By working together using Improvement Science, we can rebuild our health care system.
After completing this chapter, you should be able to:
• Define quality standards in health care management.
• Describe the history and evolution of quality in health care.
• Define and discuss core measures.
• Identify the role of regulatory agencies in health care quality.
• Discuss the use of key indicators to measure performance.
• Describe your role in quality and performance improvement.
• Identify tools and processes for continuous quality improvement.
• Identify the role of regulatory standards and agencies.
• Incorporate successful process improvement strategies.
• Consider the value and requirements of quality credentialing.
• Synthesize understanding of the QSEN Initiative, Healthy People 2020, and The Joint Commission National Patient Safety Goals in developing a safe patient care environment.
You may wonder why nurses need to know about quality issues to provide patient care. All nurses know that an important part of their professional life is to provide high-quality care. However, many new graduates soon discover that not all nurses do the right thing all the time for the patient and family. In fact, a landmark study in 1999, called The Quality Chasm, estimated that the impact of poor-quality care results in almost 100,000 deaths annually in acute care settings alone. Because of the costly effects of poor care, nurses need to understand their important role in ensuring quality patient care and the actions they can take to ensure excellence. According to the Institute of Medicine (2011), the enactment of the Affordable Care Act requires nurses to play a key role in transforming health care to provide higher quality and safer care than ever before and to be involved at every level to redesign the system to improve the quality of care. As managers and providers of care, nurses can be a large part of changing health care delivery to be safer and more efficient.
Issues that are on the forefront of news will take precedence over those that are routine or commonplace. Recently, medical errors have become of primary concern. Quality-assurance departments have the job of helping nurses and health care team members avoid errors by implementing various prevention methods. They also ask for the help of nurses in mobilizing process improvement teams that work to identify risk areas and develop prevention plans. Quality care can be likened to fire prevention instead of firefighting. Illegible handwriting continues to contribute to errors and has led to regulations about what medical abbreviations are appropriate. (See Table 11.1, The Joint Commission Official “Do Not Use” List of Abbreviations.)
Hospital leaders implemented quality improvement programs starting in the early 1980s with the inception of the National Demonstration Project on Quality Improvement in Healthcare, which we know today as the Institute for Healthcare Improvement (IHI, 2016). In the late 1980s, the topic of human immunodeficiency virus (HIV) and hepatitis B virus caused an increased use of gloves to prevent the transmission of infection. The increased need for more gloves led to a need to produce them quickly, which resulted in the introduction of foreign supplies of latex gloves. More latex allergies surfaced. In the 1990s, more emphasis was placed on using needleless systems to prevent needle stick injuries, resulting in legislation to increase the number of needleless devices used. In the 2000s, there has been concern and controversy regarding the nursing shortage and access to health care. In the 2010s, increasing demands will continue for all health care providers, with the expectation of high-quality care. As knowledge development increases, new technologies and treatments mean that health care providers will need to develop quality initiatives to ensure patients receive the most effective and efficient care.
Standards of Quality Health Care Management
Several agencies have established standards that guide quality in health care. Some of these include the American Nurses Association (ANA) Standards of Nursing Care, accrediting group standards such as those of The Joint Commission (TJC), which accredits health care organizations, and the Agency for Healthcare Research and Quality (AHRQ), which has established clinical practice treatment guidelines designed to improve patient outcomes and reduce costs. In addition, another national program to ensure quality health care for the country is the Healthy People initiative. The current version of the initiative is called Healthy People 2020.
First outlined in 1979, a report by the U.S. Surgeon General outlined the needs of the nation for improved health. Healthy People 2020 contains more than 1200 objectives, with each objective having a reliable data source, baseline measures, and a specific target for improvement by 2020. The objectives were prepared by experts from multiple federal agencies and made available for public comment. Agencies that support health care research often use the objectives to identify research priorities. Nursing intervention research funding requests using the Healthy People 2020 objectives are often more likely to be awarded if all other aspects are equal.
Based on the population objectives, 12 Leading Health Indicators were identified. These indicators are used to determine whether objectives are being met or not. The data are collected over 10 years and used to update and improve the objectives for the upcoming 10 years. Major improvements in population health have been made based on this work; however, the 2010 data demonstrated the need for continued improvement (U.S. Department of Health and Human Services, 2016).
TJC is an accrediting agency that evaluates care in an organization and then determines whether the overall care meets quality care standards. TJC requires hospitals to submit error reports and identifies key “sentinel events” that have the potential for great harm and publishes a monthly sentinel event alert. A sentinel event is an unexpected occurrence involving death or loss of limb or function. Such events are called “sentinel,” because they sound a warning of the need for immediate investigation and response (Fig. 22.1) (The Joint Commission, 2016a).
Without continual growth and progress, such words as improvement, achievement, and success have no meaning.
Benjamin Franklin
What Is Root Cause Analysis?
When errors occur, the primary cause needs to be determined so that a solution can be found. Root cause analysis (RCA) is a process designed for use in investigating and categorizing the root causes of events that occur. In the health care setting, there are many factors that can contribute to the cause of errors. Rather than placing blame on any one person or thing, RCA, when conducted appropriately, can identify all factors leading to the error. A hospital’s risk management department often conducts an RCA, and the results are presented to the quality improvement (QI) department for follow-up action. The role of the QI department is to be proactive at finding ways to prevent similar incidents from occurring.
Imagine an occurrence during which a nurse administers the wrong dose of a medication instead of the correct dose. In the past, the nurse (who was viewed as the last person between the medication and the patient) had sole responsibility for medication delivery. RCA has demonstrated that errors are often the result of a complex, broken system. Remedies in the past for “nurse” errors was education and sometimes discipline. RCA has shown the health care industry that medication delivery is a very complex process, and there are many things that contribute to a medication error. System issues, which are often a cause for errors that impact the delivery of medication, can be detected using the RCA process. Many things contribute to medication errors, as nurses encounter problems within the system, work-design problems, or human and environmental factors. Considering this, getting medications to the nursing unit, or medication labeling may pose medication delivery challenges.
Common causes of medication errors include wrong-dose errors, lack of drug knowledge, rule violations, carelessness, memory lapses, inadequate monitoring, misuse of infusion pumps, faulty-dose checking and failure to identify the correct drug, medication stocking problems, and using the wrong technique. System failures include lack of easy access to drug information, look-alike packaging, sound-alike drug names, transcription errors, lack of patient information, poor communication, distractions, interruptions, and excess workloads (Pape, 2003; Ehsani et al., 2013). The environment plays a part because of the many distractions the nurse must attend to in clinical practice.
The environment is as much a part of the system as are the processes within the organization. Nurses are often interrupted as they prepare medications for their patients. Sometimes the lighting is bad, or there is a great deal of noise and confusion that can distract a nurse. Technology can be helpful and is an integral part of the system components, but it cannot address the human factors and issues. Therefore, each aspect of medication errors should be considered when evaluating a cause-and-effect relationship of medication errors (Pape, 2006; U.S. Department of Health and Human Services, 2015).
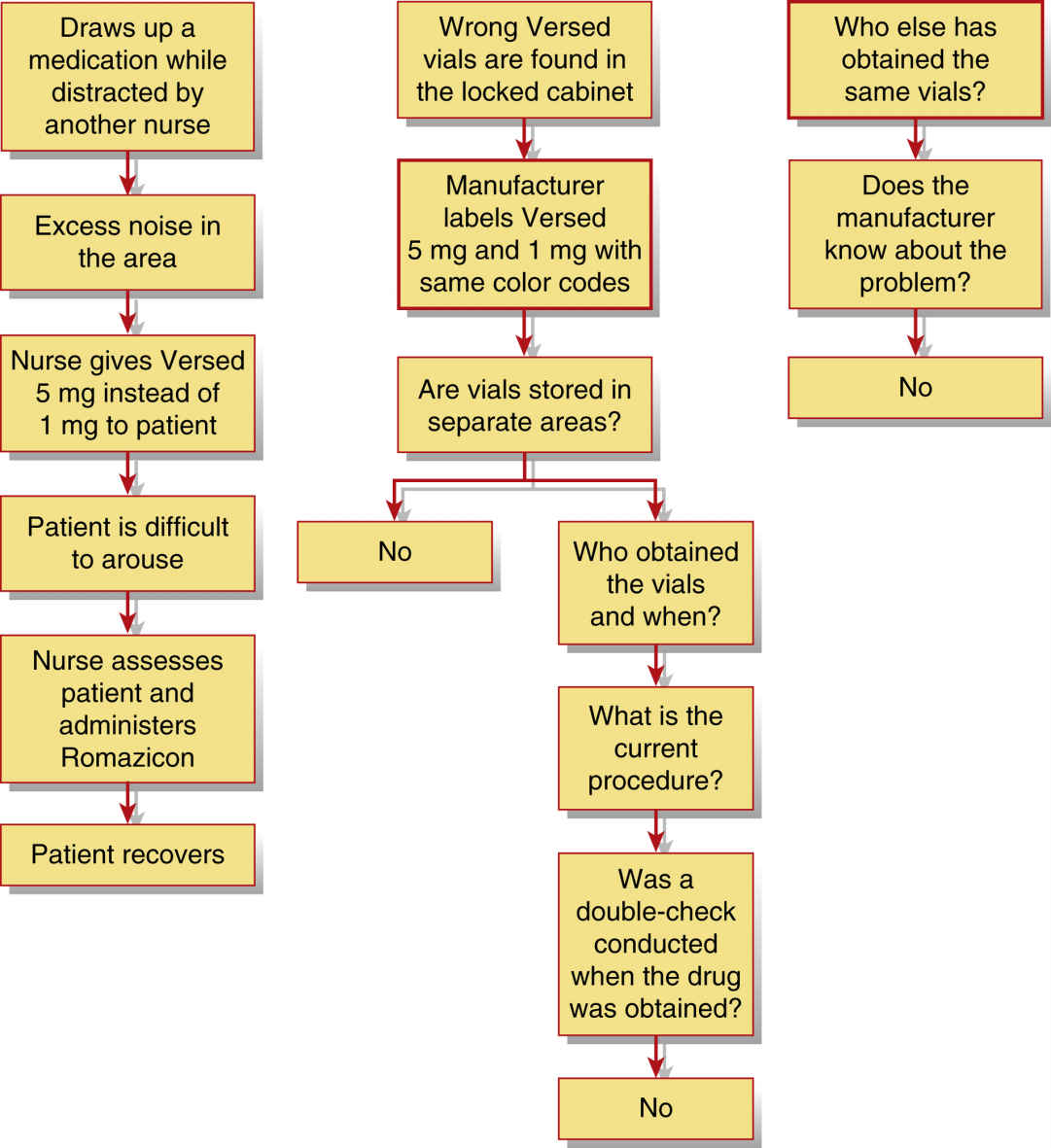
A root cause factor flow diagram should be generated to find the real origin of the error. As an example, Fig. 22.2 depicts a simplified version of the root cause analysis performed. As the investigation proceeded, it became evident that a look-alike vial meant that the nurse was not entirely at fault. In addition, distractions and hurriedness also contributed to the error.
History and Evolution of Quality in Health Care
The advent of quality in health care began when hospitals found the need to look outside their own expertise for error prevention strategies. The year is not as important as the fact that health care organizations found a need to borrow from other industries that were successful at managing risk. Manufacturing industries began focusing on error prevention in the early 1920s, whereas the evolution of improved quality techniques in health care was not adopted until the 1960s, and quality techniques are still evolving.
Historically, the focus of quality improvement was in controlling processes by inspection so that errors were prevented. Later, the emphasis changed from inspection to proactive approaches to error prevention. Included with prevention are monitoring processes to control errors.
Who Are Edward Deming, Joseph M. Juran, and Philip Crosby?
Edward Deming is often considered the father of quality improvement, although quality concepts have developed and improved throughout several decades. What once began simply as a method for discovering how to prevent defects has evolved into highly skilled methods for tracking and improving quality today. Deming’s teachings embraced the philosophy that quality is everyone’s responsibility within an organization.
Another valuable forefather of quality initiatives is Joseph M. Juran, who emphasized the meaning of the Pareto principle. The Pareto principle states that 80% of problems are caused by 20% of sources, people, or things. Therefore if you can fix the 20%, you can fix almost the entire system. Juran’s work marked the beginning of the idea of total quality management (TQM).
Philip Crosby is considered the father of zero defects. He often proposed simplifying things so that everyone could understand. He also believed in the importance of communicating quality efforts and their results to the entire organization. Afterward, ideas such as “lean” manufacturing, “just-in-time” product delivery, and “Six Sigma” methods crossed over into health care.
Recently, there has been a real change in how members of the health care team view quality improvement within health care settings. What once was considered work only for the QI department is now brought to the frontline workers, who can best affect the outcomes. By frontline workers, we mean the nurses at the bedside and other workers in direct patient care areas who know the problems that need to be resolved. This is also termed Improvement Science. An ongoing commitment to improvement strategies supports an atmosphere of teamwork. The focus is on the process and systems rather than on blaming individuals (Fig. 22.3).
Still, the regulation of health care is conducted at the national level by regulatory governmental bodies. These government agencies are responsible for approving many of the licenses for educational institutions that educate personnel. An example of a government agency that regulates nursing is state boards of nursing. Institutional accreditation is also conducted by some government agencies such as the public health department.
As mentioned earlier, TJC, previously called JCAHO, is the primary agency used for hospital accreditation. The mere mention of a visit by TJC can elicit feelings of fear and anxiety in the minds of nurses and hospital administrators. This is because hospitals must meet certain quality standards to pass TJC’s inspections to maintain accreditation, and achieving accreditation is required to receive government funding for the health care provided. In the 1990s, TJC first began to mandate the use of continuous quality improvement (CQI) and to recommend that organizations adopt a quality improvement model for all process improvement activities. TJC typically endorses the use of the plan–do–study–act cycle (PDSA) as one tool for process improvement.
Some hospital QI departments have combined newer strategies with PDSA, including define–measure–analyze–improve–control (DMAIC) and rapid cycle changes (RCCs), which further incorporate a team focus. These are components of CQI, but more discussion of these methods will come later. TJC has also mandated specific quality outcome measures for all hospitals. Outcome measures mean looking for real patient results to determine whether the organization’s goals were achieved. TJC wants to know if the care that patients receive is meeting standards or is improving.
What are Core Measures?
Core measures include those for patients admitted with a diagnosis of acute myocardial infarction, congestive heart failure, community-acquired pneumonia, surgical-infection prophylaxis, pregnancy-related conditions, deep vein thrombosis, and whether specific best practices were implemented within the health care setting. These measures are those that the public consumer considers important for choosing one hospital over another.
Hospitals must continue to assess the core measures that were developed by TJC. There are 13 core measure sets (Acute Myocardial Infarction, Children’s Asthma Care, Emergency Department, Hospital Outpatient Department, Hospital-Based Inpatient Psychiatric Services, Immunization, Perinatal Care, Pneumonia Measures, Stroke, Substance Use, Surgical Care Improvement Project [SCIP], Tobacco Treatment, and Venous Thromboembolism), as defined by The Joint Commission (2016b). The goal is to improve the quality of health care by implementing a national standardized performance measurement system. Key actions are listed in each category that define the best research-based care process that is appropriate for that category. By tracking these core measures, hospitals improve patient care by focusing on the results of that care.
In 2011, the Centers for Medicare and Medicaid Services (CMS) launched the Medicare Shared Savings Plan, as a requirement by the Patient Protection and Affordable Care Act, to assist all health care providers across health care settings (hospitals, doctor’s offices, long-term care settings) in coordinating care for Medicare patients. Under the Medicare Shared Savings Plan, Accountable Care Organizations (ACOs), consisting of health care providers, agree to collaborate in providing patient care, versus working independently in an effort to control costs and provide quality patient care. In order for an ACO to receive financial benefits of services rendered to a Medicare patient from CMS, the ACO must demonstrate that it has met the performance standard(s) as set forth by CMS (Centers for Medicare & Medicaid Services, 2015a, p.1). There are currently 33 quality measures divided into 4 categories. This information is available from the CMS website at cms.gov (Centers for Medicare & Medicaid Services, 2016a).
What is HCAHPS?
HCAHPS refers to the Hospital Consumer Assessment of Healthcare Providers and Systems. It is a national program for collecting and providing health care information from the consumer perspective, and the results are used to improve health care services. The patient survey was developed for public reporting as a way to compare hospitals across the continuum of patient care and garner information about the overall quality of care received from the patient’s viewpoint. The HCAHPS contains ratings of communication, responsiveness, pain management, discharge information, cleanliness of the hospital environment, quietness of the hospital environment, and if patients would recommend the hospital (HCAHPS, 2014).
What is Hospital Compare?
The Hospital Compare website is designed so consumers can compare how well selected hospitals serve to provide the care recommended to their patients. This information is provided through the efforts of Medicare and the Hospital Quality Alliance so consumers make informed decisions about health care. The performance measures that can be compared include information related to heart attack, heart failure, pneumonia, surgery, and other conditions (Centers for Medicare & Medicaid Services, 2015b). Consumers can go to www.hospitalcompare.hhs.gov and search by zip code to compare hospitals and prescribers.
Just What is the Joint Commission?
TJC is the major accrediting body for health care institutions that are funded by Medicare and Medicaid. The CMS is a part of the U.S. Department of Health and Human Services. Both organizations set the standards for safe practice and evaluate compliance. Having TJC accreditation symbolizes the organization’s commitment to quality. This means that nearly all hospitals must be TJC accredited to stay in business.
In the past, TJC standards have directly addressed patient safety in many areas. Beginning on July 1, 2001, additions to these standards required hospitals to develop a systematic approach to error reduction and to design patient care processes with safety in mind. For CQI initiatives, TJC recommends using things such as flow charts, Pareto charts, run charts or line graphs, control charts, and histograms to display data. We call these “tools” or “instruments,” because they help depict the measurements and track the problems and improvements. After the data have been collected, these tools help visualize results of performance improvement understood by most nurses. Other valuable tools are discussed later.
What Are Patient Safety Goals?
A primary driving force for CQI activities is TJC’s National Patient Safety Goals (NPSG). In 2001, TJC began instituting annual patient safety goals intended to improve the quality of health care. The hospital national patient safety goals are summarized in Box 22.1 (The Joint Commission, 2016c).
TJC’s Board of Commissioners approved the first NPSGs in July 2002. TJC established these goals to help accredited organizations address specific areas of concern regarding patient safety. Each goal includes brief, evidence-based recommendations. Evidence-based means the goals are based on real-world research and/or expert opinions. Each year, the goals and associated recommendations are reevaluated; most are continued and others may be replaced because of emerging new priorities or evidence from research studies. New goals and recommendations are announced in July and become effective on January 1 of the following year (TJC, 2016c); for more information on the NPSGs for specific organizations, one can access TJC’s website.
Monitoring the Quality of Health Care
It is important for nurses to know how to design and conduct simple quality improvement projects to improve processes within their nursing units. Nurses need to know the basics of collecting and analyzing data and what to do with the results. They must be able to educate other nurses about performance improvement as well.
What Is Quality Improvement?
QI refers to the process or activities that are used to measure, monitor, evaluate, and control services, which will lead to measurable improvement to health care consumers. It includes reports that must be generated to track progress. Incidence reports are sometimes referred to as QI reports or variance reports. These help guide the hospital risk management (RM) department and QI department to make system improvements (Box 22.2).
How Do We Monitor Quality?
As stated earlier, someone must monitor quality care compliance to continuously maintain and improve standards of practice. The QI department is typically the department that receives data, analyzes trends, and recommends actions to facilitate improvement in the organization. However, there should also be a CQI Council as a primary decision-making nursing team, as well as quality circles (QCs) that function along service lines, collaborating to improve care for a group of patient types.
Examples of service lines include surgical units, medical units, neurologic units, rehabilitation units, and outpatient units. These teams of nurses and other staff review specific problems or indicators each month to determine whether quality care is being delivered. The goal is to keep patients safe by encouraging everyone to practice according to established standards. Each service line provides an annual quality plan for the following year, based on recent problem areas or hot topics identified. Because it is impossible to track everything that nurses consider important to quality care, QCs use various methods to prioritize or target their reviews. They establish unit-specific quality indicators for tracking problems on the nursing unit using measurable questions that provide data for trending improvements.
What Is an Indicator and a Metric?
A quality indicator is an item of concern that has arisen because of a nursing practice problem. It is often an RM as well. For example, a quality team may have identified a problem with securing urethral catheters properly. This seems to be a recurrent issue. Perhaps several patients had urethral catheters that were inadvertently pulled out. After some investigation and collecting baseline data, the problem was identified as having to do with not securing the catheters properly. Thus the team will collect data for a specific time and will track the nurses’ practices. They would count the number of urethral catheters not secured correctly and divide that by the total number of urethral catheters during a specific time frame to obtain the average rate of compliance. The metric or measure is the actual rate of urethral catheters that are secured properly (Table 22.1). The correct practice would be clarified with all nurses according to an established policy. Later, when most of the nurses were securing urethral catheters correctly, there may not be a need to monitor this particular practice any longer. In essence, the indicator is the problem, and the metric is the measurement of that problem.
A unit-based QI nurse is usually assigned the responsibility to audit charts or to verify a procedure by direct observation to determine compliance with a specific nursing practice. The results are compiled and sent to the QI department. After nurses are re-educated about the correct practice, the same indicator is tracked for several months to see whether there has been an improvement. This is done until noncompliance reaches pre-established criteria (e.g., below 5%) and/or compliance is 95%.
Indicators are sometimes selected based on an RM issue. For example, a patient may have suffered an injury because a catheter was not secured correctly. The critical thinking exercise (Critical Thinking Box 22.1) can help you discover another example of how important chart auditing can be.
Table 22.1 shows some examples of metrics. Metric descriptors contain more detailed information about what is to be measured and what is not measured. For example, if bedside nurses were measuring the rate of IV tubing labeled according to policy, they would further define what type of IV tubing is used. Further exploration would determine whether data should include only primary IV lines or both primary and piggyback lines. Most likely, the metrics would include both, but it is always best to be specific about what is to be counted. TJC surveyors typically look at these details.