4h and treatment appropriate for maintaining glucose within normal limits. Monitor I&O q8h. Separate intake of formula from intake of other nutrients or fluids. Keep enteral tube flushing amounts separate from enteral formula intake.
Monitor I&O q8h. Separate intake of formula from intake of other nutrients or fluids. Keep enteral tube flushing amounts separate from enteral formula intake. If using an open delivery system, do not use formula that has been opened for more than 24 hr. If using a closed delivery system, refer to manufacturer or agency policy for duration of hang time.
If using an open delivery system, do not use formula that has been opened for more than 24 hr. If using a closed delivery system, refer to manufacturer or agency policy for duration of hang time. Several key points in the delivery of enteral formulas established by Hazard Analysis Critical Control Point (HACCP) developed by the U.S. Department of Agriculture (USDA) and the Food and Drug Administration (FDA) include the following:
Several key points in the delivery of enteral formulas established by Hazard Analysis Critical Control Point (HACCP) developed by the U.S. Department of Agriculture (USDA) and the Food and Drug Administration (FDA) include the following: Perform meticulous handwashing when handling all aspects of the products, including bag, formula, pump and additives.
Perform meticulous handwashing when handling all aspects of the products, including bag, formula, pump and additives. Only hang a volume of formula that will infuse within a designated timeframe. Mark bag indicating how long it should hang.
Only hang a volume of formula that will infuse within a designated timeframe. Mark bag indicating how long it should hang. If giving intermittent feedings, flush bag and set with water between feedings. Refer to agency policy for type of water to be used (sterile vs. tap).
If giving intermittent feedings, flush bag and set with water between feedings. Refer to agency policy for type of water to be used (sterile vs. tap).TABLE 13-3 ADMINISTRATION OF ENTERAL PRODUCTS
| TYPE | DEFINITION | COMPLICATIONS |
|---|---|---|
| Bolus | Given by gravity; pushed via syringe | May cause cramping, bloating, nausea, diarrhea, aspiration; not recommended |
| Intermittent | Administered over 30-60 min via infusion bag; total volume should not exceed 450 mL/feeding | May cause cramping, nausea, bloating, diarrhea, aspiration; may need to ↓ infusion rate to ↓ complications |
| Continuous | Given at the same infusion rate over 24 hr; may be cycled over 12-24 hr if patient tolerates the volume | May cause cramping, nausea, bloating, diarrhea, aspiration; may need to ↓ infusion rate to ↓ complications |
 Total Parenteral Nutrition
Total Parenteral Nutrition
Overview/Pathophysiology
Parenteral solutions
Fat
When fats are mixed in the same infusion bag with the CHO and amino acids, the solution is referred to as a total nutrient admixture (TNA) or a 3 : 1 solution (all three nutrient components in one bag). The IVFE may be given piggyback into the amino acid/dextrose infusion to infuse over 8-12 hr. The amount of IVFE administered may be reduced or removed for patients who have hypertriglyceridemia (e.g., patients receiving antirejection medication following organ transplant, coronary artery disease, pancreatitis, acquired immunodeficiency syndrome [AIDS]). Determine whether patient has an egg allergy because long-chain triglycerides in IVFEs may originate from phospholipids in egg yolks. If a patient develops a rash during IVFE infusion, consider an allergy immediately. If the ratio of the protein, CHO, and IVFE in the admixture is not stable, separation of the intravenous fats from the emulsion may occur and is called “cracking” of the solution. The intravenous fats may float on top of the mixture much like an egg yolk floating in the solution or appear as an uneven yellow consistency. In addition, “oiling out” may occur and looks like an oil slick or oil droplets on top of the solution. Return to the pharmacy any solution that appears “different,” and do not use it.
BOX 13-3 presents guidelines for administration of TPN.
BOX 13-3 GENERAL NURSING CARE GUIDELINES FOR THE ADMINISTRATION OF TOTAL PARENTERAL NUTRITION
 Use a 0.22-µm filter on all solutions containing amino acids and dextrose; use a 1.2-µm filter with all solutions containing amino acids, dextrose, and IVFEs. The purpose of the filter is to reduce infusion of crystals that may form from the interaction between calcium and phosphorus in the admixture. In addition, the 0.22-µm filter removes bacteria that may be in the infusion or IV system.
Use a 0.22-µm filter on all solutions containing amino acids and dextrose; use a 1.2-µm filter with all solutions containing amino acids, dextrose, and IVFEs. The purpose of the filter is to reduce infusion of crystals that may form from the interaction between calcium and phosphorus in the admixture. In addition, the 0.22-µm filter removes bacteria that may be in the infusion or IV system. The total number of calories initiated is determined by a person trained in nutritional therapy (RN, RD, or RPh) and is based on patient’s metabolic and nutritional status.
The total number of calories initiated is determined by a person trained in nutritional therapy (RN, RD, or RPh) and is based on patient’s metabolic and nutritional status. IV push administration of D50 or infusion of D10W is not required with an interruption in the infusion.
IV push administration of D50 or infusion of D10W is not required with an interruption in the infusion. Monitor for hyperglycemia.
Monitor for hyperglycemia. Nondiabetic: q6h for 24-48 hr, then discontinue if no signs of glucose intolerance have occurred. If the individual is glucose-intolerant, advance bedside assessment to q4h, and begin administration of sliding scale insulin as prescribed.
Nondiabetic: q6h for 24-48 hr, then discontinue if no signs of glucose intolerance have occurred. If the individual is glucose-intolerant, advance bedside assessment to q4h, and begin administration of sliding scale insulin as prescribed.Selection of administration site
Peripheral venous catheter
Reserved for individuals with a need for nutritional support for short-term periods, with small nutritional requirements, and for whom CVC access is unavailable. Only a low-osmolarity solution (less than 800 mOsm/L) can be used. To reduce osmolarity of the base solution, dilution of the components is usually required. The required large volume limits the type of patients in whom this admixture can be administered. (If unsure or if information is unavailable on the infusion container related to infusion route, consult with a pharmacist or refer to hospital policy.)
See TABLE 13-4 for types of CVCs used for administration of parenteral nutrition. TABLE 13-5 presents guidelines for management of catheter complications.
TABLE 13-4 TYPES OF CENTRAL VENOUS CATHETERS USED FOR ADMINISTERING PARENTERAL NUTRITION
| CATHETER | DESCRIPTION |
|---|---|
| Temporary | |
| Multilumen | May have up to 4 lumens; dedicate 1 lumen (preferably distal) for administration of TPN; may be inserted by physician at the bedside |
| PICC | May be single or dual lumen; may be used for home TPN administration because catheter may remain in place for several months; may be placed by either RN trained in IV catheter insertions or physician (usually radiologist) |
| Permanent | |
| Right atrial | Placed by physician, usually surgically, into subclavian or jugular vein with catheter tunneled and exiting from the skin; the catheter usually contains a Dacron cuff from which the catheter exits the vessel; this catheter is associated with the lowest infection rate of all central venous catheters |
| IVAD | May be placed in either radiology department or OR; designed for repeated access over a long period, thus making repeated venipunctures unnecessary |
IV, Intravenous; IVAD, implantable venous access device; OR, operating room; PICC, peripherally inserted central venous catheter; RN, registered nurse; TPN, total parenteral nutrition.
TABLE 13-5 MANAGEMENT OF CATHETER COMPLICATIONS IN PATIENTS RECEIVING PARENTERAL NUTRITION
| POTENTIAL COMPLICATION | MANAGEMENT STRATEGY |
|---|---|
| Infection: insertion site | Maintain occlusive, dry dressing |
| Change dressing per institutional policy using sterile technique | |
| When drainage appears at insertion site, change the dressing immediately | |
| Culture the drainage prn | |
| Remember: Patients who are neutropenic will develop redness at catheter insertion site because of their decrease in neutrophils | |
| Infection: bacteremia | Observe temperature curve for signs/symptoms of increase |
| Monitor for chills, rigor, tachycardia | |
| Maintain occlusive, dry dressing; change per institutional policy using sterile technique | |
| If prescribed, obtain blood cultures: one from catheter and one from a peripheral site to differentiate whether the organism is from the catheter or another site within patient | |
| Restrict blood drawing from lumen used for TPN administration | |
| Maintain blood glucose within normal limits | |
| Change IV caps on each lumen per hospital policy | |
| Use only Luer-Lok connections | |
| Have extra skin prep, sterile supplies available for physician during insertion of a temporary catheter | |
| Catheter occlusion | Flush routinely using positive pressure and saline solution before and after each piggyback infusion and blood drawing; if the catheter manufacturer recommends heparin, use a heparinized solution following saline administration; if an individual develops HIT, eliminate all heparin products from IV lines, even in catheters whose manufacturer recommends using heparin |
| Maintain IV filter to reduce infusion of any crystals that may have formed during admixture process | |
| Do not try to push occlusion through the catheter | |
| Notify physician | |
| Leakage or catheter puncture | Do not insert needles into lumen cap |
| Notify physician immediately if this occurs and prepare for changing of catheter (if temporary catheter) or repair of catheter (if right atrial catheter) | |
| Pneumothorax | Position rolled towel under patient’s back, parallel to the spine, before physician inserts temporary catheter |
| Obtain chest x-ray film after inserting catheter and before using catheter (except in an emergency) | |
| Listen for breath sounds bilaterally | |
| Evaluate for onset of acute chest pain that occurred with catheter insertion | |
| Evaluate for ear pain on the side of attempted insertion | |
| Assess for dyspnea or shortness of breath | |
| Remember: The greater the number of attempts for insertion, the greater the chance of a pneumothorax | |
| Air embolism | Examine catheter to determine whether an open port has enabled entry of air into circulatory system |
| Clamp catheter if open to air | |
| Turn patient onto left side with head down and feet up | |
| Immediately notify physician of this medical emergency after positioning patient correctly | |
| Administer oxygen as prescribed | |
| CVC thrombosis with upper extremity DVT | Assess any swelling of upper extremities, noting skin color, size of extremity, presence or absence of pulses |
| Notify physician of upper extremity size change | |
| Elevate extremity | |
| Evaluate need for removal of CVC | |
| Administer anticoagulation therapy as prescribed | |
| Monitor laboratory parameters per agency policy to assess results of anticoagulation therapy, if indicated | |
| Pulmonary thromboembolism | Evaluate for presence of pleuritic pain |
| Assess for predisposing factors such as surgery, high estrogen states (pregnancy or use of birth control pills), history or presence of malignancy, trauma, immobilization, presence of CVC, heart failure, spinal cord injury, history of previous thromboembolic disease, history of hypercoagulable states, history of hematologic conditions (e.g., polycythemia vera), nephritic syndrome, inflammatory bowel disease | |
| Assess for dyspnea or shortness of breath, hemoptysis, cough, fever, syncope, and orthopnea | |
| Encourage use of sequential compression devices when in bed, if medically indicated | |
| Use antiembolism stockings, if medically indicated | |
| Encourage ambulation, if medically indicated | |
| Administer oxygen for hypoxemia | |
| Administer anticoagulation therapy as prescribed | |
| Monitor laboratory parameters per agency policy to assess anticoagulation therapy, if indicated | |
| Pulmonary edema | Monitor I&O, daily weights |
| Assess for frothy sputum; dyspnea, shortness of breath, cyanosis | |
| Administer oxygen as prescribed | |
| Assess need for fluid restriction |
CVC, Central venous catheter; DVT, deep vein thrombosis; HIT, heparin-induced thrombocytopenia; I&O, intake and output; IV, intravenous; prn, as needed; TPN, total parenteral nutrition.
Nursing Diagnoses and Interventions
(Related primarily to both Enteral Nutrition and Parenteral Nutrition)
less than body requirements
related to inability to ingest, digest, or absorb nutrients
Desired outcome
Patient has adequate nutrition, as evidenced by stabilization of weight at desired level or steady weight gain of 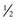 -1 lb/wk; presence of wound granulation (i.e., pinkish white tissue around wound edges; wound edges approximating together), and absence of infection (see Risk for infection, p. 715).
-1 lb/wk; presence of wound granulation (i.e., pinkish white tissue around wound edges; wound edges approximating together), and absence of infection (see Risk for infection, p. 715).
Nursing Interventions
For Enteral or Parenteral Nutrition in an Acute Care Setting
Risk for aspiration
related to GI feeding or delayed gastric emptying
Nursing Interventions
Diarrhea (or risk for same)
related to medications, dumping syndrome, bacterial contamination, or formula intolerance
Nursing Interventions
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



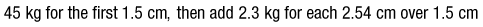
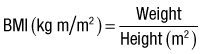
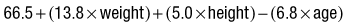
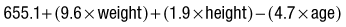
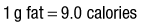














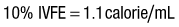
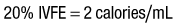
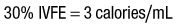








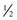 -1 hr before chest physical therapy or placing patient supine.
-1 hr before chest physical therapy or placing patient supine.