Cardiopulmonary Resuscitation, Infant
An adult who needs cardiopulmonary resuscitation (CPR) typically suffers from a primary cardiac disorder or an arrhythmia that has stopped the heart. An infant who needs CPR typically suffers from hypoxia caused by respiratory difficulty or respiratory arrest.
Most pediatric crises requiring CPR are preventable. They include motor vehicle accidents, drowning, burns, smoke inhalation, falls, poisoning, suffocation, and choking (usually from inhaling liquids).1 Other causes of cardiopulmonary arrest in infants include laryngospasm and edema from upper respiratory infections and sudden infant death syndrome.
The goal of CPR is the return of spontaneous circulation.1 However, CPR techniques differ depending on whether the patient is an adult, a child, or an infant.
For CPR purposes, the American Heart Association defines a patient by age. An infant is younger than age 1; a child is age 1 to puberty.1 Survival chances improve the sooner CPR begins and the faster advanced life-support systems are implemented. No matter how speedily you undertake CPR for an infant, however, first determine whether the infant’s respiratory distress results from a mechanical obstruction or an infection, such as epiglottiditis or croup. Epiglottiditis or croup requires immediate medical attention, not CPR. CPR is appropriate only when the infant isn’t breathing.1
Equipment
Backboard or other hard surface ▪ gloves ▪ Optional: disposable infant-size airway equipment.
Implementation
Gently tap the foot of the apparently unconscious infant and call out his name.
Put on gloves, if available, to prevent exposure to potentially infectious blood and body fluids.
For a sudden, witnessed collapse, call for help or call emergency medical service. If you didn’t witness the collapse, perform resuscitation measures for 2 minutes; then call for help.1
Place the infant supine on a hard surface.
Restoring Heartbeat and Circulation
Assess the infant’s pulse by palpating the brachial artery located inside the infant’s upper arm between the elbow and the shoulder (as shown below).1 Take no more than 10 seconds to try to find a pulse. If you find a pulse and the pulse is greater than or equal to 60 beats/minute, continue rescue breathing but don’t initiate chest compressions.1
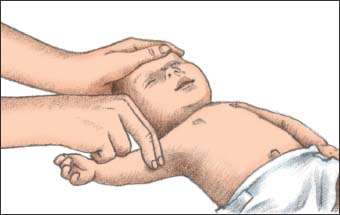
Begin chest compressions if you find no pulse or the pulse rate is less than 60 beats/minute with signs of poor perfusion. Place two fingers on the sternum just below the nipple line (as shown below). Use these two fingers to depress the sternum at least a third of the depth of the chest at 100 compressions per minute.1 When performing chest compressions, take care to ensure smooth motions. Keep your fingers on the infant’s chest at all times. Time your motions so that the compression and relaxation phases are equal to promote effective compressions.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Get Clinical Tree app for offline access
